Sagittal balance and spinopelvic parameters after lateral lumbar interbody fusion for degenerative scoliosis: a case-control study
- PMID: 24150436
- PMCID: PMC4340477
- DOI: 10.1097/BRS.0000000000000073
Sagittal balance and spinopelvic parameters after lateral lumbar interbody fusion for degenerative scoliosis: a case-control study
Abstract
Study design: Retrospective matched-cohort analysis.
Objective: To evaluate the change in radiographical parameters in patients undergoing interbody fusion and posterior instrumentation compared with posterior spine fusion (PSF) alone for degenerative scoliosis.
Summary of background data: Little is known about the effect of lateral interbody fusion (LIF) on sagittal plane correction in the setting of degenerative scoliosis. We performed a retrospective study to investigate these changes compared with PSF.
Methods: Between 1997 and 2011, 33 patients had LIF at 181 levels between T8 and L5 vertebrae for the treatment of degenerative scoliosis (mean; 5 ± 2 levels). Of those, 23 patients had additional anterior lumbar interbody fusion (ALIF) at 37 levels between L4 and S1 vertebrae (mean; 1.6 ± 0.5 levels). A 1:1 matched control of patients who underwent PSF was performed. Patients were matched by age, sex, and diagnosis. Clinical and radiographical data were collected and compared between the matched cohorts.
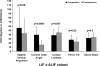
Results: Lumbar lordosis (LL) was significantly restored in the LIF ± ALIF compared with PSF cohort (44° ± 14° vs. 36° ± 15°, P = 0.02). The segmental LL over the 102 LIF levels significantly improved from 12°± 10° to 21°± 13° postoperatively (P < 0.0001). However, the change over the 37 ALIF levels was not significant (from 30° ± 15° to 29° ± 9°, P = 0.8). Sagittal plane alignment was improved in the LIF ± ALIF compared with PSF cohort and trended toward but did not reach significance (3.8 ± 3.2 cm vs. 6.2 ± 5.7 cm, P = 0.09). Sacral slope was significantly higher in the LIF ± ALIF compared with PSF cohort (33° ± 11° vs. 28° ± 10°, P = 0.03). Pelvic tilt was lower in the LIF ± ALIF compared with PSF cohort and trended toward but did not reach significance (22° ± 10° vs. 26° ± 10°, P = 0.08).
Conclusion: LL and sacral slope had mildly but statistically improved in the interbody fusion cohort compared with PSF cohort. Sagittal alignment and pelvic tilt trended toward but did not reach statistical significance. Segmental LL was improved at LIF levels more than at ALIF levels.
Level of evidence: 3.
Figures
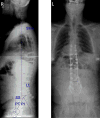
| Coronal Cobb angle (°) | SVA | LL | PT | SS | PI | |
| Preoperative | 15° | 13 cm | 43° | 33° | 34° | 67° |
| Postoperative | 6° | 4.1 cm | 57° | 29° | 35° | 64° |
| Sagittal Vertical Alignment (SVA), Lumbar Lordosis (LL), Pelvic Tilt (PT), Sacral Slope (SS), and Pelvic Incidence (PI). | ||||||

| Coronal Cobb angle (°) | SVA | LL | PT | SS | PI | |
| Preoperative | 15° | 13 cm | 43° | 33° | 34° | 67° |
| Postoperative | 6° | 4.1 cm | 57° | 29° | 35° | 64° |
| Sagittal Vertical Alignment (SVA), Lumbar Lordosis (LL), Pelvic Tilt (PT), Sacral Slope (SS), and Pelvic Incidence (PI). | ||||||

Similar articles
-
Utility of multilevel lateral interbody fusion of the thoracolumbar coronal curve apex in adult deformity surgery in combination with open posterior instrumentation and L5-S1 interbody fusion: a case-matched evaluation of 32 patients.J Neurosurg Spine. 2017 Feb;26(2):208-219. doi: 10.3171/2016.8.SPINE151543. Epub 2016 Oct 21. J Neurosurg Spine. 2017. PMID: 27767682
