Incidental, subsolid pulmonary nodules at CT: etiology and management
- PMID: 24061063
- PMCID: PMC3800431
- DOI: 10.1102/1470-7330.2013.9025
Incidental, subsolid pulmonary nodules at CT: etiology and management
Abstract
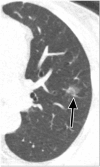
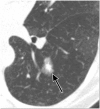
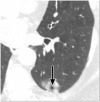
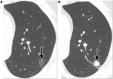
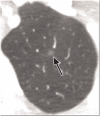
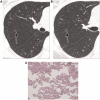
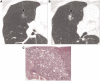
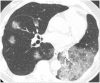
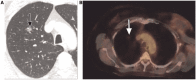
Pulmonary nodules, both solid and subsolid, are common incidental findings on computed tomography (CT) studies. Subsolid nodules (SSNs) may be further classified as either pure ground-glass nodules or part-solid nodules. The differential diagnosis for an SSN is broad, including infection, organizing pneumonia, inflammation, hemorrhage, focal fibrosis, and neoplasm. Adenocarcinomas of the lung are currently the most common type of lung cancer, representing 30-35% of all primary lung tumors, and the subtype of bronchioloalveolar cell carcinoma (BAC) commonly presents as an SSN. In 2011, a new classification system for lung adenocarcinomas was proposed by the International Association for the Study of Lung Cancer, the American Thoracic Society, and the European Respiratory Society. An important feature of the new system is the relinquishment of the term BAC in favor of more specific histologic subtypes. It has been reported that these subtypes are associated with characteristic CT findings. This article reviews the new classification system of lung adenocarcinomas, discusses and illustrates the associated CT findings, and outlines the current recommendations for further diagnosis, treatment, and follow-up of SSNs based on computed tomography findings.
Figures


Similar articles
-
Overview and strategic management of subsolid pulmonary nodules.J Thorac Imaging. 2012 Jul;27(4):240-8. doi: 10.1097/RTI.0b013e31825d515b. J Thorac Imaging. 2012. PMID: 22847591 Review.
-
Nodule characterization: subsolid nodules.Radiol Clin North Am. 2014 Jan;52(1):47-67. doi: 10.1016/j.rcl.2013.08.011. Epub 2013 Oct 6. Radiol Clin North Am. 2014. PMID: 24267710
-
A Subsolid Nodules Imaging Reporting System (SSN-IRS) for Classifying 3 Subtypes of Pulmonary Adenocarcinoma.Clin Lung Cancer. 2020 Jul;21(4):314-325.e4. doi: 10.1016/j.cllc.2020.01.014. Epub 2020 Feb 6. Clin Lung Cancer. 2020. PMID: 32273256
-
Subsolid pulmonary nodules and the spectrum of peripheral adenocarcinomas of the lung: recommended interim guidelines for assessment and management.Radiology. 2009 Dec;253(3):606-22. doi: 10.1148/radiol.2533090179. Radiology. 2009. PMID: 19952025 Review.
-
Imaging and Management of Subsolid Lung Nodules.Radiol Clin North Am. 2025 Jul;63(4):517-535. doi: 10.1016/j.rcl.2024.12.002. Epub 2025 Jan 24. Radiol Clin North Am. 2025. PMID: 40409933 Review.
Cited by
-
[Diagnosis and Treatment of Pulmonary Ground-glass Nodules].Zhongguo Fei Ai Za Zhi. 2019 Jul 20;22(7):449-456. doi: 10.3779/j.issn.1009-3419.2019.07.07. Zhongguo Fei Ai Za Zhi. 2019. PMID: 31315784 Free PMC article. Review. Chinese.
-
Lung Cancer Screening, Version 3.2018, NCCN Clinical Practice Guidelines in Oncology.J Natl Compr Canc Netw. 2018 Apr;16(4):412-441. doi: 10.6004/jnccn.2018.0020. J Natl Compr Canc Netw. 2018. PMID: 29632061 Free PMC article. Review.
-
Neutrophil-Lymphocyte Ratio as a Predictive Factor of Growing Malignant Pulmonary Ground-glass Opacity.Cancer Manag Res. 2021 Jul 13;13:5651-5655. doi: 10.2147/CMAR.S319190. eCollection 2021. Cancer Manag Res. 2021. PMID: 34285585 Free PMC article.
-
[Combined use of thin-section CT and 18F-FDG PET/CT for characterization of solitary pulmonary nodules].Nan Fang Yi Ke Da Xue Xue Bao. 2017 Mar 20;37(3):283-289. doi: 10.3969/j.issn.1673-4254.2017.03.01. Nan Fang Yi Ke Da Xue Xue Bao. 2017. PMID: 28377340 Free PMC article.
-
Lymphadenectomy is Unnecessary for Pure Ground-Glass Opacity Pulmonary Nodules.J Clin Med. 2020 Mar 2;9(3):672. doi: 10.3390/jcm9030672. J Clin Med. 2020. PMID: 32131524 Free PMC article.
References
-
- Austin JH, Garg K, Aberle D, Yankelevitz D, et al. Radiologic implications of the 2011 classification of adenocarcinoma of the lung. Radiology. 2013;266:62–71. - PubMed
-
- Wallis A, Chandratreya L, Bhatt N, Edey A. Imaging bronchogenic adenocarcinoma: emerging concepts. J Comput Assist Tomogr. 2012;36:629–635. - PubMed
-
- Gould MK, Maclean CC, Kuschner WG, Rydzak CE, Owens DK. Accuracy of positron emission tomography for diagnosis of pulmonary nodules and mass lesions: a meta-analysis. JAMA. 2001;285:914–924. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
