The hemodynamic response to dexmedetomidine loading dose in children with and without pulmonary hypertension
- PMID: 23960035
- PMCID: PMC3830564
- DOI: 10.1213/ANE.0b013e3182a15aa6
The hemodynamic response to dexmedetomidine loading dose in children with and without pulmonary hypertension
Abstract
Background: Dexmedetomidine, an α-2 receptor agonist, is widely used in children with cardiac disease. Significant hemodynamic responses, including systemic and pulmonary vasoconstriction, have been reported after dexmedetomidine administration. Our primary goal of this prospective, observational study was to quantify the effects of dexmedetomidine initial loading doses on mean pulmonary artery pressure (PAP) in children with and without pulmonary hypertension.
Methods: Subjects were children undergoing cardiac catheterization for either routine surveillance after cardiac transplantation (n = 21) or pulmonary hypertension studies (n = 21). After anesthetic induction with sevoflurane and tracheal intubation, sevoflurane was discontinued and anesthesia was maintained with midazolam 0.1 mg/kg i.v. (or 0.5 mg/kg orally preoperatively) and remifentanil i.v. infusion 0.5 to 0.8 μg/kg/min. Ventilation was mechanically controlled to maintain PCO2 35 to 40 mm Hg. When end-tidal sevoflurane was 0% and fraction of inspired oxygen (FIO2) was 0.21, baseline heart rate, mean arterial blood pressure, PAP, right atrial pressure, pulmonary artery occlusion pressure, right ventricular end-diastolic pressure, cardiac output, and arterial blood gases were measured, and indexed systemic vascular resistance, indexed pulmonary vascular resistance, and cardiac index were calculated. Each subject then received a 10-minute infusion of dexmedetomidine of 1 μg/kg, 0.75 μg/kg, or 0.5 μg/kg. Measurements and calculations were repeated at the conclusion of the infusion.
Results: Most hemodynamic responses were similar in children with and without pulmonary hypertension. Heart rate decreased significantly, and mean arterial blood pressure and indexed systemic vascular resistance increased significantly. Cardiac index did not change. A small, statistically significant increase in PAP was observed in transplant patients but not in subjects with pulmonary hypertension. Changes in indexed pulmonary vascular resistance were not significant.
Conclusion: Dexmedetomidine initial loading doses were associated with significant systemic vasoconstriction and hypertension, but a similar response was not observed in the pulmonary vasculature, even in children with pulmonary hypertension. Dexmedetomidine does not appear to be contraindicated in children with pulmonary hypertension.
Figures
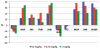
Comment in
-
A word of caution: dexmedetomidine and pulmonary hypertension.Anesth Analg. 2014 Jul;119(1):216-217. doi: 10.1213/ANE.0000000000000236. Anesth Analg. 2014. PMID: 24945133 No abstract available.
-
In response.Anesth Analg. 2014 Jul;119(1):217-218. doi: 10.1213/ANE.0000000000000237. Anesth Analg. 2014. PMID: 24945134 No abstract available.
References
-
- Munro HM, Tirotta CF, Felix DE, Lagueruela RG, Madril DR, Zahn EM, Nykanen DG. Initial experience with dexmedetomidine for diagnostic and interventional cardiac catheterization in children. Paediatr Anaesth. 2007;17:109–12. - PubMed
-
- Barton KP, Munoz R, Morell VO, Chrysostomou C. Dexmedetomidine as the primary sedative during invasive procedures in infants and toddlers with congenital heart disease. Pediatr Crit Care Med. 2008;9:612–5. - PubMed
-
- Chrysostomou C, Sanchez De Toledo J, Avolio T, Motoa MV, Berry D, Morell VO, Orr R, Munoz R. Dexmedetomidine use in a pediatric cardiac intensive care unit: can we use it in infants after cardiac surgery? Pediatr Crit Care Med. 2009;10:654–60. - PubMed
-
- Hosokawa K, Shime N, Kato Y, Taniguchi A, Maeda Y, Miyazaki T, Hashimoto S. Dexmedetomidine sedation in children after cardiac surgery. Pediatr Crit Care Med. 2010;11:39–43. - PubMed
-
- Chrysostomou C, Komarlu R, Lichtenstein S, Shiderly D, Arora G, Orr R, Wearden PD, Morell VO, Munoz R, Jooste EH. Electrocardiographic effects of dexmedetomidine in patients with congenital heart disease. Intensive Care Med. 2010;36:836–42. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

