Waist circumference as measure of abdominal fat compartments
- PMID: 23762536
- PMCID: PMC3665262
- DOI: 10.1155/2013/454285
Waist circumference as measure of abdominal fat compartments
Abstract
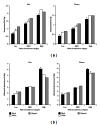
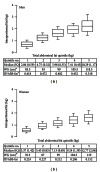
This study examines intercorrelations among waist circumference (WC), intraperitoneal fat (IPF), and subcutaneous abdominal fat (SAF) in ethnically diverse Dallas Heart Study consisting of 1538 women and 1212 men (50% Black). Correlations between fat depots and triglyceride or HOMA2-IR, biomarkers of metabolic syndrome, are also reported. Total abdominal fat (TAF), ASF, and IPF masses were measured by magnetic resonance imaging. The highest correlations with WC according to ethnicity and gender were noted for TAF (R (2) = 0.81 - 0.88) with progressively lower correlations with ASF (0.65-0.82) and IPF (0.29-0.85). The percentage of IPF relative to TAF was not significantly correlated with WC. For all WC categories, higher IPF/ASF ratios were associated with higher triglyceride levels. In contrast, differences in ratios had little or no association with HOMA2-IR. However, when all data were pooled, IPF was positively correlated with both triglyceride (r = 0.358 (men) and 0.363 (women)) and HOMA2-IR (r = 0.480 (men) and 0.517 (women)); after adjustment for ASF, IPF was still correlated with triglyceride (r = 0.353 (men) and 0.348 (women)) and HOMA2-IR (r = 0.290 (men) and 0.221 (women)). WC measures TAF reliably, but its association with IPF depends on IPF/ASF ratios that vary by gender and ethnicity.
Figures




References
-
- Alberti KGMM, Eckel RH, Grundy SM, et al. Harmonizing the metabolic syndrome: a joint interim statement of the international diabetes federation task force on epidemiology and prevention; National heart, lung, and blood institute; American heart association; World heart federation; International atherosclerosis society; And international association for the study of obesity. Circulation. 2009;120(16):1640–1645. - PubMed
-
- Carr DB, Utzschneider KM, Hull RL, et al. Intra-abdominal fat is a major determinant of the National Cholesterol Education Program Adult Treatment Panel III criteria for the metabolic syndrome. Diabetes. 2004;53(8):2087–2094. - PubMed
-
- von Eyben FE, Mouritsen E, Holm J, et al. Intra-abdominal obesity and metabolic risk factors: a study of young adults. International Journal of Obesity. 2003;27(8):941–949. - PubMed
-
- Smith JD, Borel A-L, Nazare J-A, et al. Visceral adipose tissue indicates the severity of cardiometabolic risk in Patients with and without type 2 diabetes: results from the INSPIRE me IAA Study. Journal of Clinical Endocrinology and Metabolism. 2012;97(5):1517–1525. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

