THD Doppler procedure for hemorrhoids: the surgical technique
- PMID: 24026315
- PMCID: PMC3950605
- DOI: 10.1007/s10151-013-1062-3
THD Doppler procedure for hemorrhoids: the surgical technique
Abstract
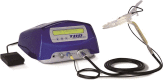
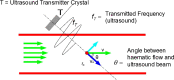
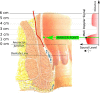
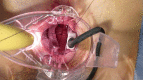
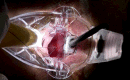
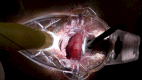
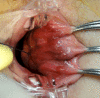
Transanal hemorrhoidal dearterialization (THD) is an effective treatment for hemorrhoidal disease. The ligation of hemorrhoidal arteries (called "dearterialization") can provide a significant reduction of the arterial overflow to the hemorrhoidal piles. Plication of the redundant rectal mucosa/submucosa (called "mucopexy") can provide a repositioning of prolapsing tissue to the anatomical site. In this paper, the surgical technique and perioperative patient management are illustrated. Following adequate clinical assessment, patients undergo THD under general or spinal anesthesia, in either the lithotomy or the prone position. In all patients, distal Doppler-guided dearterialization is performed, providing the selective ligation of hemorrhoidal arteries identified by Doppler. In patients with hemorrhoidal/muco-hemorrhoidal prolapse, the mucopexy is performed with a continuous suture including the redundant and prolapsing mucosa and submucosa. The description of the surgical procedure is complemented by an accompanying video (see supplementary material). In long-term follow-up, there is resolution of symptoms in the vast majority of patients. The most common complication is transient tenesmus, which sometimes can result in rectal discomfort or pain. Rectal bleeding occurs in a very limited number of patients. Neither fecal incontinence nor chronic pain should occur. Anorectal physiology parameters should be unaltered, and anal sphincters should not be injured by following this procedure. When accurately performed and for the correct indications, THD is a safe procedure and one of the most effective treatments for hemorrhoidal disease.
Figures



References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

