Docosahexaenoic acid supplementation alters key properties of cardiac mitochondria and modestly attenuates development of left ventricular dysfunction in pressure overload-induced heart failure
- PMID: 24013804
- PMCID: PMC4364545
- DOI: 10.1007/s10557-013-6487-4
Docosahexaenoic acid supplementation alters key properties of cardiac mitochondria and modestly attenuates development of left ventricular dysfunction in pressure overload-induced heart failure
Abstract
Purpose: Supplementation with the n3 polyunsaturated fatty acid docosahexaenoic acid (DHA) is beneficial in heart failure patients, however the mechanisms are unclear. DHA is incorporated into membrane phospholipids, which may prevent mitochondrial dysfunction. Thus we assessed the effects of DHA supplementation on cardiac mitochondria and the development of heart failure caused by aortic pressure overload.
Methods: Pathological cardiac hypertrophy was generated in rats by thoracic aortic constriction. Animals were fed either a standard diet or were supplemented with DHA (2.3 % of energy intake).
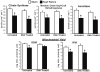
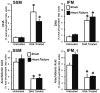
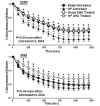
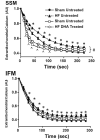
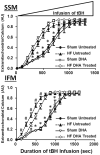
Results: After 14 weeks, heart failure was evident by left ventricular hypertrophy and chamber enlargement compared to shams. Left ventricle fractional shortening was unaffected by DHA treatment in sham animals (44.1 ± 1.6 % vs. 43.5 ± 2.2 % for standard diet and DHA, respectively), and decreased with heart failure in both treatment groups, but to a lesser extent in DHA treated animals (34.9 ± 1.7 %) than with the standard diet (29.7 ± 1.5 %, P < 0.03). DHA supplementation increased DHA content in mitochondrial phospholipids and decreased membrane viscosity. Myocardial mitochondrial oxidative capacity was decreased by heart failure and unaffected by DHA. DHA treatment enhanced Ca(2+) uptake by subsarcolemmal mitochondria in both sham and heart failure groups. Further, DHA lessened Ca(2+)-induced mitochondria swelling, an index of permeability transition, in heart failure animals. Heart failure increased hydrogen peroxide-induced mitochondrial permeability transition compared to sham, which was partially attenuated in interfibrillar mitochondria by treatment with DHA.
Conclusions: DHA decreased mitochondrial membrane viscosity and accelerated Ca(2+) uptake, and attenuated susceptibility to mitochondrial permeability transition and development of left ventricular dysfunction.
Figures
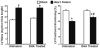
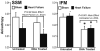
Similar articles
-
Feeding Docosahexaenoic Acid and Arachidonic Acid during Suckling and Weaning Contributes to Oral Tolerance Development by Beneficially Modulating the Intestinal Cytokine and Immunoglobulin Levels in an Allergy-Prone Brown Norway Rat Model.J Nutr. 2024 Dec;154(12):3790-3802. doi: 10.1016/j.tjnut.2024.10.021. Epub 2024 Oct 12. J Nutr. 2024. PMID: 39401683
-
Evaluation of docosahexaenoic acid in a dog model of hypertension induced left ventricular hypertrophy.J Cardiovasc Transl Res. 2013 Dec;6(6):1000-1010. doi: 10.1007/s12265-013-9511-y. Epub 2013 Sep 25. J Cardiovasc Transl Res. 2013. PMID: 24065618 Free PMC article.
-
Balancing mitochondrial dynamics via increasing mitochondrial fusion attenuates infarct size and left ventricular dysfunction in rats with cardiac ischemia/reperfusion injury.Clin Sci (Lond). 2019 Feb 12;133(3):497-513. doi: 10.1042/CS20190014. Print 2019 Feb 14. Clin Sci (Lond). 2019. Retraction in: Clin Sci (Lond). 2025 Jun 23;139(12):CS20190014_RET. doi: 10.1042/CS20190014_RET. PMID: 30705107 Retracted.
