The application of intraoperative transit time flow measurement to accurately assess anastomotic quality in sequential vein grafting
- PMID: 24000314
- PMCID: PMC3829511
- DOI: 10.1093/icvts/ivt398
The application of intraoperative transit time flow measurement to accurately assess anastomotic quality in sequential vein grafting
Abstract
Objectives: Intraoperative transit time flow measurement (TTFM) is widely used to assess anastomotic quality in coronary artery bypass grafting (CABG). However, in sequential vein grafting, the flow characteristics collected by the conventional TTFM method are usually associated with total graft flow and might not accurately indicate the quality of every distal anastomosis in a sequential graft. The purpose of our study was to examine a new TTFM method that could assess the quality of each distal anastomosis in a sequential graft more reliably than the conventional TTFM approach.
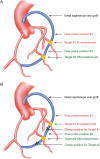
Methods: Two TTFM methods were tested in 84 patients who underwent sequential saphenous off-pump CABG in Beijing An Zhen Hospital between April and August 2012. In the conventional TTFM method, normal blood flow in the sequential graft was maintained during the measurement, and the flow probe was placed a few centimetres above the anastomosis to be evaluated. In the new method, blood flow in the sequential graft was temporarily reduced during the measurement by placing an atraumatic bulldog clamp at the graft a few centimetres distal to the anastomosis to be evaluated, while the position of the flow probe remained the same as in the conventional method. This new TTFM method was named the flow reduction TTFM. Graft flow parameters measured by both methods were compared.
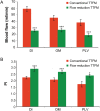
Results: Compared with the conventional TTFM, the flow reduction TTFM resulted in significantly lower mean graft blood flow (P < 0.05); in contrast, yielded significantly higher pulsatility index (P < 0.05). Diastolic filling was not significantly different between the two methods and was >50% in both cases. Interestingly, the flow reduction TTFM identified two defective middle distal anastomoses that the conventional TTFM failed to detect. Graft flows near the defective distal anastomoses were improved substantially after revision.
Conclusions: In this study, we found that temporary reduction of graft flow during TTFM seemed to enhance the sensitivity of TTFM to less-than-critical anastomotic defects in a sequential graft and to improve the overall accuracy of the intraoperative assessment of anastomotic quality in sequential vein grafting.
Keywords: Anastomotic quality; Sequential saphenous coronary artery bypass grafting; Transit time flow measurement.
Figures
Similar articles
-
Understanding coronary artery bypass transit time flow curves: role of bypass graft compliance.Interact Cardiovasc Thorac Surg. 2014 Feb;18(2):164-8. doi: 10.1093/icvts/ivt457. Epub 2013 Oct 30. Interact Cardiovasc Thorac Surg. 2014. PMID: 24174121 Free PMC article.
-
A novel transit-time flow metric, diastolic resistance index, detects subcritical anastomotic stenosis in coronary artery bypass grafting.JTCVS Tech. 2022 Dec 13;17:94-103. doi: 10.1016/j.xjtc.2022.11.013. eCollection 2023 Feb. JTCVS Tech. 2022. PMID: 36820345 Free PMC article.
-
Flow characteristics of LIMA radial composite sequential bypass grafting and single LIMA and saphenous vein sequential bypass grafting performed under OPCAB.J Cardiovasc Surg (Torino). 2012 Aug;53(4):537-44. J Cardiovasc Surg (Torino). 2012. PMID: 22854531
-
Transit time flow management as a management strategy in high-risk groups undergoing coronary artery bypass grafting.J Cardiothorac Surg. 2025 Mar 21;20(1):158. doi: 10.1186/s13019-025-03408-8. J Cardiothorac Surg. 2025. PMID: 40119360 Free PMC article. Review.
-
Techniques and standards in intraoperative graft verification by transit time flow measurement after coronary artery bypass graft surgery: a critical review.Eur J Cardiothorac Surg. 2017 Jan;51(1):26-33. doi: 10.1093/ejcts/ezw203. Epub 2016 Jun 13. Eur J Cardiothorac Surg. 2017. PMID: 27298393 Review.
Cited by
-
Intraoperative graft assessment during coronary artery bypass surgery.Gen Thorac Cardiovasc Surg. 2015 Mar;63(3):123-30. doi: 10.1007/s11748-014-0512-9. Epub 2015 Jan 6. Gen Thorac Cardiovasc Surg. 2015. PMID: 25556862 Review.
-
Assessment of the Graft Quality and Patency during and after Coronary Artery Bypass Grafting.Diagnostics (Basel). 2023 May 29;13(11):1891. doi: 10.3390/diagnostics13111891. Diagnostics (Basel). 2023. PMID: 37296743 Free PMC article. Review.
References
-
- Coronary artery surgery study (CASS) A randomized trial of coronary artery bypass surgery. Survival data. Circulation. 1983;68:939–50. doi:10.1161/01.CIR.68.5.939. - DOI - PubMed
-
- Magee MJ, Coombs LP, Peterson ED, Mack MJ. Patient selection and current practice strategy for off-pump coronary artery bypass surgery. Circulation. 2003;108:II9–14. - PubMed
-
- Emmert MY, Salzberg SP, Seifert B, Schurr UP, Hoerstrup SP, Reuthebuch O, et al. Routine off-pump coronary artery bypass grafting is safe and feasible in high-risk patients with left main disease. Ann Thorac Surg. 2010;89:1125–30. doi:10.1016/j.athoracsur.2009.12.059. - DOI - PubMed
-
- Kappetein AP, Feldman TE, Mack MJ, Morice MC, Holmes DR, Ståhle E, et al. Comparison of coronary bypass surgery with drug-eluting stenting for the treatment of left main and/or three-vessel disease: 3-year follow-up of the syntax trial. Eur Heart J. 2011;32:2125–34. doi:10.1093/eurheartj/ehr213. - DOI - PubMed
-
- Farsak B, Tokmakoglu H, Kandemir O, Günaydin S, Aydin H, Yorgancioglu C, et al. Angiographic assessment of sequential and individual coronary artery bypass grafting. J Card Surg. 2003;18:524–9. discussion 530–1 doi:10.1046/j.0886-0440.2003.02063.x. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

