Histopathological correlates with survival in reoperated glioblastomas
- PMID: 23666202
- PMCID: PMC3994532
- DOI: 10.1007/s11060-013-1141-3
Histopathological correlates with survival in reoperated glioblastomas
Abstract
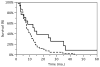
The addition of concomitant and adjuvant chemotherapy to radiation therapy after surgical resection has increased significantly the survival of patients with glioblastoma (GB). In conjunction, there has been an increasing fraction of patients who present with new enlarged areas of contrast enhancement and edema on post-treatment imaging that improve without further treatment. It remains to be established how this phenomenon, commonly termed pseudoprogression, can be distinguished from true tumor recurrence defined as the histological presence of active high-grade tumor, as well as its prognostic significance. Data for over 500 patients undergoing surgery for recurrent GB were reviewed. Pathological specimens were categorized as those that contained active high-grade glioma in any amount, and those that did not. Patient survival was compared between these two groups, and independent associations were assessed using Cox proportionate hazards regression analysis. 59 patients met the study criteria including complete pathological and follow-up data. Mean age was 53 ± 11 years. Median survival from suspected recurrence and initial diagnosis were 8 [5-14] and 20 [12-30] months. Seventeen patients (29 %) had no evidence of active high-grade tumor and 42 (71 %) had at least focal active high-grade glioma. Pathologic pseudoprogression at re-operation (p = 0.03) and gross total resection (p = 0.01) were independently associated with survival. The histopathological features defined here and used to assess the tumor at reoperation were independently associated with survival. These findings may be important in designing treatment strategies and clinical trial endpoints for patients with GB.
Conflict of interest statement
Figures



References
-
- Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005;352(10):987–996. - PubMed
-
- de Wit MC, de Bruin HG, Eijkenboom W, Sillevis Smitt PA, van den Bent MJ. Immediate post-radiotherapy changes in malignant glioma can mimic tumor progression. Neurology. 2004;63(3):535–537. - PubMed
-
- Chamberlain MC, Glantz MJ, Chalmers L, Van Horn A, Sloan AE. Early necrosis following concurrent Temodar and radio-therapy in patients with glioblastoma. J Neurooncol. 2007;82(1):81–83. - PubMed
-
- Brandsma D, Stalpers L, Taal W, Sminia P, van den Bent MJ. Clinical features, mechanisms, and management of pseudoprogression in malignant gliomas. Lancet Oncol. 2008;9(5):453–461. - PubMed
-
- Chaskis C, Neyns B, Michotte A, De Ridder M, Everaert H. Pseudoprogression after radiotherapy with concurrent temozolomide for high-grade glioma: clinical observations and working recommendations. Surg Neurol. 2009;72(4):423–428. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

