Cardiovascular complications of radiation therapy for thoracic malignancies: the role for non-invasive imaging for detection of cardiovascular disease
- PMID: 23666251
- PMCID: PMC3945797
- DOI: 10.1093/eurheartj/eht114
Cardiovascular complications of radiation therapy for thoracic malignancies: the role for non-invasive imaging for detection of cardiovascular disease
Abstract
Radiation exposure to the thorax is associated with substantial risk for the subsequent development of cardiovascular disease. Thus, the increasing role of radiation therapy in the contemporary treatment of cancer, combined with improving survival rates of patients undergoing this therapy, contributes to a growing population at risk of cardiovascular morbidity and mortality. Associated cardiovascular injuries include pericardial disease, coronary artery disease, valvular disease, conduction disease, cardiomyopathy, and medium and large vessel vasculopathy-any of which can occur at varying intervals following irradiation. Higher radiation doses, younger age at the time of irradiation, longer intervals from the time of radiation, and coexisting cardiovascular risk factors all predispose to these injuries. The true incidence of radiation-related cardiovascular disease remains uncertain due to lack of large multicentre studies with a sufficient duration of cardiovascular follow-up. There are currently no consensus guidelines available to inform the optimal approach to cardiovascular surveillance of recipients of thoracic radiation. Therefore, we review the cardiovascular consequences of radiation therapy and focus on the potential role of non-invasive cardiovascular imaging in the assessment and management of radiation-related cardiovascular disease. In doing so, we highlight characteristics that can be used to identify individuals at risk for developing post-radiation cardiovascular disease and propose an imaging-based algorithm for their clinical surveillance.
Keywords: Non-invasive imaging; Radiation therapy.
Figures
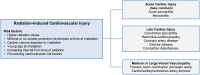

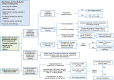
References
-
- Darby S, McGale P, Correa C, Taylor C, Arriagada R, Clarke M, Cutter D, Davies C, Ewertz M, Godwin J, Gray R, Pierce L, Whelan T, Wang Y, Peto R Early Breast Cancer Trialists’ Collaborative G. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet. 2011;378:1707–1716. - PMC - PubMed
-
- Boice JD., Jr An affair of the heart. J Natl Cancer Inst. 2007;99:186–187. - PubMed
-
- Cohn KE, Stewart JR, Fajardo LF, Hancock EW. Heart disease following radiation. Medicine (Baltimore) 1967;46:281–298. - PubMed
-
- Rademaker J, Schoder H, Ariaratnam NS, Strauss HW, Yahalom J, Steingart R, Oeffinger KC. Coronary artery disease after radiation therapy for Hodgkin's lymphoma: coronary CT angiography findings and calcium scores in nine asymptomatic patients. AJR Am J Roentgenol. 2008;191:32–37. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

