Brachial arterial temperature as an indicator of core temperature: proof of concept and potential applications
- PMID: 23930377
- PMCID: PMC4557585
Brachial arterial temperature as an indicator of core temperature: proof of concept and potential applications
Abstract
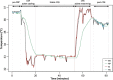
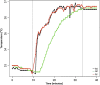
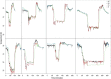
There is potential for heat loss and hypothermia during anesthesia and also for hyperthermia if heat conservation and active warming measures are not accurately titrated. Accurate temperature monitoring is particularly important in procedures in which the patient is actively cooled and then rewarmed such as during cardiopulmonary bypass surgery (CPB). We simultaneously measured core, nasopharyngeal, and brachial artery temperatures to investigate the last named as a potential peripheral temperature monitoring site. Ten patients undergoing hypothermic CPB were instrumented for simultaneous monitoring of temperatures in the pulmonary artery (PA), aortic arterial inflow (AI), nasopharynx (NP), and brachial artery (BA). Core temperature was defined as PA temperature before and after CPB and the AI temperature during CPB. Mean deviations of BA and NP temperatures from core temperature were calculated for three steady-state periods (before, during, and after CPB). Mean deviation of BA and NP temperatures from AI temperature was also calculated during active rewarming. A total of 1862 measurements were obtained and logged from eight patients. Mean BA and NP deviations from core temperature across the steady-state periods (before, during, and after CBP) were, respectively: .23 +/- .25, -.26 +/- .3, and -.09 +/- .05 degrees C (BA), and .11 +/- .19, -.1 +/- .47, and -.04 +/- .3 degrees C (NP). During steady-state periods, there was no evidence of a difference between the mean BA and NP deviation. During active rewarming, the mean difference between the BA and AI temperatures was .14 +/- .36 degrees C. During this period, NP temperature lagged behind AI and BA temperatures by up to 41 minutes and was up to 5.3 degres C lower than BA (mean difference between BA and NP temperatures was 1.22 +/- .58 degrees C). The BA temperature is an adequate surrogate for core temperature. It also accurately tracks the changing AI temperature during rewarming and is therefore potentially useful in detecting a hyperthermic perfusate, which might cause cerebral hyperthermia.
Conflict of interest statement
The senior author has stated that the authors have reported no material, financial, or other relationship with any healthcare-related business or other entity whose products or services are discussed in this paper.
Figures

Similar articles
-
Temperature monitoring during cardiopulmonary bypass--do we undercool or overheat the brain?Eur J Cardiothorac Surg. 2004 Sep;26(3):580-5. doi: 10.1016/j.ejcts.2004.05.004. Eur J Cardiothorac Surg. 2004. PMID: 15302054
-
Should we rely on nasopharyngeal temperature during cardiopulmonary bypass?Perfusion. 2002 Mar;17(2):145-51. doi: 10.1191/0267659102pf536oa. Perfusion. 2002. PMID: 11958306 Clinical Trial.
-
Afterdrop after hypothermic cardiopulmonary bypass: the value of tympanic membrane temperature monitoring.J Cardiothorac Vasc Anesth. 1996 Apr;10(3):336-41. doi: 10.1016/s1053-0770(96)80093-0. J Cardiothorac Vasc Anesth. 1996. PMID: 8725413
-
The Society of Thoracic Surgeons, The Society of Cardiovascular Anesthesiologists, and The American Society of ExtraCorporeal Technology: Clinical Practice Guidelines for Cardiopulmonary Bypass--Temperature Management During Cardiopulmonary Bypass.J Cardiothorac Vasc Anesth. 2015 Aug;29(4):1104-13. doi: 10.1053/j.jvca.2015.07.011. J Cardiothorac Vasc Anesth. 2015. PMID: 26279227 Review.
-
The management of temperature during cardiopulmonary bypass: effect on neuropsychological outcome.J Card Surg. 1995 Jul;10(4 Suppl):481-7. doi: 10.1111/j.1540-8191.1995.tb00681.x. J Card Surg. 1995. PMID: 7579846 Review.
Cited by
-
Zero-heat-flux core temperature monitoring system: an observational secondary analysis to evaluate agreement with naso-/oropharyngeal probe during anesthesia.J Clin Monit Comput. 2020 Oct;34(5):1121-1129. doi: 10.1007/s10877-019-00411-y. Epub 2019 Nov 6. J Clin Monit Comput. 2020. PMID: 31696391
References
-
- Grigore AM, Murray CF, Ramakrishna H, Djaiani G.. A core review of temperature regimens and neuroprotection during cardiopulmonary bypass: Does rewarming rate matter? Anesth Analg. 2009;109:1741–1751. - PubMed
-
- Cook DJ.. CON: Temperature regimens and neuroprotection during cardiopulmonary bypass: Does rewarming rate matter? Anesth Analg. 2009;109:1733–1737. - PubMed
-
- Akata T, Setoguchi H, Shirozu K, Yoshino J.. Reliability of temperatures measured at standard monitoring sites as an index of brain temperature during deep hypothermic cardiopulmonary bypass conducted for thoracic aortic reconstruction. J Thorac Cardiovasc Surg. 2007;133:1559–1565. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous
