The plastic nature of the human bone-periodontal ligament-tooth fibrous joint
- PMID: 24063947
- PMCID: PMC3938967
- DOI: 10.1016/j.bone.2013.09.007
The plastic nature of the human bone-periodontal ligament-tooth fibrous joint
Abstract
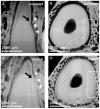
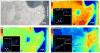
This study investigates bony protrusions within a narrowed periodontal ligament space (PDL-space) of a human bone-PDL-tooth fibrous joint by mapping structural, biochemical, and mechanical heterogeneity. Higher resolution structural characterization was achieved via complementary atomic force microscopy (AFM), nano-transmission X-ray microscopy (nano-TXM), and microtomography (MicroXCT™). Structural heterogeneity was correlated to biochemical and elemental composition, illustrated via histochemistry and microprobe X-ray fluorescence analysis (μ-XRF), and mechanical heterogeneity evaluated by AFM-based nanoindentation. Results demonstrated that the narrowed PDL-space was due to invasion of bundle bone (BB) into PDL-space. Protruded BB had a wider range with higher elastic modulus values (2-8GPa) compared to lamellar bone (0.8-6GPa), and increased quantities of Ca, P and Zn as revealed by μ-XRF. Interestingly, the hygroscopic 10-30μm interface between protruded BB and lamellar bone exhibited higher X-ray attenuation similar to cement lines and lamellae within bone. Localization of the small leucine rich proteoglycan biglycan (BGN) responsible for mineralization was observed at the PDL-bone interface and around the osteocyte lacunae. Based on these results, it can be argued that the LB-BB interface was the original site of PDL attachment, and that the genesis of protruded BB identified as protrusions occurred as a result of shift in strain. We emphasize the importance of bony protrusions within the context of organ function and that additional study is warranted.
Keywords: Alveolar bone; Bone functional adaptation; Bone–PDL–tooth fibrous joint; Bundle bone; Discontinuities; Periodontal ligament.
© 2013. Published by Elsevier Inc. All rights reserved.
Figures






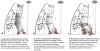
Similar articles
-
Multiscale biomechanical responses of adapted bone-periodontal ligament-tooth fibrous joints.Bone. 2015 Dec;81:196-207. doi: 10.1016/j.bone.2015.07.004. Epub 2015 Jul 4. Bone. 2015. PMID: 26151121 Free PMC article.
-
Discontinuities in the human bone-PDL-cementum complex.Biomaterials. 2011 Oct;32(29):7106-17. doi: 10.1016/j.biomaterials.2011.06.021. Epub 2011 Jul 20. Biomaterials. 2011. PMID: 21774982 Free PMC article.
-
The biomechanical characteristics of the bone-periodontal ligament-cementum complex.Biomaterials. 2010 Sep;31(25):6635-46. doi: 10.1016/j.biomaterials.2010.05.024. Epub 2010 Jun 11. Biomaterials. 2010. PMID: 20541802 Free PMC article.
-
A Force on the Crown and Tug of War in the Periodontal Complex.J Dent Res. 2018 Mar;97(3):241-250. doi: 10.1177/0022034517744556. Epub 2018 Jan 24. J Dent Res. 2018. PMID: 29364757 Free PMC article. Review.
-
Biomechanical pathways of dentoalveolar fibrous joints in health and disease.Periodontol 2000. 2020 Feb;82(1):238-256. doi: 10.1111/prd.12306. Periodontol 2000. 2020. PMID: 31850635 Review.
Cited by
-
Multiscale biomechanical responses of adapted bone-periodontal ligament-tooth fibrous joints.Bone. 2015 Dec;81:196-207. doi: 10.1016/j.bone.2015.07.004. Epub 2015 Jul 4. Bone. 2015. PMID: 26151121 Free PMC article.
-
Mineral density volume gradients in normal and diseased human tissues.PLoS One. 2015 Apr 9;10(4):e0121611. doi: 10.1371/journal.pone.0121611. eCollection 2015. PLoS One. 2015. PMID: 25856386 Free PMC article.
-
The Mechanical Effect of the Periodontal Ligament on Bone Strain Regimes in a Validated Finite Element Model of a Macaque Mandible.Front Bioeng Biotechnol. 2019 Oct 30;7:269. doi: 10.3389/fbioe.2019.00269. eCollection 2019. Front Bioeng Biotechnol. 2019. PMID: 31737614 Free PMC article.
-
Mechanoadaptive Responses in the Periodontium Are Coordinated by Wnt.J Dent Res. 2019 Jun;98(6):689-697. doi: 10.1177/0022034519839438. Epub 2019 Apr 10. J Dent Res. 2019. PMID: 30971171 Free PMC article.
-
Effect of proteoglycans at interfaces as related to location, architecture, and mechanical cues.Arch Oral Biol. 2016 Mar;63:82-92. doi: 10.1016/j.archoralbio.2015.11.021. Epub 2015 Dec 3. Arch Oral Biol. 2016. PMID: 26741830 Free PMC article.
References
-
- Nanci A. Ten Cate’s Oral Histology. Mosby Elsevier; St. Louis: 2008.
-
- van den Bos T, Beertsen W. Alkaline phosphatase activity in human periodontal ligament: age effect and relation to cementum growth rate. J Periodontal Res. 1999;34:1–6. - PubMed
-
- Thompson DW. On Growth and Form. Cambridge University Press; 1961. On form and mechanical efficiency; p. 221.
-
- Wolff J. The law of bone remodelling. Springer Verlag; Berlin: 1986.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