-
Coenzyme Q10 for heart failure.Cochrane Database Syst Rev. 2021 Feb 3;(2)(2):CD008684. doi: 10.1002/14651858.CD008684.pub3. Cochrane Database Syst Rev. 2021. PMID: 35608922 Free PMC article.
-
Dexrazoxane for preventing or reducing cardiotoxicity in adults and children with cancer receiving anthracyclines.Cochrane Database Syst Rev. 2022 Sep 27;9(9):CD014638. doi: 10.1002/14651858.CD014638.pub2. Cochrane Database Syst Rev. 2022. PMID: 36162822 Free PMC article.
Cited by
-
Long-chain omega-3 polyunsaturated fatty acids and the risk of heart failure.Ther Adv Chronic Dis. 2022 Mar 18;13:20406223221081616. doi: 10.1177/20406223221081616. eCollection 2022. Ther Adv Chronic Dis. 2022. PMID: 35321400 Free PMC article.
-
Cardiac mitochondrial proteome dynamics with heavy water reveals stable rate of mitochondrial protein synthesis in heart failure despite decline in mitochondrial oxidative capacity.J Mol Cell Cardiol. 2014 Oct;75:88-97. doi: 10.1016/j.yjmcc.2014.06.014. Epub 2014 Jul 1. J Mol Cell Cardiol. 2014. PMID: 24995939 Free PMC article.
-
An Effective Sodium-Dependent Glucose Transporter 2 Inhibition, Canagliflozin, Prevents Development of Hypertensive Heart Failure in Dahl Salt-Sensitive Rats.Front Pharmacol. 2022 Mar 9;13:856386. doi: 10.3389/fphar.2022.856386. eCollection 2022. Front Pharmacol. 2022. PMID: 35370704 Free PMC article.
-
Eicosapentaenoic Acid (EPA) and Docosahexaenoic Acid (DHA) Ameliorate Heart Failure through Reductions in Oxidative Stress: A Systematic Review and Meta-Analysis.Antioxidants (Basel). 2024 Aug 6;13(8):955. doi: 10.3390/antiox13080955. Antioxidants (Basel). 2024. PMID: 39199201 Free PMC article. Review.
-
Testosterone deficiency impairs cardiac interfibrillar mitochondrial function and myocardial contractility while inducing oxidative stress.Front Endocrinol (Lausanne). 2023 Sep 13;14:1206387. doi: 10.3389/fendo.2023.1206387. eCollection 2023. Front Endocrinol (Lausanne). 2023. PMID: 37780627 Free PMC article.
References
-
- Ghio S, Scelsi L, Latini R, Masson S, Eleuteri E, Palvarini M, et al. Effects of n 3 polyunsaturated fatty acids and of rosuvastatin on left ventricular function in chronic heart failure: a substudy of GISSI HF trial. Eur J Heart Fail. 2010;12:1345–53. - PubMed
-
- Gissi Hf I. Effect of n 3 polyunsaturated fatty acids in patients with chronic heart failure (the GISSI HF trial): a randomised, double blind, placebo controlled trial. Lancet. 2008;372:1223–30. - PubMed
-
- Nodari S, Triggiani M, Campia U, Manerba A, Milesi G, Cesana BM, et al. Effects of n 3 polyunsaturated fatty acids on left ventric ular function and functional capacity in patients with dilated cardio myopathy. J Am Coll Cardiol. 2011;57:870–9. - PubMed
-
- Moertl D, Hammer A, Steiner S, Hutuleac R, Vonbank K, Berger R. Dose dependent effects of omega 3 polyunsaturated fatty acids on systolic left ventricular function, endothelial function, and markers of inflammation in chronic heart failure of nonischemic origin: a double blind, placebo controlled, 3 arm study. Am Heart J. 2011;161:915–9. - PubMed
-
- Mozaffarian D, Wu JH. Omega 3 fatty acids and cardiovascular disease: effects on risk factors, molecular pathways, and clinical events. J Am Coll Cardiol. 2011;58:2047–67. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

