Molecular mechanisms of thoracic aortic dissection
- PMID: 23856125
- PMCID: PMC3788606
- DOI: 10.1016/j.jss.2013.06.007
Molecular mechanisms of thoracic aortic dissection
Abstract
Thoracic aortic dissection (TAD) is a highly lethal vascular disease. In many patients with TAD, the aorta progressively dilates and ultimately ruptures. Dissection formation, progression, and rupture cannot be reliably prevented pharmacologically because the molecular mechanisms of aortic wall degeneration are poorly understood. The key histopathologic feature of TAD is medial degeneration, a process characterized by smooth muscle cell depletion and extracellular matrix degradation. These structural changes have a profound impact on the functional properties of the aortic wall and can result from excessive protease-mediated destruction of the extracellular matrix, altered signaling pathways, and altered gene expression. Review of the literature reveals differences in the processes that lead to ascending versus descending and sporadic versus hereditary TAD. These differences add to the complexity of this disease. Although tremendous progress has been made in diagnosing and treating TAD, a better understanding of the molecular, cellular, and genetic mechanisms that cause this disease is necessary to developing more effective preventative and therapeutic treatment strategies.
Keywords: Aneurysm; Aortic dissection; Degeneration; Media.
Copyright © 2013 Elsevier Inc. All rights reserved.
Figures

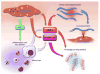

References
-
- Golledge J, Eagle KA. Acute aortic dissection. Lancet. 2008;372:55. - PubMed
-
- Clouse WD, Hallett JW, Jr, Schaff HV, et al. Acute aortic dissection: population-based incidence compared with degenerative aortic aneurysm rupture. Mayo Clin Proc. 2004;79:176. - PubMed
-
- Meszaros I, Morocz J, Szlavi J, et al. Epidemiology and clinicopathology of aortic dissection. Chest. 2000;117:1271. - PubMed
-
- Kochanek KD, Xu JQ, Murphy SL, et al. Deaths: Final data for 2009. Natl Vital Stat Rep. 2011:60. - PubMed
-
- Borst HG, Heinemann MK, Stone CD. Histology and ultrastructure. In: Borst HG, Heinemann MK, Stone CD, editors. Surgical Treatment of Aortic Dissection. New York, NY: Churchill Livingstone; 1996. pp. 37–46.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

