Functional connectivity between the amygdala and prefrontal cortex in medication-naive individuals with major depressive disorder
- PMID: 24148846
- PMCID: PMC3819156
- DOI: 10.1503/jpn.120117
Functional connectivity between the amygdala and prefrontal cortex in medication-naive individuals with major depressive disorder
Abstract
Background: Convergent evidence suggests dysfunction within the prefrontal cortex (PFC) and amygdala, important components of a neural system that subserves emotional processing, in individuals with major depressive disorder (MDD). Abnormalities in this system in the left hemisphere and during processing of negative emotional stimuli are especially implicated. In this study, we used functional magnetic resonance imaging (fMRI) to investigate amygdala-PFC functional connectivity during emotional face processing in medication-naive individuals with MDD.
Methods: Individuals with MDD and healthy controls underwent fMRI scanning while processing 3 types of emotional face stimuli. We compared the strength of functional connectivity from the amygdala between the MDD and control groups.
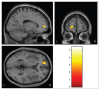
Results: Our study included 28 individuals with MDD and 30 controls. Decreased amygdala-left rostral PFC (rPFC) functional connectivity was observed in the MDD group compared with controls for the fear condition (p < 0.05, corrected). No significant differences were found in amygdala connectivity to any cerebral regions between the MDD and control groups for the happy or neutral conditions.
Limitations: All participants with MDD were experiencing acute episodes, therefore the findings could not be generalized to the entire MDD population.
Conclusion: Medication-naive individuals with MDD showed decreased amygdala-left rPFC functional connectivity in response to negative emotional stimuli, suggesting that abnormalities in amygdala-left rPFC neural circuitry responses to negative emotional stimuli might play an important role in the pathophysiology of MDD.
Figures
Similar articles
-
Decreased functional connectivity between the amygdala and the left ventral prefrontal cortex in treatment-naive patients with major depressive disorder: a resting-state functional magnetic resonance imaging study.Psychol Med. 2013 Sep;43(9):1921-7. doi: 10.1017/S0033291712002759. Epub 2012 Nov 30. Psychol Med. 2013. PMID: 23194671
-
Failure to regulate: counterproductive recruitment of top-down prefrontal-subcortical circuitry in major depression.J Neurosci. 2007 Aug 15;27(33):8877-84. doi: 10.1523/JNEUROSCI.2063-07.2007. J Neurosci. 2007. PMID: 17699669 Free PMC article.
-
Functional connectivity of emotional processing in depression.J Affect Disord. 2011 Nov;134(1-3):272-9. doi: 10.1016/j.jad.2011.06.021. Epub 2011 Jul 14. J Affect Disord. 2011. PMID: 21757239
-
A review of fMRI studies during visual emotive processing in major depressive disorder.World J Biol Psychiatry. 2015 Oct;16(7):448-71. doi: 10.3109/15622975.2014.885659. Epub 2014 Mar 17. World J Biol Psychiatry. 2015. PMID: 24635551 Review.
-
Major depressive disorder associated alterations in the effective connectivity of the face processing network: a systematic review.Transl Psychiatry. 2024 Jan 25;14(1):62. doi: 10.1038/s41398-024-02734-0. Transl Psychiatry. 2024. PMID: 38272868 Free PMC article.
Cited by
-
The Comorbidity Between Internet Gaming Disorder and Depression: Interrelationship and Neural Mechanisms.Front Psychiatry. 2018 Apr 23;9:154. doi: 10.3389/fpsyt.2018.00154. eCollection 2018. Front Psychiatry. 2018. PMID: 29740358 Free PMC article.
-
Why are cortical GABA neurons relevant to internal focus in depression? A cross-level model linking cellular, biochemical and neural network findings.Mol Psychiatry. 2014 Sep;19(9):966-977. doi: 10.1038/mp.2014.68. Epub 2014 Jul 22. Mol Psychiatry. 2014. PMID: 25048001 Free PMC article.
-
Development of Neuroimaging-Based Biomarkers in Major Depression.Adv Exp Med Biol. 2021;1305:85-99. doi: 10.1007/978-981-33-6044-0_6. Adv Exp Med Biol. 2021. PMID: 33834396
-
Structural and Functional Abnormities of Amygdala and Prefrontal Cortex in Major Depressive Disorder With Suicide Attempts.Front Psychiatry. 2020 Jan 8;10:923. doi: 10.3389/fpsyt.2019.00923. eCollection 2019. Front Psychiatry. 2020. PMID: 31969839 Free PMC article.
-
Altered Resting State Effective Connectivity of Anterior Insula in Depression.Front Psychiatry. 2018 Mar 15;9:83. doi: 10.3389/fpsyt.2018.00083. eCollection 2018. Front Psychiatry. 2018. PMID: 29599728 Free PMC article.
References
-
- Quirk GJ, Beer JS. Prefrontal involvement in the regulation of emotion: convergence of rat and human studies. Curr Opin Neurobiol. 2006;16:723–7. - PubMed
-
- Phillips ML, Young AW, Senior C, et al. A specific neural substrate for perceiving facial expressions of disgust. Nature. 1997;389:495–8. - PubMed
-
- Tang Y, Wang F, Xie G, et al. Reduced ventral anterior cingulate and amygdala volumes in medication-naive females with major depressive disorder: a voxel-based morphometric magnetic resonance imaging study. Psychiatry Res. 2007;156:83–6. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous
