Acquired pial and dural arteriovenous fistulae following superior sagittal sinus thrombosis in patients with protein S deficiency: a report of two cases
- PMID: 24162240
- PMCID: PMC4533415
- DOI: 10.2176/nmc.cr2012-0311
Acquired pial and dural arteriovenous fistulae following superior sagittal sinus thrombosis in patients with protein S deficiency: a report of two cases
Abstract
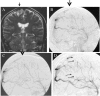
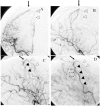
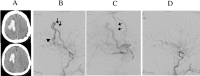
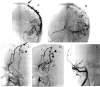
Two patients with protein S deficiency with acquired multiple pial and dural arteriovenous fistulae (AVFs) following superior sagittal sinus (SSS) thrombosis are reported. Case 1 is a 38-year-old male with protein S deficiency who developed generalized seizure due to SSS thrombosis. Local fibrinolysis was achieved in the acute stage. His 10-month follow-up angiogram revealed an asymptomatic acquired dural AVF arising from the middle meningeal artery and the anterior cerebral artery with drainage to the thrombosed cortical vein in the right frontal lobe. Furthermore, his 2-year follow-up angiogram revealed a de novo pial AVF from the middle cerebral artery in the Sylvian fissure with drainage to the cortical vein initially thrombosed. However, this asymptomatic pial AVF caused bleeding in the ipsilateral cerebral hemisphere 12 years after onset, whereas the dural AVF spontaneously disappeared. Surgical disconnection was successfully performed to eliminate the source of hemorrhage. Case 2 is a 50-year-old male with a past history of SSS thrombosis with protein S deficiency who developed pulsatile tinnitus and generalized seizure. His angiogram showed a cortical dural AVF in the left parietal lobe and a sporadic dural AVF involving the right sigmoid sinus. The parietal lesion was eliminated by transarterial embolization followed by craniotomy. However, a de novo pial AVF emerged from the middle cerebral artery adjacent to the previously treated lesion. Of four cortical AVFs in two patients, thrombosis of cortical veins caused by protein S deficiency might play an important role in their formation. Long-term follow-up is required because this peculiar disorder has an unusual clinical course.
Figures




Similar articles
-
Multiple Dural and Pial Arteriovenous Fistulae in a Twenty-Four-Year-Old Woman in the Setting of Superior Sagittal Sinus Thrombosis: Case Report and Review of Literature.J Stroke Cerebrovasc Dis. 2016 Oct;25(10):e192-9. doi: 10.1016/j.jstrokecerebrovasdis.2016.07.037. Epub 2016 Aug 17. J Stroke Cerebrovasc Dis. 2016. PMID: 27544867 Review.
-
Acquired pial arteriovenous fistula secondary to cerebral cortical vein thrombosis: A case report and review of the literature.Neuroradiol J. 2022 Aug;35(4):515-519. doi: 10.1177/19714009211049080. Epub 2021 Oct 5. Neuroradiol J. 2022. PMID: 34609931 Free PMC article. Review.
-
Multiple Cranial Dural and Pial Arteriovenous Fistulas with Occlusion of All After Embolization of Primary Superior Sagittal Sinus Dural Fistula.World Neurosurg. 2020 Aug;140:224-228. doi: 10.1016/j.wneu.2020.05.045. Epub 2020 May 11. World Neurosurg. 2020. PMID: 32437996
-
Dural arteriovenous fistula involving the superior sagittal sinus following sinus thrombosis--case report.Neurol Med Chir (Tokyo). 2002 May;42(5):217-20. doi: 10.2176/nmc.42.217. Neurol Med Chir (Tokyo). 2002. PMID: 12064156
-
Treatment of a superior sagittal sinus dural arteriovenous fistula with Onyx: technical case report.Neurosurgery. 2006 Jul;59(1 Suppl 1):ONSE169-70; discussion ONSE169-70. doi: 10.1227/01.NEU.0000220113.34075.40. Neurosurgery. 2006. PMID: 16888563
Cited by
-
Cerebral venous sinus thrombosis and dural arteriovenous fistula associated with protein S deficiency: a case series study.BMC Neurol. 2022 May 2;22(1):164. doi: 10.1186/s12883-022-02693-3. BMC Neurol. 2022. PMID: 35501720 Free PMC article.
-
Intracranial non-galenic pial arteriovenous fistula: A review of the literature.Interv Neuroradiol. 2016 Oct;22(5):557-68. doi: 10.1177/1591019916653934. Epub 2016 Jul 6. Interv Neuroradiol. 2016. PMID: 27388601 Free PMC article. Review.
-
Transarterial embolization for convexity dural arteriovenous fistula with or without pial arterial supply: A report of four patients.Surg Neurol Int. 2022 Aug 5;13:340. doi: 10.25259/SNI_215_2022. eCollection 2022. Surg Neurol Int. 2022. PMID: 36128114 Free PMC article.
-
Giant cranial angiolipoma with arteriovenous fistula: A case report.Surg Neurol Int. 2022 Jul 22;13:314. doi: 10.25259/SNI_422_2022. eCollection 2022. Surg Neurol Int. 2022. PMID: 35928320 Free PMC article.
-
Anterior Cranial Fossa Dural Arteriovenous Fistula with Pial Arterial Supply.Asian J Neurosurg. 2020 Feb 25;15(1):176-179. doi: 10.4103/ajns.AJNS_288_19. eCollection 2020 Jan-Mar. Asian J Neurosurg. 2020. PMID: 32181197 Free PMC article.
References
-
- Sugiura Y, Miyamoto T, Takehara S, Sumiya K, Nozaki T: [Multiple dural arteriovenous fistulas following extensive sinus thrombosis: a case report]. No Shinkei Geka 24: 379– 383, 1996. (Japanese) - PubMed
-
- Ozawa T, Miyasaka Y, Tanaka R, Kurata A, Fujii K: Dural-pial arteriovenous malformation after sinus thrombosis. Stroke 29: 1721– 1724, 1998. - PubMed
-
- Nishio A, Ohata K, Tsuchida K, Tsuyuguchi N, Hara M, Komiyama M, Tsuruno T, Murata T: Dural arteriovenous fistula involving the superior sagittal sinus following sinus thrombosis—case report. Neurol Med Chir (Tokyo) 42: 217– 220, 2002. - PubMed
-
- Toledo MM, Wilson TJ, Dashti S, McDougall CG, Spetzler RF: Dural arteriovenous fistula associated with superior sagittal sinus occlusion secondary to invasion by a parafalcine meningioma: case report. Neurosurgery 67: 205– 207; discussion 207, 2010. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

