Predictors of morbidity and mortality after hepatectomy in elderly patients: analysis of 7621 NSQIP patients
- PMID: 24033514
- PMCID: PMC4008164
- DOI: 10.1111/hpb.12155
Predictors of morbidity and mortality after hepatectomy in elderly patients: analysis of 7621 NSQIP patients
Abstract
Objectives: Increasingly, surgeons are performing hepatectomies in older patients. This study was designed to analyse the incidences of and risk factors for post-hepatectomy morbidity and mortality in elderly patients.
Methods: All elective hepatectomies for the period 2005-2010 recorded in the American College of Surgeons (ACS) National Surgical Quality Improvement Program (NSQIP) database were evaluated. Factors associated with 30-day rates of morbidity and mortality were compared between patients aged ≥75 years and those aged <75 years.
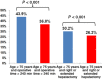
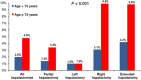
Results: Elderly patients accounted for 894 of 7621 (11.7%) hepatectomies. These patients more frequently had comorbidities (diabetes, cardiovascular or lung disease, lower albumin, elevated creatinine, anaesthesia risk; all P < 0.05) and were more likely to undergo partial or left rather than right or extended hepatectomies (P = 0.013). Despite the lesser surgical magnitude of these procedures, elderly patients experienced higher rates of severe complications (23.9% versus 18.4%; P < 0.001) and overall postoperative mortality (4.8% versus 2.0%; P < 0.001). The occurrence of any severe complication was associated with a mortality rate of 20.1% in elderly patients and 10.8% in non-elderly patients (P < 0.001). This disparity in mortality was more pronounced in patients with two or more (31.7% versus 20.2%; P < 0.001) and three or more (46.3% versus 31.1%; P < 0.001) severe complications. Independent risk factors for severe complications and/or mortality included an albumin level of < 4 g/dl, lung disease, intraoperative transfusion, a concurrent intra-abdominal operation, and an operative time of >240 min (all P < 0.05).
Conclusions: Given their lower physiologic reserve, elderly patients are at much greater risk for mortality after severe complications. To improve outcomes, surgeons should balance age and preoperative comorbidities with magnitude of hepatectomy.
© 2013 International Hepato-Pancreato-Biliary Association.
Figures



References
-
- Andres A, Toso C, Moldovan B, Schiffer E, Rubbia-Brandt L, Terraz S, et al. Complications of elective liver resections in a centre with low mortality: a simple score to predict morbidity. Arch Surg. 2011;146:1246–1252. - PubMed
-
- Zimmitti G, Roses RE, Andreou A, Shindoh J, Curley SA, Aloia TA, et al. Greater complexity of liver surgery is not associated with an increased incidence of liver-related complications except for bile leak: an experience with 2628 consecutive resections. J Gastrointest Surg. 2013;17:57–64. discussion 64–65. - PMC - PubMed
-
- Madoff DC, Abdalla EK, Vauthey JN. Portal vein embolization in preparation for major hepatic resection: evolution of a new standard of care. J Vasc Interv Radiol. 2005;16:779–790. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

