Integrating the myocardial matrix into heart failure recognition and management
- PMID: 23989715
- PMCID: PMC3869184
- DOI: 10.1161/CIRCRESAHA.113.300309
Integrating the myocardial matrix into heart failure recognition and management
Abstract
In contrast to public perception, the morbidity and mortality and the resultant healthcare costs associated with chronic heart failure (HF) are increasing and arguably reaching epidemic proportions. Although basic research efforts have provided unique insights into fundamental processes that govern myocardial extracellular matrix (ECM) growth and function, the translation of these findings to improved diagnostics and therapeutics for HF has not been as forthcoming. The factors that contribute to this relative paucity of new clinical tools for HF are multifactorial but likely include the need to recognize and differentiate HF phenotypes and to couple the use of biomarkers and multimodality imaging in early translational research studies. Recognizing the classification scheme of HF with a reduced ejection fraction (EF) to that of HF with a preserved EF and incorporating unique and differential measurements of ECM remodeling to these specific disease processes are warranted. For example, profiling pathways of ECM degradation such as the matrix metalloproteinases in patients with ischemic heart disease and HF with a reduced EF can provide prognostic information in terms of risk of progression to HF. In patients with chronic hypertensive disease and HF with a preserved EF, plasma profiling indexes of ECM synthesis and turnover, as well as advances in ECM imaging, have been shown to provide diagnostic and prognostic use. In terms of therapeutics, strategies to stabilize the ECM in HF with a reduced EF hold potential, whereas in contradistinction, selective antifibrotic agents may hold promise for HF with a preserved EF.
Keywords: cardiovascular diseases; diagnostics; myocardial remodeling; therapeutics; ventricular function.
Conflict of interest statement
Figures

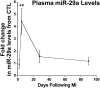
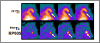


References
-
- Konstam MA, Kramer DG, Patel AR, Maron MS, Udelson JE. Left ventricular remodeling in heart failure: current concepts in clinical significance and assessment. JACC Cardiovasc Imaging. 2011 - PubMed
-
- Zile MR, Gaasch WH, Anand IS, Haass M, Little WC, Miller AB, Lopez-Sendon J, Teerlink JR, White M, McMurray JJ, Komajda M, McKelvie R, Ptaszynska A, Hetzel SJ, Massie BM, Carson PE. I-Preserve Investigators. Mode of death in patients with heart failure and a preserved ejection fraction: results from the Irbesartan in Heart Failure With Preserved Ejection Fraction Study (I-Preserve) trial. Circulation. 2010 - PubMed
-
- Alagiakrishnan K, Banach M, Jones LG, Datta S, Ahmed A, Aronow WS. Update on diastolic heart failure or heart failure with preserved ejection fraction in the older adults. Ann Med. 2013 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

