Operative and non-operative management of endoscopic retrograde cholangiopancreatography-associated duodenal injuries
- PMID: 23676815
- PMCID: PMC4132505
- DOI: 10.1308/003588413X13511609958578
Operative and non-operative management of endoscopic retrograde cholangiopancreatography-associated duodenal injuries
Abstract
Introduction: Endoscopic retrograde cholangiopancreatography (ERCP) is indispensable in everyday surgical practice. Despite this, as an invasive procedure, it has its own mortality and morbidity, the most feared of which is periduodenal perforations. Our experience with ERCP related periduodenal perforations and its treatment strategies are presented. Additionally, a rarely encountered subtype is highlighted.
Methods: Patients who underwent ERCP and sustained a periduodenal perforation between August 2008 and October 2011 were reviewed.
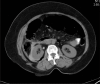
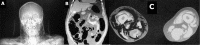
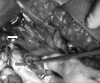
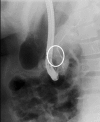
Results: During the period from August 2008 to October 2011, 597 ERCP procedures were performed in our hospital. Ten of these patients (3 male, 7 female) had a perforation. The mean patient age was 56.6 years. During the procedure, injury was suspected in four patients; it passed unnoticed in the remaining six. The decision to operate or follow a conservative policy was based on a combination of clinical and radiological findings. Operative intervention was required in three patients, with one mortality, while conservative treatment was followed in the remaining seven. A laparotomy was performed early in two patients whereas it was performed after an initial period of conservative treatment in one. The presence of periduodenal fluid collection, contrast extravasation or free intraperitoneal air were decisive factors for performing laparotomy.
Conclusions: ERCP-related periduodenal perforations include different categories. Certain types require operative repair while others should be treated conservatively. The choice of the management approach should be individualised, depending on the clinical picture and radiological findings. Although rare, these are potentially serious complications that may end fatally. Early recognition and appropriate intervention is the only way to avert a fatal outcome.
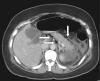
Figures

Similar articles
-
Review of duodenal perforations after endoscopic retrograde cholangiopancreatography in Hospital Puerta de Hierro from 1999 to 2014.Rev Esp Enferm Dig. 2018 Aug;110(8):515-519. doi: 10.17235/reed.2018.5255/2017. Rev Esp Enferm Dig. 2018. PMID: 29667417
-
Endoscopic Treatment of Endoscopic Retrograde Cholangiopancreatography-Related Duodenal Perforations.J Laparoendosc Adv Surg Tech A. 2019 Mar;29(3):385-391. doi: 10.1089/lap.2018.0617. Epub 2019 Jan 24. J Laparoendosc Adv Surg Tech A. 2019. Retraction in: J Laparoendosc Adv Surg Tech A. 2019 Jul;29(7):987. doi: 10.1089/lap.2018.0617.retract. PMID: 30676226 Retracted.
-
Immediate detection of endoscopic retrograde cholangiopancreatography-related periampullary perforation: fluoroscopy or endoscopy?World J Gastroenterol. 2014 Nov 14;20(42):15797-804. doi: 10.3748/wjg.v20.i42.15797. World J Gastroenterol. 2014. PMID: 25400465 Free PMC article.
-
Management of duodenal perforation post-endoscopic retrograde cholangiopancreatography. When and whom to operate and what factors determine the outcome? A review article.JOP. 2012 Jan 10;13(1):18-25. JOP. 2012. PMID: 22233942 Review.
-
[Management of perforations as adverse events of ERCP plus ES. Personal experience].G Chir. 2009 Nov-Dec;30(11-12):520-30. G Chir. 2009. PMID: 20109385 Review. Italian.
Cited by
-
CT evaluation of gastrointestinal system perforations: A retrospective comparative analysis between retroperitoneal and intraperitoneal perforation sites.Radiologie (Heidelb). 2025 Aug 24. doi: 10.1007/s00117-025-01500-7. Online ahead of print. Radiologie (Heidelb). 2025. PMID: 40851046 English.
-
Diagnosis and management of type II endoscopic retrograde cholangiopancreatography-related perforations: a multicenter retrospective study.BMC Gastroenterol. 2024 Jul 30;24(1):241. doi: 10.1186/s12876-024-03335-3. BMC Gastroenterol. 2024. PMID: 39080542 Free PMC article.
-
ERCP-induced perforation: review and revisit after half a century.F1000Res. 2024 Mar 15;12:612. doi: 10.12688/f1000research.129637.2. eCollection 2023. F1000Res. 2024. PMID: 39027921 Free PMC article. Review.
-
Stapfer I and II duodenal perforations after endoscopic procedures: how surgical delay impacts outcomes.Surg Endosc. 2024 Nov;38(11):6614-6624. doi: 10.1007/s00464-024-11232-9. Epub 2024 Sep 16. Surg Endosc. 2024. PMID: 39285044
-
Surgical versus non-operative initial management of post-endoscopic retrograde cholangiopancreatography perforation: a systematic review and meta-analysis.Ann Gastroenterol. 2022 Jan-Feb;35(1):95-101. doi: 10.20524/aog.2021.0671. Epub 2021 Oct 12. Ann Gastroenterol. 2022. PMID: 34987295 Free PMC article.
References
-
- Frakes JT. Medicolegal Issues. In: Baron TH, Kozarek RA, Carr-Locke DL, eds.ERCP. Philadelphia: Elsevier; 2008; pp3–11
-
- Christensen M, Matzen P, Schulze S, Rosenberg J. Complications of ERCP: a prospective study. Gastrointest Endosc 2004; 60: 721–731 - PubMed
-
- Ercan M, Bostanci EB, Dalgic Tet al Surgical outcome of patients with perforation after endoscopic retrograde cholangiopancreatography. J Laparoendosc Adv Surg Tech A 2012; 22: 371–377 - PubMed
-
- Krishna RP, Singh RK, Behari Aet al Post-endoscopic retrograde cholangiopancreatography perforation managed by surgery or percutaneous drainage. Surg Today 2011; 41: 660–666 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

