Repeated intravenous doxapram induces phrenic motor facilitation
- PMID: 24013015
- PMCID: PMC3844021
- DOI: 10.1016/j.expneurol.2013.08.016
Repeated intravenous doxapram induces phrenic motor facilitation
Abstract
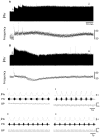
Doxapram is a respiratory stimulant used to treat hypoventilation. Here we investigated whether doxapram could also trigger respiratory neuroplasticity. Specifically, we hypothesized that intermittent delivery of doxapram at low doses would lead to long-lasting increases (i.e., facilitation) of phrenic motor output in anesthetized, vagotomized, and mechanically-ventilated rats. Doxapram was delivered intravenously in a single bolus (2 or 6mg/kg) or as a series of 3 injections (2mg/kg) at 5min intervals. Control groups received pH-matched saline injections (vehicle) or no treatment (anesthesia time control). Doxapram evoked an immediate increase in phrenic output in all groups, but a persistent increase in burst amplitude only occurred after repeated dosing with 2mg/kg. At 60min following the last injection, phrenic burst amplitude was 168±24% of baseline (%BL) in the group receiving 3 injections (P<0.05 vs. controls), but was 103±8%BL and 112±4%BL in the groups receiving a single dose of 2 or 6mg/kg, respectively. Following bilateral section of the carotid sinus nerves, the acute phrenic response to doxapram (2mg/kg) was reduced by 68% suggesting that at low doses the drug was acting primarily via the carotid chemoreceptors. We conclude that intermittent application of doxapram can trigger phrenic neuroplasticity, and this approach might be of use in the context of respiratory rehabilitation following neurologic injury.
Keywords: Doxapram; Phrenic motor facilitation; Respiratory neuroplasticity.
© 2013.
Figures

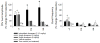
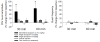
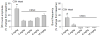
References
-
- Bach KB, Mitchell GS. Hypoxia-induced long-term facilitation of respiratory activity is serotonin dependent. Respir Physiol. 1996;104:251–260. - PubMed
-
- Baker TL, Fuller DD, Zabka AG, Mitchell GS. Respiratory plasticity: differential actions of continuous and episodic hypoxia and hypercapnia. Respir Physiol. 2001;129:25–35. - PubMed
-
- Bascom AT, Lattin CD, Aboussouan LS, Goshgarian HG. Effect of acute aminophylline administration on diaphragm function in high cervical tetraplegia: a case report. Chest. 2005;127:658–661. - PubMed
-
- Bavis RW, Mitchell GS. Intermittent hypoxia induces phrenic long-term facilitation in carotid-denervated rats. J Appl Physiol. 2003;94:399–409. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

