Populations at risk for severe or complicated influenza illness: systematic review and meta-analysis
- PMID: 23974637
- PMCID: PMC3805492
- DOI: 10.1136/bmj.f5061
Populations at risk for severe or complicated influenza illness: systematic review and meta-analysis
Abstract
Objective: To evaluate risk factors for severe outcomes in patients with seasonal and pandemic influenza.
Design: Systematic review.
Study selection: Observational studies reporting on risk factor-outcome combinations of interest in participants with influenza. Outcomes included death, ventilator support, admission to hospital, admission to an intensive care unit, pneumonia, and composite outcomes.
Data sources: Medline, Embase, CINAHL, Global Health, and the Cochrane Central Register of Controlled Trials to March 2011.
Risk of bias assessment: Newcastle-Ottawa scale to assess the risk of bias. GRADE framework to evaluate the quality of evidence.
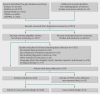
Results: 63 537 articles were identified of which 234 with a total of 610 782 participants met the inclusion criteria. The evidence supporting risk factors for severe outcomes of influenza ranged from being limited to absent. This was particularly relevant for the relative lack of data for non-2009 H1N1 pandemics and for seasonal influenza studies. Limitations in the published literature included lack of power and lack of adjustment for confounders was widespread: adjusted risk estimates were provided for only 5% of risk factor-outcome comparisons in 39 of 260 (15%) studies. The level of evidence was low for "any risk factor" (odds ratio for mortality 2.77, 95% confidence interval 1.90 to 4.05 for pandemic influenza and 2.04, 1.74 to 2.39 for seasonal influenza), obesity (2.74, 1.56 to 4.80 and 30.1, 1.74 to 2.39), cardiovascular diseases (2.92, 1.76 to 4.86 and 1.97, 1.06 to 3.67), and neuromuscular disease (2.68, 1.91 to 3.75 and 3.21, 1.84 to 5.58). The level of evidence was very low for all other risk factors. Some well accepted risk factors such as pregnancy and belonging to an ethnic minority group could not be identified as risk factors. In contrast, women who were less than four weeks post partum had a significantly increased risk of death from pandemic influenza (4.43, 1.24 to 15.81).
Conclusion: The level of evidence to support risk factors for influenza related complications is low and some well accepted risk factors, including pregnancy and ethnicity, could not be confirmed as risks. Rigorous and adequately powered studies are needed.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at
Comment in
-
For some groups traditionally considered to be 'high risk', the evidence of an increased risk of severe influenza-associated illness is poor quality.Evid Based Med. 2014 Jun;19(3):110. doi: 10.1136/eb-2013-101572. Epub 2013 Dec 19. Evid Based Med. 2014. PMID: 24357401 No abstract available.
References
-
- World Health Organization. Fact sheet on influenza. 2009. www.who.int/mediacentre/factsheets/fs211/en/index.html.
-
- Center for Disease Control and Prevention. People at high risk of developing flu-related complications. 2012. www.cdc.gov/flu/index.htm.
-
- Dawood FS, Iuliano AD, Reed C, Meltzer MI, Shay DK, Cheng PY, et al. Estimated global mortality associated with the first 12 months of 2009 pandemic influenza A H1N1 virus circulation: a modelling study. Lancet Infect Dis 2012;12:687-95. - PubMed
-
- Fiore AE, Uyeki TM, Broder K, Finelli L, Euler GL, Singleton JA, et al. Prevention and control of influenza with vaccines: recommendations of the Advisory Committee on Immunization Practices (ACIP), 2010. MMWR Recomm Rep 2010;59(RR-8):1-62. - PubMed
-
- World Health Organization. Strategic Advisory Group of Experts (SAGE) meeting of April 2012. www.who.int/influenza/vaccines/SAGE_information/en/index.html.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous