Dropped gallstones: spectrum of imaging findings, complications and diagnostic pitfalls
- PMID: 23747395
- PMCID: PMC3745054
- DOI: 10.1259/bjr.20120588
Dropped gallstones: spectrum of imaging findings, complications and diagnostic pitfalls
Abstract
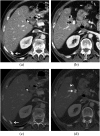
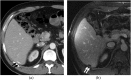
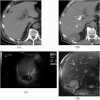
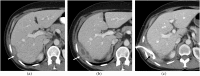
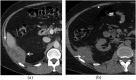
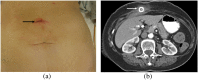
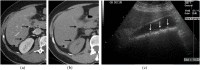
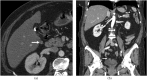
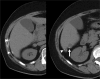
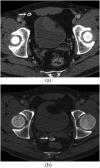
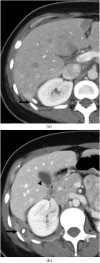
Spillage of gallstones into the abdominal cavity, referred to as "dropped gallstones" (DGs), occurs commonly during laparoscopic cholecystectomy. The majority of these spilled stones remain clinically silent; however, if uncomplicated DGs are not correctly identified on subsequent imaging, they may mimic peritoneal implants and cause unduly concern. A small percentage of DGs cause complications, including abscess and fistula formation. Recognising the DG within the abscess is critical for definitive treatment. This pictorial review illustrates the imaging appearances and complications of DGs on CT, MRI and ultrasound and emphasises pitfalls in diagnosis.
Figures

References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

