The effects of exogenous surfactant administration on ventilation-induced inflammation in mouse models of lung injury
- PMID: 24256698
- PMCID: PMC4222563
- DOI: 10.1186/1471-2466-13-67
The effects of exogenous surfactant administration on ventilation-induced inflammation in mouse models of lung injury
Abstract
Background: Mechanical ventilation (MV) is an essential supportive therapy for acute lung injury (ALI); however it can also contribute to systemic inflammation. Since pulmonary surfactant has anti-inflammatory properties, the aim of the study was to investigate the effect of exogenous surfactant administration on ventilation-induced systemic inflammation.
Methods: Mice were randomized to receive an intra-tracheal instillation of a natural exogenous surfactant preparation (bLES, 50 mg/kg) or no treatment as a control. MV was then performed using the isolated and perfused mouse lung (IPML) set up. This model allowed for lung perfusion during MV. In experiment 1, mice were exposed to mechanical ventilation only (tidal volume =20 mL/kg, 2 hours). In experiment 2, hydrochloric acid or air was instilled intra-tracheally four hours before applying exogenous surfactant and ventilation (tidal volume =5 mL/kg, 2 hours).
Results: For both experiments, exogenous surfactant administration led to increased total and functional surfactant in the treated groups compared to the controls. Exogenous surfactant administration in mice exposed to MV only did not affect peak inspiratory pressure (PIP), lung IL-6 levels and the development of perfusate inflammation compared to non-treated controls. Acid injured mice exposed to conventional MV showed elevated PIP, lung IL-6 and protein levels and greater perfusate inflammation compared to air instilled controls. Instillation of exogenous surfactant did not influence the development of lung injury. Moreover, exogenous surfactant was not effective in reducing the concentration of inflammatory cytokines in the perfusate.
Conclusions: The data indicates that exogenous surfactant did not mitigate ventilation-induced systemic inflammation in our models. Future studies will focus on altering surfactant composition to improve its immuno-modulating activity.
Figures


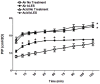


Similar articles
-
Elevated endogenous surfactant reduces inflammation in an acute lung injury model.Exp Lung Res. 2009 Sep;35(7):591-604. doi: 10.1080/01902140902780460. Exp Lung Res. 2009. PMID: 19842847
-
Characterization of inflammation in a rat model of acute lung injury after repeated pulmonary lavage.Exp Lung Res. 2015;41(8):466-76. doi: 10.3109/01902148.2015.1075079. Exp Lung Res. 2015. PMID: 26381719
-
The effects of exogenous surfactant treatment in a murine model of two-hit lung injury.Anesth Analg. 2015 Feb;120(2):381-8. doi: 10.1213/ANE.0000000000000549. Anesth Analg. 2015. PMID: 25502842
-
The exogenous surfactant pre-treatment attenuates ventilator-induced lung injury in adult rats.Respir Physiol Neurobiol. 2022 Aug;302:103911. doi: 10.1016/j.resp.2022.103911. Epub 2022 Apr 14. Respir Physiol Neurobiol. 2022. PMID: 35430285
-
Nanoparticle-mediated surfactant therapy in patients with severe COVID-19: a perspective.J Mater Chem B. 2021 Sep 15;9(35):6988-6993. doi: 10.1039/d1tb00730k. J Mater Chem B. 2021. PMID: 34085075 Review.
Cited by
-
Seawater-drowning-induced acute lung injury: From molecular mechanisms to potential treatments.Exp Ther Med. 2017 Jun;13(6):2591-2598. doi: 10.3892/etm.2017.4302. Epub 2017 Apr 5. Exp Ther Med. 2017. PMID: 28587319 Free PMC article.
-
Exogenous surfactant reduces inflammation and redox imbalance in rats under prone or supine mechanical ventilation.Exp Biol Med (Maywood). 2023 Jun;248(12):1074-1084. doi: 10.1177/15353702231160352. Epub 2023 Apr 24. Exp Biol Med (Maywood). 2023. PMID: 37092748 Free PMC article.
-
Nonionic surfactant attenuates acute lung injury by restoring epithelial integrity and alveolar fluid clearance.Int J Med Sci. 2021 Jan 21;18(6):1363-1374. doi: 10.7150/ijms.51905. eCollection 2021. Int J Med Sci. 2021. PMID: 33628092 Free PMC article.
-
Surfactant Attenuates Air Embolism-Induced Lung Injury by Suppressing NKCC1 Expression and NF-κB Activation.Inflammation. 2021 Feb;44(1):57-67. doi: 10.1007/s10753-020-01266-1. Inflammation. 2021. PMID: 33089374 Free PMC article.
-
Hyperoxia treatment of TREK-1/TREK-2/TRAAK-deficient mice is associated with a reduction in surfactant proteins.Am J Physiol Lung Cell Mol Physiol. 2017 Dec 1;313(6):L1030-L1046. doi: 10.1152/ajplung.00121.2017. Epub 2017 Aug 24. Am J Physiol Lung Cell Mol Physiol. 2017. PMID: 28839101 Free PMC article.
References
-
- Goerke J. Pulmonary surfactant: functions and molecular composition. Biochim Biophys Acta. 1998;1408(2–3):79–89. - PubMed
-
- Wright JR. Immunomodulatory functions of surfactant. Physiol Rev. 1997;77(4):931–962. - PubMed
-
- Veldhuizen RA, McCaig LA, Akino T, Lewis JF. Pulmonary surfactant subfractions in patients with the acute respiratory distress syndrome. Am J Respir Crit Care Med. 1995;152(6 Pt 1):1867–1871. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

