Intracoronary fixed dose of nitroprusside via thrombus aspiration catheter for the prevention of the no-reflow phenomenon following primary percutaneous coronary intervention in acute myocardial infarction
- PMID: 24137212
- PMCID: PMC3786843
- DOI: 10.3892/etm.2013.1139
Intracoronary fixed dose of nitroprusside via thrombus aspiration catheter for the prevention of the no-reflow phenomenon following primary percutaneous coronary intervention in acute myocardial infarction
Abstract
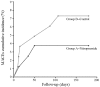
Previous studies have shown that intracoronary (IC) nitroprusside (NTP) injection is a safe and effective strategy for the treatment of no-reflow (NR) during percutaneous coronary intervention (PCI). The present study tested the hypothesis that, on the basis of thrombus aspiration for the treatment of ST-segment elevation myocardial infarction (STEMI), the selective IC administration of a fixed dose of NTP (100 μg) plus tirofiban is a safe and superior treatment method compared with the IC administration of tirofiban alone for the prevention of NR during primary PCI. A total of 162 consecutive patients with STEMI, who underwent primary PCI within 12 h of onset, were randomly assigned to two groups: Group A, IC administration of a fixed dose of NTP (100 μg) plus tirofiban (10 μg/kg) and group B, IC administration of tirofiban (10 μg/kg) alone (n=80 and n=82, respectively). The drugs were selectively injected into the infarct-related artery (IRA) via a thrombus aspiration catheter advanced into the IRA. The primary end-point was post-procedural corrected thrombolysis in myocardial infarction (TIMI) frame count (CTFC). The proportion of complete (>70%) ST-segment resolution (STR); the TIMI myocardial perfusion grade (TMPG) 2-3 ratio following PCI; the peak value of creatine kinase (CK)-MB; the TIMI flow grade; the incidence of major adverse cardiac events (MACEs) and the left ventricular ejection fraction (LVEF) after 6 months of follow-up were observed as the secondary end-points. There were no significant differences in the baseline clinical and angiographic characteristics between the two groups. Compared with group B, group A had i) a lower CTFC (23±7 versus 29±11, P=0.000); ii) a higher proportion of complete STR (72.5 versus 55.9%, P=0.040); iii) an enhanced TMPG 2-3 ratio (71.3 versus 53.7%, P=0.030) and iv) a lower peak CK-MB value (170±56 versus 210±48 U/l, P=0.010). There were no statistically significant differences in the final TIMI grade-3 flow between the two groups (92.5 versus 91.5% for groups A and B, respectively; P=0.956). The LVEF at 6 months was higher in group A than group B (63±9 versus 53±11%, respectively; P=0.001); however, the incidence of MACEs was not statistically different between the two groups, although there was a trend indicating improvement in group A (log rank χ2=0.953, P=0.489). The selective IC administration of a fixed dose of NTP (100 μg) plus tirofiban via a thrombus aspiration catheter advanced into the IRA is a safe and superior treatment method compared with tirofiban alone in patients with STEMI undergoing primary PCI. This novel therapeutic strategy improves the myocardial level perfusion, in addition to reducing the infarct size. Furthermore, it may improve the postoperative clinical prognosis following PCI.
Keywords: ST elevation myocardial infarction; nitroprusside; no-reflow; thrombus aspiration; tirofiban.
Figures
Similar articles
-
Thrombus aspiration plus intra-infarct-related artery administration of tirofiban improves myocardial perfusion during primary angioplasty for acute myocardial infarction.Chin Med J (Engl). 2010 Apr 5;123(7):877-83. Chin Med J (Engl). 2010. PMID: 20497681 Clinical Trial.
-
Effects of intracoronary injection of nicorandil and tirofiban on myocardial perfusion and short-term prognosis in elderly patients with acute ST-segment elevation myocardial infarction after emergency PCI.World J Emerg Med. 2020;11(3):157-163. doi: 10.5847/wjem.j.1920-8642.2020.03.005. World J Emerg Med. 2020. PMID: 32351648 Free PMC article.
