Modifications of skeletal muscle ryanodine receptor type 1 and exercise intolerance in heart failure
- PMID: 23953820
- PMCID: PMC4399850
- DOI: 10.1016/j.healun.2013.06.026
Modifications of skeletal muscle ryanodine receptor type 1 and exercise intolerance in heart failure
Abstract
Background: In experimental heart failure animal models, remodeling of skeletal and cardiac muscle ryanodine receptors (RyR), including phosphorylation, S-nitrosylation and oxidation, have been reported to contribute to pathologic Ca2+ release, impaired muscle function and fatigue. However, it is not known whether similar remodeling of RyR1 in skeletal muscle occurs in patients with heart failure, and if this is associated with impairment of physical activity.
Methods: We studied 8 sedentary patients with New York Heart Association (NYHA) Class III heart failure and 7 age-matched, healthy, but sedentary controls. All heart failure patients had NYHA Class III and peak VO2, echocardiography and NT-proBNP data consistent with moderate to severe heart failure. The age-matched controls included were allowed hypertension but sub-clinical heart failure was to have been ruled out by normal peak VO2, echocardiography and NT-proBNP.
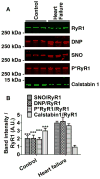
Results: Exercise capacity (VO2max) differed by almost 2-fold between heart failure patients and age-matched controls. Compared with controls, skeletal muscle RyR1 in heart failure patients was excessively phosphorylated, S-nitrosylated and oxidized. Furthermore, RyR1 from heart failure patients was depleted of its stabilizing protein FK 506-binding protein 12 (FKBP12, or calstabin1).
Conclusions: For the first time we show that skeletal muscle RyR1 from human heart failure is post-translationally modified, which corroborates previous data from experimental animal studies. This indicates pathologic Ca2+ release as a potential mechanism behind skeletal muscle weakness and impaired exercise tolerance in patients with heart failure and suggests a potential target for pharmacologic intervention.
Keywords: ageing; muscle fatigue activity; physical exercise capacity calcium oxidative stress; post-translational contraction; protein processing.
Copyright © 2013 International Society for Heart and Lung Transplantation. Published by Elsevier Inc. All rights reserved.
Figures
References
-
- Jessup M, Brozena S. Heart failure. N Engl J Med. 2003;348:2007–18. - PubMed
-
- Mancini DM, Eisen H, Kussmaul W, Mull R, Edmunds LH, Jr, Wilson JR. Value of peak exercise oxygen consumption for optimal timing of cardiac transplantation in ambulatory patients with heart failure. Circulation. 1991;83:778–86. - PubMed
-
- Piepoli MF, Guazzi M, Boriani G, et al. Exercise intolerance in chronic heart failure: mechanisms and therapies. Part I. European journal of cardiovascular prevention and rehabilitation : official journal of the European Society of Cardiology, Working Groups on Epidemiology & Prevention and Cardiac Rehabilitation and Exercise Physiology. 2010;17:637–42. - PubMed
-
- Wilson JR, Martin JL, Ferraro N. Impaired skeletal muscle nutritive flow during exercise in patients with congestive heart failure: role of cardiac pump dysfunction as determined by the effect of dobutamine. Am J Cardiol. 1984;53:1308–15. - PubMed
-
- Wilson JR, Martin JL, Ferraro N, Weber KT. Effect of hydralazine on perfusion and metabolism in the leg during upright bicycle exercise in patients with heart failure. Circulation. 1983;68:425–32. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