-
Comparative analysis of 3 surgical strategies for adult spinal deformity with mild to moderate sagittal imbalance.J Neurosurg Spine. 2018 Jan;28(1):40-49. doi: 10.3171/2017.5.SPINE161370. Epub 2017 Nov 3. J Neurosurg Spine. 2018. PMID: 29087808
-
Multicenter assessment of outcomes and complications associated with transforaminal versus anterior lumbar interbody fusion for fractional curve correction.J Neurosurg Spine. 2021 Aug 20;35(6):729-742. doi: 10.3171/2020.11.SPINE201915. Print 2021 Dec 1. J Neurosurg Spine. 2021. PMID: 34416723
-
Lumbar Lordosis Correction with Interbody Fusion: Systematic Literature Review and Analysis.World Neurosurg. 2018 Oct;118:21-31. doi: 10.1016/j.wneu.2018.06.216. Epub 2018 Jul 4. World Neurosurg. 2018. PMID: 29981462
-
ALIF in the correction of spinal sagittal misalignment. A systematic review of literature.Eur Spine J. 2021 Jan;30(1):50-62. doi: 10.1007/s00586-020-06598-y. Epub 2020 Sep 15. Eur Spine J. 2021. PMID: 32930843
Cited by
-
Treatment of Adult Spinal Deformity with Sagittal Imbalance Using Oblique Lumbar Interbody Fusion: Can We Predict How Much Lordosis Correction Is Possible?Asian Spine J. 2019 Dec;13(6):1017-1027. doi: 10.31616/asj.2018.0306. Epub 2019 Jul 30. Asian Spine J. 2019. PMID: 31352725 Free PMC article.
-
Unplanned Second-Stage Decompression for Neurological Deterioration Caused by Central Canal Stenosis after Indirect Lumbar Decompression Surgery.Asian Spine J. 2019 Mar 15;13(4):584-591. doi: 10.31616/asj.2018.0232. Print 2019 Aug. Asian Spine J. 2019. PMID: 30866617 Free PMC article.
-
Indirect Decompression Using Lateral Lumbar Interbody Fusion for Restenosis after an Initial Decompression Surgery.Asian Spine J. 2020 Jun;14(3):305-311. doi: 10.31616/asj.2019.0194. Epub 2020 Jan 8. Asian Spine J. 2020. PMID: 31906613 Free PMC article.
-
Effectiveness of Short-Segment Fixation versus Long-Segment Fixation for Degenerative Scoliosis with Cobb Angle 20°~40°: A Retrospective Observational Study.Med Sci Monit. 2020 Jul 22;26:e923656. doi: 10.12659/MSM.923656. Med Sci Monit. 2020. PMID: 32694499 Free PMC article.
-
What Are the Benefits of Lateral Lumbar Interbody Fusion on the Treatment of Adult Spinal Deformity: A Systematic Review and Meta-Analysis Deformity.Global Spine J. 2023 Jan;13(1):172-187. doi: 10.1177/21925682221089876. Epub 2022 Apr 20. Global Spine J. 2023. PMID: 35442824 Free PMC article. Review.
References
-
- Sasso RC, Best NM, Mummaneni PV, et al. Analysis of operative complications in a series of 471 anterior lumbar interbody fusion procedures. Spine (Phila Pa 1976) 2005;30:670–4. - PubMed
-
- Crandall DG, Revella J. Transforaminal lumbar interbody fusion versus anterior lumbar interbody fusion as an adjunct to posterior instrumented correction of degenerative lumbar scoliosis: three year clinical and radiographic outcomes. Spine (Phila Pa 1976) 2009;34:2126–33. - PubMed
-
- Hsieh PC, Koski TR, O’Shaughnessy BA, et al. Anterior lumbar interbody fusion in comparison with transforaminal lumbar interbody fusion: implications for the restoration of foraminal height, local disc angle, lumbar lordosis, and sagittal balance. J Neurosurg Spine. 2007;7:379–86. - PubMed
-
- Pavlov PW, Meijers H, van Limbeek J, et al. Good outcome and restoration of lordosis after anterior lumbar interbody fusion with additional posterior fixation. Spine (Phila Pa 1976) 2004;29:1893–9. discussion 900. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

