Body mass index and its association with clinical outcomes for advanced non-small-cell lung cancer patients enrolled on Eastern Cooperative Oncology Group clinical trials
- PMID: 23887169
- PMCID: PMC3763835
- DOI: 10.1097/JTO.0b013e31829cf942
Body mass index and its association with clinical outcomes for advanced non-small-cell lung cancer patients enrolled on Eastern Cooperative Oncology Group clinical trials
Abstract
Introduction: Obesity increases the risk of death from many adverse health outcomes and has also been linked with cancer outcomes. The impact of obesity on outcomes of advanced non-small-cell lung cancer patients is unclear.
Methods: The authors evaluated the association of body mass index (BMI) and outcomes in 2585 eligible patients enrolled in three consecutive first-line trials conducted by the Eastern Cooperative Oncology Group. BMI was categorized as underweight (BMI < 18.5 kg/m), normal weight (BMI: 18.5 to < 25 kg/m), overweight (BMI: 25 to < 30 kg/m), and obese (BMI ≥ 30 kg/m). In addition to analyzing overall and progression-free survival, reasons for treatment discontinuation were also assessed by BMI group.
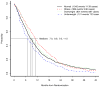
Results: Of the patients enrolled, 4.6% were underweight, 44.1% were normal weight, 34.3% of patients were classified as overweight, and 16.9% were obese. Nonproportional hazards existed for obese patients relative to the other three groups of patients, with a change in overall survival hazard occurring at approximately 16 months. In multivariable Cox models, obese patients had superior outcomes earlier on study compared with normal/overweight patients 0.86 (HR=0.86, p=0.04; 95% CI: 0.75-0.99), but later experienced increased hazard (HR=1.54, p< 0.001; 95% CI: 1.22-1.94), indicating a time effect while undergoing treatment.
Conclusion: Data from these three trials suggest differential outcomes associated with BMI, and additional studies of the mechanisms underlying this observation, as well as dietary and lifestyle interventions, are warranted to help optimize therapy.
Figures
References
-
- Flegal KM, Carroll MD, Kit BK, et al. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA. 2012;307:491–497. - PubMed
-
- Mokdad AH, Ford ES, Bowman BA, et al. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA. 2003;289:76–79. - PubMed
-
- Halabi SH, Ou S-S, Vogelzang, et al. Inverse correlation between body mass index and clinical outcomes in men with advanced castration-recurrent prostate cancer. Cancer. 2007;110:1478–1484. - PubMed
-
- Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer. 2004;4:579–591. - PubMed
-
- Renehan AG, Soerjomataram I, Leitzmann MF. Interpreting the epidemiological evidence linking obesity and cancer: a framework for population-attributable risk estimations in Europe. Eur J Cancer. 2010;46:2581–2592. - PubMed
Publication types
MeSH terms
Grants and funding
- CA21076/CA/NCI NIH HHS/United States
- CA66636/CA/NCI NIH HHS/United States
- U10 CA021115/CA/NCI NIH HHS/United States
- U10 CA049883/CA/NCI NIH HHS/United States
- P30 CA082709/CA/NCI NIH HHS/United States
- U10 CA021076/CA/NCI NIH HHS/United States
- U10 CA066636/CA/NCI NIH HHS/United States
- CA49957/CA/NCI NIH HHS/United States
- U10 CA016116/CA/NCI NIH HHS/United States
- U10 CA023318/CA/NCI NIH HHS/United States
- U10 CA049957/CA/NCI NIH HHS/United States
- CA16116/CA/NCI NIH HHS/United States
- CA23318/CA/NCI NIH HHS/United States
- CA49883/CA/NCI NIH HHS/United States
- CA21115/CA/NCI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical