Variation in reported experience of involvement in cancer treatment decision making: evidence from the National Cancer Patient Experience Survey
- PMID: 23807170
- PMCID: PMC3738115
- DOI: 10.1038/bjc.2013.316
Variation in reported experience of involvement in cancer treatment decision making: evidence from the National Cancer Patient Experience Survey
Abstract
Background: Exploring variation in patients' experiences of involvement in treatment decision making can identify groups needing extra support, such as additional consultation time, when considering treatment options.
Methods: We analysed data from the 2010 English National Cancer Patient Experience Survey, a national survey of all patients attending hospitals in England for cancer treatment over a 3-month period, to examine how experience of involvement in decisions about treatment varied between patients with 38 different primary cancers using logistic regression. We analysed responses from 41 411 patients to a single question examining patient experience of involvement in treatment decision making. We calculated unadjusted odds ratios of reporting the most positive experience between patients of different sociodemographic and tumour characteristics and explored the effects of adjusting for age, gender, ethnicity, deprivation, cancer type and hospital of treatment.
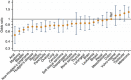
Results: Of the 41 441 respondents, 29 776 (72%) reported positive experiences of decision-making involvement. Younger patients reported substantially less positive experiences of involvement in decision making (adjusted OR=0.49 16-24 vs 65-74; P<0.001), as did ethnic minorities (adjusted ORs=0.52, 0.62 and 0.73 for Black, Chinese and Asian vs White patients, respectively; P<0.001). Experience varied considerably between patients with different cancers ( e.g., OR=0.52 for anal and 1.37 for melanoma vs colon cancer; P<0.001), with ovarian, myeloma, bladder and rectal cancer patients reporting substantially worse experiences compared with other patients with gynaecological, haematological, urological and colorectal cancers, respectively. Clustering of different patient groups within hospitals with outlying performance report scores could not account for observed differences.
Conclusion: Efforts to improve involvement in treatment decision making can focus on those who report the worst experience, in particular younger patients, ethnic minorities and patients with rectal, ovarian, multiple myeloma and bladder cancer.
Figures
References
-
- Ayanian JZ, Zaslavsky AM, Arora NK, Kahn KL, Malin JL, Ganz Pa, Ryn M, van, Hornbrook MC, Kiefe CI, He Y, Urmie JM, Weeks JC, Harrington DP. Patients' experiences with care for lung cancer and colorectal cancer: findings from the Cancer Care Outcomes Research and Surveillance Consortium. J Clin Oncol. 2010;28:4154–4161. - PMC - PubMed
-
- Barry MJ, Edgman-Levitan S. Shared decision making--pinnacle of patient-centered care. N Engl J Med. 2012;366:780–781. - PubMed
-
- Benbassat J, Pilpel D, Tidhar M. Patients' preferences for participation in clinical decision making: a review of published surveys. Behav Med. 1998;24:81–88. - PubMed
-
- Brown R, Butow P, Wilson-Genderson M, Bernhard J, Ribi K, Juraskova I. Meeting the decision-making preferences of patients with breast cancer in oncology consultations: impact on decision-related outcomes. J Clin Oncol. 2012;30:857–862. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

