Does the direct anterior approach in THA offer faster rehabilitation and comparable safety to the posterior approach?
- PMID: 23963704
- PMCID: PMC3890195
- DOI: 10.1007/s11999-013-3231-0
Does the direct anterior approach in THA offer faster rehabilitation and comparable safety to the posterior approach?
Abstract
Background: Newer surgical approaches to THA, such as the direct anterior approach, may influence a patient's time to recovery, but it is important to make sure that these approaches do not compromise reconstructive safety or accuracy.
Questions/purposes: We compared the direct anterior approach and conventional posterior approach in terms of (1) recovery of hip function after primary THA, (2) general health outcomes, (3) operative time and surgical complications, and (4) accuracy of component placement.
Methods: In this prospective, comparative, nonrandomized study of 120 patients (60 direct anterior THA, 60 posterior THAs), we assessed functional recovery using the VAS pain score, timed up and go (TUG) test, motor component of the Functional Independence Measure™ (M-FIM™), UCLA activity score, Harris hip score, and patient-maintained subjective milestone diary and general health outcome using SF-12 scores. Operative time, complications, and component placement were also compared.
Results: Functional recovery was faster in patients with the direct anterior approach on the basis of TUG and M-FIM™ up to 2 weeks; no differences were found in terms of the other metrics we used, and no differences were observed between groups beyond 6 weeks. General health outcomes, operative time, and complications were similar between groups. No clinically important differences were observed in terms of implant alignment.
Conclusions: We observed very modest functional advantages early in recovery after direct anterior THA compared to posterior-approach THA. Randomized trials are needed to validate these findings, and these findings may not generalize well to lower-volume practice settings or to surgeons earlier in the learning curve of direct anterior THA.
Figures

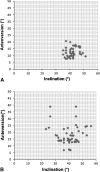
Similar articles
-
A systematic review and meta-analysis of direct anterior approach versus posterior approach in total hip arthroplasty.J Orthop Surg Res. 2018 Sep 6;13(1):229. doi: 10.1186/s13018-018-0929-4. J Orthop Surg Res. 2018. PMID: 30189881 Free PMC article.
-
Does Surgical Approach Affect Patient-reported Function After Primary THA?Clin Orthop Relat Res. 2016 Apr;474(4):971-81. doi: 10.1007/s11999-015-4639-5. Epub 2015 Nov 30. Clin Orthop Relat Res. 2016. PMID: 26620966 Free PMC article.
-
John Charnley Award: Randomized Clinical Trial of Direct Anterior and Miniposterior Approach THA: Which Provides Better Functional Recovery?Clin Orthop Relat Res. 2018 Feb;476(2):216-229. doi: 10.1007/s11999.0000000000000112. Clin Orthop Relat Res. 2018. PMID: 29529650 Free PMC article. Clinical Trial.
-
Do Postoperative Results Differ in a Randomized Trial Between a Direct Anterior and a Direct Lateral Approach in THA?Clin Orthop Relat Res. 2019 Jan;477(1):145-155. doi: 10.1097/CORR.0000000000000439. Clin Orthop Relat Res. 2019. PMID: 30179928 Free PMC article. Clinical Trial.
-
Gait analysis after total hip arthroplasty using direct anterior approach versus anterolateral approach: a systematic review and meta-analysis.BMC Musculoskelet Disord. 2019 Feb 8;20(1):63. doi: 10.1186/s12891-019-2450-2. BMC Musculoskelet Disord. 2019. PMID: 30736783 Free PMC article.
Cited by
-
Clinical efficacy of direct anterior approach vs. other surgical approaches for total hip arthroplasty: A systematic review and meta-analysis based on RCTs.Front Surg. 2022 Oct 3;9:1022937. doi: 10.3389/fsurg.2022.1022937. eCollection 2022. Front Surg. 2022. PMID: 36263087 Free PMC article. Review.
-
A systematic review and meta-analysis of direct anterior approach versus posterior approach in total hip arthroplasty.J Orthop Surg Res. 2018 Sep 6;13(1):229. doi: 10.1186/s13018-018-0929-4. J Orthop Surg Res. 2018. PMID: 30189881 Free PMC article.
-
The risk of revision after total hip arthroplasty in young patients depends on surgical approach, femoral head size and bearing type; an analysis of 19,682 operations in the Dutch arthroplasty register.BMC Musculoskelet Disord. 2019 Aug 22;20(1):385. doi: 10.1186/s12891-019-2765-z. BMC Musculoskelet Disord. 2019. PMID: 31438921 Free PMC article.
-
Influence of surgical approach on complication risk in primary total hip arthroplasty.Acta Orthop. 2018 Jun;89(3):289-294. doi: 10.1080/17453674.2018.1438694. Epub 2018 Feb 16. Acta Orthop. 2018. PMID: 29451051 Free PMC article.
-
Mid-term results of cemented hip arthroplasties through the direct anterior approach in the lateral decubitus position: a retrospective cohort study.J Orthop Surg Res. 2024 Apr 1;19(1):206. doi: 10.1186/s13018-024-04696-x. J Orthop Surg Res. 2024. PMID: 38561763 Free PMC article.
References
-
- Alecci V, Valente M, Crucil M, Minerva M, Pellegrino CM, Sabbadini DD. Comparison of primary total hip replacements performed with a direct anterior approach versus the standard lateral approach: perioperative findings. J Orthop Traumatol. 2011;12:123–129. doi: 10.1007/s10195-011-0144-0. - DOI - PMC - PubMed
-
- Amstutz HC, Thomas BJ, Jinnah R, Kim W, Grogan T, Yale C. Treatment of primary osteoarthritis of the hip: a comparison of total joint and surface replacement arthroplasty. J Bone Joint Surg Am. 1984;66:228–241. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

