Different TLR4 expression and microglia/macrophage activation induced by hemorrhage in the rat spinal cord after compressive injury
- PMID: 24015844
- PMCID: PMC3847110
- DOI: 10.1186/1742-2094-10-112
Different TLR4 expression and microglia/macrophage activation induced by hemorrhage in the rat spinal cord after compressive injury
Abstract
Background: Hemorrhage is a direct consequence of traumatic injury to the central nervous system and may cause innate immune reactions including cerebral Toll-like receptor (TLR) 4 upregulation which usually leads to poor outcome in the traumatic brain injury. In spinal cord injury (SCI), however, how hemorrhage induces innate immune reaction in spinal parenchyma remains unknown. The present study aimed to see whether blood component and/or other factor(s) induce TLR4 and microglia/macrophages involved innate immune reactions in the rat spinal cord after traumatic injury.
Methods: Using the compressive SCI model of the rat, hemorrhage in the spinal cord was identified by hematoxylin-eosin staining. Microglia/macrophage activation, TLR4 expression, and cell apoptosis were investigated by immunohistochemistry. Nuclear factor (NF)-κB p50 level of the two segments of the cord was detected by western blotting assay. With carbon powder injection, blood origination of the hematoma was explored. The blood-spinal cord barrier (BSCB) states of the lesion site and the hematoma were compared with immunohistochemistry and tannic acid-ferric chloride staining.
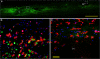
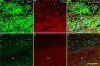
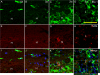
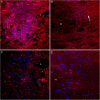
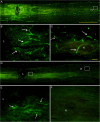
Results: Histological observation found blood accumulated in the center of compression lesion site (epicenter) and in the hematoma approximately 1.5 cm away from the epicenter. TLR4 expression, microglia//macrophage activation, and subsequent apoptosis in the area of far-away hematoma were late and weak in comparison to that in epicenter. In addition, TLR4 positive microglia/macrophages appeared to be phagocytotic in the far-away hematoma more obviously than that in the epicenter. Injected carbon powder indicated that accumulated blood of the far-away hematoma originated from the bleeding of the lesion epicenter, and the BSCB around the hematoma was not compromised in the early phase. Accordingly, at 3 days post injury, NF-κB p50 was upregulated based on the similar levels of blood component hemoglobin, and cell apoptosis was obvious in the epicenter but not in the far-away hematoma.
Conclusion: These data suggest that besides blood component, BSCB compromise and the extent of tissue injury contribute more to TLR4 and microglia/macrophage responses to the spinal cord hemorrhage. Therefore, the innate immune environment is a necessary consideration for the SCI therapy targeting TLR4 and microglia/macrophages.
Figures





Similar articles
-
MiR-100 suppresses inflammatory activation of microglia and neuronal apoptosis following spinal cord injury via TLR4/NF-κB pathway.Eur Rev Med Pharmacol Sci. 2019 Oct;23(20):8713-8720. doi: 10.26355/eurrev_201910_19265. Eur Rev Med Pharmacol Sci. 2019. PMID: 31696457
-
Macrophages in spinal cord injury: phenotypic and functional change from exposure to myelin debris.Glia. 2015 Apr;63(4):635-51. doi: 10.1002/glia.22774. Epub 2014 Nov 28. Glia. 2015. PMID: 25452166 Free PMC article.
-
MiR-27a ameliorates inflammatory damage to the blood-spinal cord barrier after spinal cord ischemia: reperfusion injury in rats by downregulating TICAM-2 of the TLR4 signaling pathway.J Neuroinflammation. 2015 Feb 7;12:25. doi: 10.1186/s12974-015-0246-3. J Neuroinflammation. 2015. PMID: 25876455 Free PMC article.
-
Ciprofloxacin and levofloxacin attenuate microglia inflammatory response via TLR4/NF-kB pathway.J Neuroinflammation. 2019 Jul 18;16(1):148. doi: 10.1186/s12974-019-1538-9. J Neuroinflammation. 2019. PMID: 31319868 Free PMC article. Review.
-
Time-dependent microglia and macrophages response after traumatic spinal cord injury in rat: a systematic review.Injury. 2020 Nov;51(11):2390-2401. doi: 10.1016/j.injury.2020.07.007. Epub 2020 Jul 7. Injury. 2020. PMID: 32665068
Cited by
-
Critical role of regulator of calcineurin 1 in spinal cord injury.J Physiol Biochem. 2016 Dec;72(4):605-613. doi: 10.1007/s13105-016-0499-z. Epub 2016 Jun 23. J Physiol Biochem. 2016. PMID: 27339639
-
CNS Macrophages and Infant Infections.Front Immunol. 2020 Sep 18;11:2123. doi: 10.3389/fimmu.2020.02123. eCollection 2020. Front Immunol. 2020. PMID: 33072074 Free PMC article. Review.
-
Heme: The Lord of the Iron Ring.Antioxidants (Basel). 2023 May 10;12(5):1074. doi: 10.3390/antiox12051074. Antioxidants (Basel). 2023. PMID: 37237940 Free PMC article. Review.
-
Down-Regulation of CXCL12/CXCR4 Expression Alleviates Ischemia-Reperfusion-Induced Inflammatory Pain via Inhibiting Glial TLR4 Activation in the Spinal Cord.PLoS One. 2016 Oct 19;11(10):e0163807. doi: 10.1371/journal.pone.0163807. eCollection 2016. PLoS One. 2016. PMID: 27760212 Free PMC article.
-
Inosine Improves Functional Recovery and Cell Morphology Following Compressive Spinal Cord Injury in Mice.Neurotrauma Rep. 2024 Oct 2;5(1):957-968. doi: 10.1089/neur.2024.0081. eCollection 2024. Neurotrauma Rep. 2024. PMID: 39464528 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

