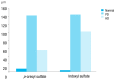
p-Cresyl sulfate and indoxyl sulfate in pediatric patients on chronic dialysis
- PMID: 23646054
- PMCID: PMC3641312
- DOI: 10.3345/kjp.2013.56.4.159
p-Cresyl sulfate and indoxyl sulfate in pediatric patients on chronic dialysis
Abstract
Purpose: Indoxyl sulfate and p-cresyl sulfate are important protein-bound uremic retention solutes whose levels can be partially reduced by renal replacement therapy. These solutes originate from intestinal bacterial protein fermentation and are associated with cardiovascular outcomes and chronic kidney disease progression. The aims of this study were to investigate the levels of indoxyl sulfate and p-cresyl sulfate as well as the effect of probiotics on reducing the levels of uremic toxins in pediatric patients on dialysis.
Methods: We enrolled 20 pediatric patients undergoing chronic dialysis; 16 patients completed the study. The patients underwent a 12-week regimen of VSL#3, a high-concentration probiotic preparation, and the serum levels of indoxyl sulfate and p-cresyl sulfate were measured before treatment and at 4, 8, and 12 weeks after the regimen by using fluorescence liquid chromatography. To assess the normal range of indoxyl sulfate and p-cresyl sulfate we enrolled the 16 children with normal glomerular filtration rate who had visited an outpatient clinic for asymptomatic microscopic hematuria that had been detected by a school screening in August 2011.
Results: The baseline serum levels of indoxyl sulfate and p-cresyl sulfate in the patients on chronic dialysis were significantly higher than those in the children with microscopic hematuria. The baseline serum levels of p-cresyl sulfate in the peritoneal dialysis group were significantly higher than those in the hemodialysis group. There were no significant changes in the levels of these uremic solutes after 12-week VSL#3 treatment in the patients on chronic dialysis.
Conclusion: The levels of the uremic toxins p-cresyl sulfate and indoxyl sulfate are highly elevated in pediatric patients on dialysis, but there was no significant effect by probiotics on the reduction of uremic toxins in pediatric dialysis patients. Therefore, studies for other medical intervention to reduce uremic toxins are also necessary in pediatric patients on dialysis.
Keywords: Children; Chronic dialysis; Indoxyl sulfate; Probiotics; p-Cresyl sulfate.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
Similar articles
-
Protein-bound uremic toxin lowering strategies in chronic kidney disease: a systematic review and meta-analysis.J Nephrol. 2021 Dec;34(6):1805-1817. doi: 10.1007/s40620-020-00955-2. Epub 2021 Jan 23. J Nephrol. 2021. PMID: 33484425
-
Correlation between Serum Levels of Protein-Bound Uremic Toxins in Hemodialysis Patients Measured by LC/MS/MS.Mass Spectrom (Tokyo). 2013;2(Spec Iss):S0017. doi: 10.5702/massspectrometry.S0017. Epub 2013 Apr 15. Mass Spectrom (Tokyo). 2013. PMID: 24349936 Free PMC article.
-
Removal of Protein-Bound Uremic Toxins during Hemodialysis Using a Binding Competitor.Clin J Am Soc Nephrol. 2019 Mar 7;14(3):394-402. doi: 10.2215/CJN.05240418. Epub 2019 Feb 12. Clin J Am Soc Nephrol. 2019. PMID: 30755453 Free PMC article.
-
The effect of isohydric hemodialysis on the binding and removal of uremic retention solutes.PLoS One. 2018 Feb 22;13(2):e0192770. doi: 10.1371/journal.pone.0192770. eCollection 2018. PLoS One. 2018. PMID: 29470534 Free PMC article.
-
Molecular mechanisms underlying uremic toxin-related systemic disorders in chronic kidney disease: focused on β2-microglobulin-related amyloidosis and indoxyl sulfate-induced atherosclerosis-Oshima Award Address 2016.Clin Exp Nephrol. 2019 Feb;23(2):151-157. doi: 10.1007/s10157-018-1588-9. Epub 2018 Jun 5. Clin Exp Nephrol. 2019. PMID: 29869756 Free PMC article. Review.
Cited by
-
Gut microbiota and chronic kidney disease: evidences and mechanisms that mediate a new communication in the gastrointestinal-renal axis.Pflugers Arch. 2020 Mar;472(3):303-320. doi: 10.1007/s00424-020-02352-x. Epub 2020 Feb 17. Pflugers Arch. 2020. PMID: 32064574 Review.
-
p-Cresyl Sulfate.Toxins (Basel). 2017 Jan 29;9(2):52. doi: 10.3390/toxins9020052. Toxins (Basel). 2017. PMID: 28146081 Free PMC article. Review.
-
The Role of the Gut Microbiota in Complications among Hemodialysis Patients.Microorganisms. 2024 Sep 12;12(9):1878. doi: 10.3390/microorganisms12091878. Microorganisms. 2024. PMID: 39338552 Free PMC article. Review.
-
Gut Dysbiosis and the Intestinal Microbiome: Streptococcus thermophilus a Key Probiotic for Reducing Uremia.Microorganisms. 2019 Jul 31;7(8):228. doi: 10.3390/microorganisms7080228. Microorganisms. 2019. PMID: 31370220 Free PMC article. Review.
-
The effects of probiotic supplement on hemoglobin in chronic renal failure patients under hemodialysis: A randomized clinical trial.J Res Med Sci. 2017 Jun 21;22:74. doi: 10.4103/jrms.JRMS_614_16. eCollection 2017. J Res Med Sci. 2017. PMID: 28717371 Free PMC article.
References
-
- Vanholder R, De Smet R, Glorieux G, Argiles A, Baurmeister U, Brunet P, et al. Review on uremic toxins: classification, concentration, and interindividual variability. Kidney Int. 2003;63:1934–1943. - PubMed
-
- Vanholder R, De Smet R. Pathophysiologic effects of uremic retention solutes. J Am Soc Nephrol. 1999;10:1815–1823. - PubMed
-
- Fagugli RM, De Smet R, Buoncristiani U, Lameire N, Vanholder R. Behavior of non-protein-bound and protein-bound uremic solutes during daily hemodialysis. Am J Kidney Dis. 2002;40:339–347. - PubMed
-
- Jourde-Chiche N, Dou L, Cerini C, Dignat-George F, Vanholder R, Brunet P. Protein-bound toxins: update 2009. Semin Dial. 2009;22:334–339. - PubMed
-
- Meyer TW, Hostetter TH. Uremia. N Engl J Med. 2007;357:1316–1325. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical