The impact of concordant and discordant comorbidities on patient-assessed quality of diabetes care
- PMID: 24151930
- PMCID: PMC5060868
- DOI: 10.1111/hex.12151
The impact of concordant and discordant comorbidities on patient-assessed quality of diabetes care
Abstract
Objective: To examine the impact of concordant and discordant comorbidities on patients' assessments of providers' adherence to diabetes-specific care guidelines and quality of chronic illness care.
Research design and methods: A population-based survey of 3761 adults with type 2 diabetes, living in Queensland, Australia was conducted in 2008. Based on self-reports, participants were grouped into four mutually exclusive comorbid categories: none, concordant only, discordant only and both concordant and discordant. Outcome measures included patient-reported providers' adherence to guideline-recommended care and the Patient Assessment of Chronic Illness Care (PACIC), which measures care according to the Chronic Care Model. Analyses using the former measure included logistic regressions, and the latter measure included univariate analysis of variance, both unadjusted and adjusted for sampling region, gender, age, educational attainment, diabetes duration and treatment status.
Results: Having concordant comorbidities increased the odds of patient-reported providers' adherence for 7 of the 11 guideline-recommended care activities in unadjusted analyses. However, the effect remained significant for only two provider activities (reviews of medication and/or complications and blood pressure examinations) when adjusted. A similar pattern was found for the both concordant and discordant comorbidity category. The presence of discordant comorbidities influenced only one provider activity (blood pressure examinations). No association between comorbidity type and the overall PACIC score was found.
Conclusions: Comorbidity type is associated with diabetes-specific care, but does not seem to influence broader aspects of chronic illness care directly. Providers need to place more emphasis on care activities which are not comorbidity-specific and thus transferable across different chronic conditions.
Keywords: chronic illness care; comorbidity; diabetes; guideline adherence; patient perspectives; quality of care.
© 2013 John Wiley & Sons Ltd.
Figures
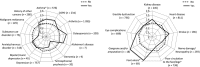
References
-
- Britt HC, Harrison CM, Miller GC, Knox SA. Prevalence and patterns of multimorbidity in Australia. The Medical Journal of Australia, 2008; 189: 72–77. - PubMed
-
- Uijen AA, van dLEH. Multimorbidity in primary care: prevalence and trend over the last 20 years. The European Journal of General Practice, 2008; 14(Suppl 1): 28–32. - PubMed
-
- Barnett K, Mercer SW, Norbury M, Watt G, Wyke S, Guthrie B. Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross‐sectional study. Lancet, 2012; 380: 37–43. - PubMed
-
- Caughey GE, Roughead EE, Vitry AI, McDermott RA, Shakib S, Gilbert AL. Comorbidity in the elderly with diabetes: Identification of areas of potential treatment conflicts. Diabetes Research and Clinical Practice, 2010; 87: 385–393. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

