Purtscher's retinopathy followed by neovascular glaucoma
- PMID: 24255591
- PMCID: PMC3832461
- DOI: 10.2147/OPTH.S54231
Purtscher's retinopathy followed by neovascular glaucoma
Abstract
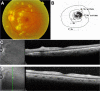
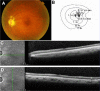
We report the case of a 66-year-old Japanese man who developed neovascular glaucoma secondary to Purtscher's retinopathy following a head injury. The patient presented at our hospital with blurred vision and a visual field abnormality in his left eye 1 month after suffering from a head injury. Upon initial presentation, his best-corrected visual acuity on a decimal chart was 1.5 oculus dexter and 0.6 oculus sinister. The intraocular pressure (IOP) was 12 mmHg in both eyes. Fundus examination of the left eye revealed multiple white lesions in the posterior pole. Optical coherence tomography demonstrated retinal edema, particularly in the inner retina. On the basis of these findings, a diagnosis of Purtscher's retinopathy was made. One month after the initial examination, the visual acuity in the left eye deteriorated to 0.01 in decimal chart, and the IOP increased to 37 mmHg. Gonioscopy showed angle neovascularization. The patient received an intravitreal bevacizumab injection and panretinal photocoagulation. Subsequently, the IOP normalized and the angle neovascularization regressed.
Keywords: blurred vision; head injury; head trauma; retinal edema; visual field.
Figures

References
-
- Purtscher O. Noch unbekannte befunde nach schadeltrauma. [Unknown findings after head trauma.] Ber Dtsch Ophthalmol Ges. 1910;36:294–301. German.
-
- Agrawal A, McKibbin MA. Purtscher’s and Purtscher-like retinopathies: a review. Surv Ophthalmol. 2006;51(2):129–136. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