-
[Efficacy comparison of combined intracoronary administration of high-dose adenosine and tirofiban versus intracoronary tirofiban during primary percutaneous coronary intervention in patients with acute myocardial infarction].Zhonghua Xin Xue Guan Bing Za Zhi. 2013 Oct;41(10):839-44. Zhonghua Xin Xue Guan Bing Za Zhi. 2013. PMID: 24377889 Clinical Trial. Chinese.
-
Effect of intracoronary nitroprusside in preventing no reflow phenomenon during primary percutaneous coronary intervention: a meta-analysis.J Interv Cardiol. 2014 Aug;27(4):356-64. doi: 10.1111/joic.12133. Epub 2014 Jul 8. J Interv Cardiol. 2014. PMID: 25041036 Review.
-
Efficacy and safety of intracoronary pro-urokinase injection during percutaneous coronary intervention in treating ST elevation myocardial infarction patients: a systematic review and meta-analysis of randomized controlled trials.Eur Rev Med Pharmacol Sci. 2022 Aug;26(16):5802-5813. doi: 10.26355/eurrev_202208_29518. Eur Rev Med Pharmacol Sci. 2022. PMID: 36066155
Cited by
-
Pathophysiology, Diagnosis, and Management of Coronary No-Reflow Phenomenon.Int J Angiol. 2022 Jan 13;31(2):107-112. doi: 10.1055/s-0041-1735949. eCollection 2022 Jun. Int J Angiol. 2022. PMID: 35864888 Free PMC article.
-
Intracoronary administration of anisodamine and nicorandil in individuals undergoing primary percutaneous coronary intervention for acute inferior myocardial infarction: A randomized factorial trial.Exp Ther Med. 2015 Sep;10(3):1059-1065. doi: 10.3892/etm.2015.2623. Epub 2015 Jul 7. Exp Ther Med. 2015. PMID: 26622439 Free PMC article.
-
The REFLO-STEMI trial comparing intracoronary adenosine, sodium nitroprusside and standard therapy for the attenuation of infarct size and microvascular obstruction during primary percutaneous coronary intervention: study protocol for a randomised controlled trial.Trials. 2014 Sep 25;15:371. doi: 10.1186/1745-6215-15-371. Trials. 2014. PMID: 25252600 Free PMC article. Clinical Trial.
-
Pathophysiology and Treatment of the No-Reflow Phenomenon in ST-Segment Elevation Myocardial Infarction: Focus on Low-Dose Fibrinolysis during Primary Percutaneous Intervention.Rev Cardiovasc Med. 2023 Dec 25;24(12):365. doi: 10.31083/j.rcm2412365. eCollection 2023 Dec. Rev Cardiovasc Med. 2023. PMID: 39077094 Free PMC article. Review.
-
"No-Reflow" Phenomenon: A Contemporary Review.J Clin Med. 2022 Apr 16;11(8):2233. doi: 10.3390/jcm11082233. J Clin Med. 2022. PMID: 35456326 Free PMC article. Review.
References
-
- Grines CL, Browne KF, Marco J, et al. The Primary Angioplasty in Myocardial Infarction Study Group A comparison of primary angioplasty with thrombolytic therapy for acute myocardial infarction. N Engl J Med. 1993;328:673–679. - PubMed
-
- Lee CH, Tse HF. Microvascular obstruction after percutaneous coronary intervention. Catheter Cardiovasc Interv. 2010;75:369–377. - PubMed
-
- Eeckhout E, Kern MJ. The coronary no-reflow phenomenon: a review of mechanisms and therapies. Eur Heart J. 2001;22:729–739. - PubMed
-
- Tesic MB, Stankovic G, Vukcevic V, Ostojic MC. The use of intracoronary sodium nitroprusside to treat no-reflow after primary percutaneous coronary intervention in acute myocardial infarction. Herz. 2010;35:114–118. - PubMed
-
- Burzotta F, Trani C, Romagnoli E, et al. Manual thrombus-aspiration improves myocardial reperfusion: the randomized evaluation of the effect of mechanical reduction of distal embolization by thrombus-aspiration in primary and rescue angioplasty (REMEDIA) trial. J Am Coll Cardiol. 2005;46:371–376. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous