The Role of Diverting Stoma After an Ultra-low Anterior Resection for Rectal Cancer
- PMID: 23700573
- PMCID: PMC3659245
- DOI: 10.3393/ac.2013.29.2.66
The Role of Diverting Stoma After an Ultra-low Anterior Resection for Rectal Cancer
Abstract
Purpose: A diverting stoma is known to reduce the consequences of distal anastomotic failure following colorectal surgery. The aim of this study was to evaluate the efficacy of a diverting stoma after an ultra-low anterior resection (uLAR) for rectal cancer.
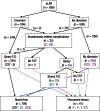
Methods: Between 2000 and 2007, 836 patients who underwent an uLAR were divided into two groups, depending on the fecal diversion: 246 received fecal diversion, and 590 had no diversion. Patient- and disease-related variables were compared between the two groups.
Results: Thirty-two of the 836 patients (3.8%) had immediate anastomosis-related complications and required reoperation. Anastomosis leakage comprised 72% of the complications (23/32). The overall immediate complication rate was significantly lower in patients with a diverting stoma (0.8%, 2/246) compared to those without a diverting stoma (5.1%, 30/590; P = 0.005). The fecal diversion group had lower tumor location, lower anastomosis level, and more preoperative chemo-radiation therapy (P < 0.001). In total, 12% of patients in the diverting stoma group had complications either in making or reversing the stoma (30/246).
Conclusion: The diverting stoma decreased the rate of immediate anastomosis-related complications. However, the rate of complications associated with the diverting stoma was non-negligible, so strict criteria should be applied when deciding whether to use a diverting stoma.
Keywords: Colorectal surgery; Ileostomy; Rectal neoplasms.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
Similar articles
-
Defunctioning loop ileostomy with low anterior resection for distal rectal cancer: should we make an ileostomy as a routine procedure? A prospective randomized study.Hepatogastroenterology. 2008 Sep-Oct;55(86-87):1562-7. Hepatogastroenterology. 2008. PMID: 19102343 Clinical Trial.
-
Diverting stomas reduce reoperation rates for anastomotic leak but not overall reoperation rates within 30 days after anterior rectal resection: a national cohort study.Int J Colorectal Dis. 2022 Jul;37(7):1681-1688. doi: 10.1007/s00384-022-04205-8. Epub 2022 Jun 24. Int J Colorectal Dis. 2022. PMID: 35739403 Free PMC article.
-
A diverting stoma is not necessary when performing a handsewn coloanal anastomosis for lower rectal cancer.Dis Colon Rectum. 2007 Jul;50(7):1040-6. doi: 10.1007/s10350-007-0233-6. Dis Colon Rectum. 2007. PMID: 17525861
-
Diverting ileostomy in colorectal surgery: when is it necessary?Langenbecks Arch Surg. 2015 Feb;400(2):145-52. doi: 10.1007/s00423-015-1275-1. Epub 2015 Jan 30. Langenbecks Arch Surg. 2015. PMID: 25633276 Review.
-
Predicting the risk and diminishing the consequences of anastomotic leakage after anterior resection for rectal cancer.Acta Chir Iugosl. 2010;57(3):47-50. doi: 10.2298/aci1003047m. Acta Chir Iugosl. 2010. PMID: 21066983 Review.
Cited by
-
Meta-analysis of defunctioning stoma in low anterior resection with total mesorectal excision for rectal cancer: evidence based on thirteen studies.World J Surg Oncol. 2015 Jan 24;13:9. doi: 10.1186/s12957-014-0417-1. World J Surg Oncol. 2015. PMID: 25617234 Free PMC article.
-
Comparison of Complications and Outcomes of Very Low Anterior Resection (VLAR) Versus Intersphentric Resection (ISR) In Patients with Rectal Cancer.World J Plast Surg. 2024;13(3):92-95. doi: 10.61186/wjps.13.3.92. World J Plast Surg. 2024. PMID: 39665004 Free PMC article.
-
Current Treatment Approaches and Outcomes in the Management of Rectal Cancer Above the Age of 80.Curr Oncol. 2021 Mar 30;28(2):1388-1401. doi: 10.3390/curroncol28020132. Curr Oncol. 2021. PMID: 33808512 Free PMC article.
-
Complications Rate and Related Factors After Laparoscopic Sphincter-Preserving Total Mesorectal Excision for Low Rectal Cancer: A Single-Center Study in Vietnam.Cureus. 2024 May 21;16(5):e60734. doi: 10.7759/cureus.60734. eCollection 2024 May. Cureus. 2024. PMID: 38774464 Free PMC article.
-
Fortune of temporary ileostomies in patients treated with laparoscopic low anterior resection for rectal cancer.Ann Surg Treat Res. 2017 Jan;92(1):35-41. doi: 10.4174/astr.2017.92.1.35. Epub 2016 Dec 30. Ann Surg Treat Res. 2017. PMID: 28090504 Free PMC article.
References
-
- Nakagoe T, Ishikawa H, Sawai T, Tsuji T, Takeshita H, Nanashima A, et al. Oncological outcome of ultra-low anterior resection with total mesorectal excision for carcinoma of the lower third of the rectum: comparison of intrapelvic double-stapled anastomosis and transanal coloanal anastomosis. Hepatogastroenterology. 2005;52:1692–1697. - PubMed
-
- Everett WG, Friend PJ, Forty J. Comparison of stapling and handsuture for left-sided large bowel anastomosis. Br J Surg. 1986;73:345–348. - PubMed
-
- Waxman BP. Large bowel anastomoses. II. The circular staplers. Br J Surg. 1983;70:64–67. - PubMed
-
- den Dulk M, Smit M, Peeters KC, Kranenbarg EM, Rutten HJ, Wiggers T, et al. A multivariate analysis of limiting factors for stoma reversal in patients with rectal cancer entered into the total mesorectal excision (TME) trial: a retrospective study. Lancet Oncol. 2007;8:297–303. - PubMed
-
- Jung SH, Yu CS, Choi PW, Kim DD, Park IJ, Kim HC, et al. Risk factors and oncologic impact of anastomotic leakage after rectal cancer surgery. Dis Colon Rectum. 2008;51:902–908. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources