Ipsilateral motor pathways after stroke: implications for non-invasive brain stimulation
- PMID: 23658541
- PMCID: PMC3647244
- DOI: 10.3389/fnhum.2013.00184
Ipsilateral motor pathways after stroke: implications for non-invasive brain stimulation
Abstract
In humans the two cerebral hemispheres have essential roles in controlling the upper limb. The purpose of this article is to draw attention to the potential importance of ipsilateral descending pathways for functional recovery after stroke, and the use of non-invasive brain stimulation (NBS) protocols of the contralesional primary motor cortex (M1). Conventionally NBS is used to suppress contralesional M1, and to attenuate transcallosal inhibition onto the ipsilesional M1. There has been little consideration of the fact that contralesional M1 suppression may also reduce excitability of ipsilateral descending pathways that may be important for paretic upper limb control for some patients. One such ipsilateral pathway is the cortico-reticulo-propriospinal pathway (CRPP). In this review we outline a neurophysiological model to explain how contralesional M1 may gain control of the paretic arm via the CRPP. We conclude that the relative importance of the CRPP for motor control in individual patients must be considered before using NBS to suppress contralesional M1. Neurophysiological, neuroimaging, and clinical assessments can assist this decision making and facilitate the translation of NBS into the clinical setting.
Keywords: propriospinal; rehabilitation; stroke; transcranial direct current stimulation; upper limb.
Figures
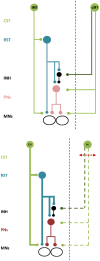
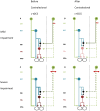
References
-
- Alstermark B., Lundberg A., Sasaki S. (1984). Integration in descending motor pathways controlling the forelimb in the cat. 12. Interneurones which may mediate descending feed-forward inhibition and feed-back inhibition from the forelimb to C3-C4 propriospinal neurones. Exp. Brain Res. 56, 308–32210.1007/BF00236285 - DOI - PubMed
-
- Ameli M., Grefkes C., Kemper F., Riegg F. P., Rehme A. K., Karbe H., et al. (2009). Differential effects of high-frequency repetitive transcranial magnetic stimulation over ipsilesional primary motor cortex in cortical and subcortical middle cerebral artery stroke. Ann. Neurol. 66, 298–30910.1002/ana.21725 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

