Quality of life following laparoscopic Nissen fundoplication: assessing short-term and long-term outcomes
- PMID: 23840119
- PMCID: PMC3699043
- DOI: 10.3748/wjg.v19.i24.3810
Quality of life following laparoscopic Nissen fundoplication: assessing short-term and long-term outcomes
Abstract
Aim: To investigate the quality of life following laparoscopic Nissen fundoplication by assessing short-term and long-term outcomes.
Methods: From 1992 to 2005, 249 patients underwent laparoscopic Nissen fundoplication. Short-term outcome data including symptom response, side effects of surgery, endoscopy, and patient's perception of overall success were collected prospectively. Long-term outcomes were investigated retrospectively in patients with a median follow-up of 10 years by assessment of reflux symptoms, side effects of surgery, durability of antireflux surgery, need for additional treatment, patient's perception of success, and quality of life. Antireflux surgery was considered a failure based on the following criteria: moderate to severe heartburn or regurgitation; moderate to severe dysphagia reported in combination with heartburn or regurgitation; regular proton pump inhibitor medication use; endoscopic evidence of erosive esophagitis Savary-Miller grade 1-4; pathological 24-h pH monitoring; or necessity to undergo an additional surgery. The main outcome measures were short- and long-term cure rates and quality of life, with patient satisfaction as a secondary outcome measure.
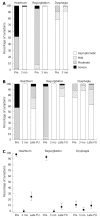
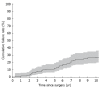
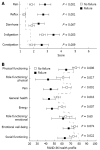
Results: Conversion from laparoscopy to open surgery was necessary in 2.4% of patients. Mortality was zero and the 30-d morbidity was 7.6% (95%CI: 4.7%-11.7%). The median postoperative hospital stay was 2 d [interquartile range (IQR) 2-3 d]. Two hundred and forty-seven patients were interviewed for short-term analysis following endoscopy. Gastroesophageal reflux disease was cured in 98.4% (95%CI: 95.9%-99.6%) of patients three months after surgery. New-onset dysphagia was encountered postoperatively in 13 patients (6.7%); 95% reported that the outcome was better after antireflux surgery than with preoperative medical treatment. One hundred and thirty-nine patients with a median follow-up of 10.2 years (IQR 7.2-11.6 years) were available for a long-term evaluation. Cumulative long-term cure rates were 87.7% (81.0%-92.2%) at 5 years and 72.9% (64.0%-79.9%) at 10 years. Gastrointestinal symptom rating scores and RAND-36 quality of life scores of patients with treatment success were similar to those of the general population but significantly lower in those with failed antireflux surgery. Of the patients available for long-term follow-up, 83% rated their operation a success.
Conclusion: For the long-term, our results indicate decreasing effectiveness of laparoscopic antireflux surgery, although most of the patients seem to have an overall quality of life similar to that of the general population.
Keywords: Antireflux; Gastrointestinal symptom rating scores; Laparoscopy; Long-term outcome; Nissen fundoplication; RAND-36.
Figures
References
-
- Dent J. Controversies in long-term management of reflux disease. Baillieres Best Pract Res Clin Gastroenterol. 2000;14:811–826. - PubMed
-
- Dellon ES, Shaheen NJ. Persistent reflux symptoms in the proton pump inhibitor era: the changing face of gastroesophageal reflux disease. Gastroenterology. 2010;139:7–13.e3. - PubMed
-
- Nealis TB, Howden CW. Is there a dark side to long-term proton pump inhibitor therapy? Am J Ther. 2008;15:536–542. - PubMed
-
- Wileman SM, McCann S, Grant AM, Krukowski ZH, Bruce J. Medical versus surgical management for gastro-oesophageal reflux disease (GORD) in adults. Cochrane Database Syst Rev. 2010;(3):CD003243. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

