Use of advanced treatment technologies among men at low risk of dying from prostate cancer
- PMID: 23800935
- PMCID: PMC3857348
- DOI: 10.1001/jama.2013.6882
Use of advanced treatment technologies among men at low risk of dying from prostate cancer
Abstract
Importance: The use of advanced treatment technologies (ie, intensity-modulated radiotherapy [IMRT] and robotic prostatectomy) for prostate cancer is increasing. The extent to which these advanced treatment technologies have disseminated among patients at low risk of dying from prostate cancer is uncertain.
Objective: To assess the use of advanced treatment technologies, compared with prior standards (ie, traditional external beam radiation treatment [EBRT] and open radical prostatectomy) and observation, among men with a low risk of dying from prostate cancer.
Design, setting, and patients: Using Surveillance, Epidemiology, and End Results (SEER)-Medicare data, we identified a retrospective cohort of men diagnosed with prostate cancer between 2004 and 2009 who underwent IMRT (n = 23,633), EBRT (n = 3926), robotic prostatectomy (n = 5881), open radical prostatectomy (n = 6123), or observation (n = 16,384). Follow-up data were available through December 31, 2010.
Main outcomes and measures: The use of advanced treatment technologies among men unlikely to die from prostate cancer, as assessed by low-risk disease (clinical stage ≤T2a, biopsy Gleason score ≤6, and prostate-specific antigen level ≤10 ng/mL), high risk of noncancer mortality (based on the predicted probability of death within 10 years in the absence of a cancer diagnosis), or both.
Results: In our cohort, the use of advanced treatment technologies increased from 32% (95% CI, 30%-33%) to 44% (95% CI, 43%-46%) among men with low-risk disease (P < .001) and from 36% (95% CI, 35%-38%) to 57% (95% CI, 55%-59%) among men with high risk of noncancer mortality (P < .001). The use of these advanced treatment technologies among men with both low-risk disease and high risk of noncancer mortality increased from 25% (95% CI, 23%-28%) to 34% (95% CI, 31%-37%) (P < .001). Among all patients diagnosed in SEER, the use of advanced treatment technologies for men unlikely to die from prostate cancer increased from 13% (95% CI, 12%-14%), or 129.2 per 1000 patients diagnosed with prostate cancer, to 24% (95% CI, 24%-25%), or 244.2 per 1000 patients diagnosed with prostate cancer (P < .001).
Conclusion and relevance: Among men diagnosed with prostate cancer between 2004 and 2009 who had low-risk disease, high risk of noncancer mortality, or both, the use of advanced treatment technologies has increased.
Conflict of interest statement
Figures

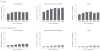
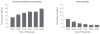
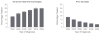
Comment in
-
Re: Effect of age, tumor risk, and comorbidity on competing risks for survival in a u.s. Population-based cohort of men with prostate cancer.J Urol. 2013 Nov;190(5):1766-7. doi: 10.1016/j.juro.2013.07.079. Epub 2013 Aug 2. J Urol. 2013. PMID: 24120782 No abstract available.
-
Use of advanced treatment technologies among men at low risk of dying from prostate cancer.BJU Int. 2014 Aug;114(2):166-7. doi: 10.1111/bju.12547. Epub 2014 Mar 14. BJU Int. 2014. PMID: 24180347 No abstract available.
-
Re: use of advanced treatment technologies among men at low risk of dying from prostate cancer.Eur Urol. 2014 Jan;65(1):250. doi: 10.1016/j.eururo.2013.10.024. Eur Urol. 2014. PMID: 24289855 No abstract available.
Similar articles
-
Association Between Radiation Therapy, Surgery, or Observation for Localized Prostate Cancer and Patient-Reported Outcomes After 3 Years.JAMA. 2017 Mar 21;317(11):1126-1140. doi: 10.1001/jama.2017.1704. JAMA. 2017. PMID: 28324093 Free PMC article.
-
Patient-Reported Outcomes Through 5 Years for Active Surveillance, Surgery, Brachytherapy, or External Beam Radiation With or Without Androgen Deprivation Therapy for Localized Prostate Cancer.JAMA. 2020 Jan 14;323(2):149-163. doi: 10.1001/jama.2019.20675. JAMA. 2020. PMID: 31935027 Free PMC article.
-
Morbidity and Mortality of Locally Advanced Prostate Cancer: A Population Based Analysis Comparing Radical Prostatectomy versus External Beam Radiation.J Urol. 2017 Nov;198(5):1061-1068. doi: 10.1016/j.juro.2017.05.073. Epub 2017 May 26. J Urol. 2017. PMID: 28552709
-
The impact of technology diffusion on treatment for prostate cancer.Med Care. 2013 Dec;51(12):1076-84. doi: 10.1097/MLR.0000000000000019. Med Care. 2013. PMID: 24226306 Free PMC article.
-
Management of localised prostate cancer: watchful waiting, surgery or radiation therapy, depending on the natural course, which is often relatively slow.Prescrire Int. 2012 Oct;21(131):242-8. Prescrire Int. 2012. PMID: 23185849 Review.
Cited by
-
High tech or high risk? An analysis of media reports about robotic surgery.J Robot Surg. 2017 Jun;11(2):211-216. doi: 10.1007/s11701-016-0647-z. Epub 2016 Oct 24. J Robot Surg. 2017. PMID: 27778227
-
Episode Payments for Transcatheter and Surgical Aortic Valve Replacement.Circ Cardiovasc Qual Outcomes. 2019 Dec;12(12):e005781. doi: 10.1161/CIRCOUTCOMES.119.005781. Epub 2019 Dec 13. Circ Cardiovasc Qual Outcomes. 2019. PMID: 31830824 Free PMC article.
-
Penile rehabilitation after radical prostatectomy: does it work?Transl Androl Urol. 2015 Apr;4(2):110-23. doi: 10.3978/j.issn.2223-4683.2015.02.01. Transl Androl Urol. 2015. PMID: 26816818 Free PMC article. Review.
-
Association Between Urologist Merit-Based Incentive Payment System Performance and Quality of Prostate Cancer Care.Urol Pract. 2024 Jan;11(1):207-214. doi: 10.1097/UPJ.0000000000000463. Epub 2023 Sep 25. Urol Pract. 2024. PMID: 37748132 Free PMC article.
-
Seventh Joint Meeting of K-J-CaP and CaPSURE: extending the global initiative to improve prostate cancer management.Prostate Int. 2014;2(2):50-69. doi: 10.12954/PI.14047. Epub 2014 Jun 30. Prostate Int. 2014. PMID: 26153555 Free PMC article.
References
-
- Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, 2010. CA Cancer J Clin. 2010;60(5):277–300. - PubMed
-
- Roehrig C, Miller G, Lake C, Bryant J. National health spending by medical condition, 1996–2005. Health Aff (Millwood) 2009;28(2):w358–w367. - PubMed
-
- Hu JC, Gu X, Lipsitz SR, et al. Comparative effectiveness of minimally invasive vs open radical prostatectomy. JAMA. 2009;302(14):1557–1564. - PubMed
-
- Barbash GI, Glied SA. New technology and health care costs: the case of robot-assisted surgery. N Engl J Med. 2010;363(8):701–704. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases

