Immune quiescence: a model of protection against HIV infection
- PMID: 24257114
- PMCID: PMC3874678
- DOI: 10.1186/1742-4690-10-141
Immune quiescence: a model of protection against HIV infection
Abstract
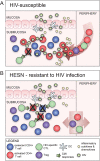
Aberrant immune activation is a strong correlate of HIV disease progression, but little is known about how immune activation alters susceptibility to HIV infection. Susceptibility to HIV infection varies between individuals, but the immunological determinants of HIV transmission are not well understood. Here, we present evidence from studies of HIV transmission in the context of clinical trials and HIV-exposed seronegative (HESN) cohorts that implicates elevated immune activation as a risk factor for acquiring HIV. We propose a model of protection from infection based on a phenotype of low baseline immune activation referred to as immune quiescence. Immune quiescence is evidenced by reduced expression of T cell activation markers, low levels of generalized gene transcription and low levels of proinflammatory cytokine and chemokine production in the periphery and genital mucosa of HESN. Since HIV preferentially replicates in activated CD4+ T cells, immune quiescence may protect against infection by limiting HIV target cell availability. Although the determinants of immune quiescence are unclear, several potential factors have been identified that may be involved in driving this phenotype. HESN were shown to have elevated proportions of regulatory T cells (Tregs), which are known to suppress T cell activation. Likewise, proteins involved in controlling inflammation in the genital tract have been found to be elevated in HESN. Furthermore, expression of interferon regulatory factor 1 (IRF-1) is reduced in HESN as a consequence of genetic polymorphisms and differential epigenetic regulation. Since IRF-1 is an important regulator of immune responses, it may play a role in maintaining immune quiescence. Based on this model, we propose a novel avenue for HIV prevention targeted based on reducing host mucosal immune activation.
Figures
Similar articles
-
Genetic and immune determinants of immune activation in HIV-exposed seronegative individuals and their role in protection against HIV infection.Infect Genet Evol. 2018 Dec;66:325-334. doi: 10.1016/j.meegid.2017.12.014. Epub 2017 Dec 16. Infect Genet Evol. 2018. PMID: 29258786
-
Deciphering the Role of Mucosal Immune Responses and the Cervicovaginal Microbiome in Resistance to HIV Infection in HIV-Exposed Seronegative (HESN) Women.Microbiol Spectr. 2021 Oct 31;9(2):e0047021. doi: 10.1128/Spectrum.00470-21. Epub 2021 Oct 27. Microbiol Spectr. 2021. PMID: 34704803 Free PMC article.
-
Highly Human Immunodeficiency Virus-Exposed Seronegative Men Have Lower Mucosal Innate Immune Reactivity.AIDS Res Hum Retroviruses. 2017 Aug;33(8):788-795. doi: 10.1089/AID.2017.0014. Epub 2017 Jun 19. AIDS Res Hum Retroviruses. 2017. PMID: 28503933 Free PMC article.
-
Evidence for the innate immune response as a correlate of protection in human immunodeficiency virus (HIV)-1 highly exposed seronegative subjects (HESN).Clin Exp Immunol. 2011 May;164(2):158-69. doi: 10.1111/j.1365-2249.2011.04379.x. Epub 2011 Mar 17. Clin Exp Immunol. 2011. PMID: 21413945 Free PMC article. Review.
-
Preventing HIV infection without targeting the virus: how reducing HIV target cells at the genital tract is a new approach to HIV prevention.AIDS Res Ther. 2017 Sep 12;14(1):46. doi: 10.1186/s12981-017-0166-7. AIDS Res Ther. 2017. PMID: 28893304 Free PMC article. Review.
Cited by
-
Segmented intravaginal ring for the combination delivery of hydroxychloroquine and anti-CCR5 siRNA nanoparticles as a potential strategy for preventing HIV infection.Drug Deliv Transl Res. 2022 Apr;12(4):816-825. doi: 10.1007/s13346-021-00983-w. Epub 2021 Apr 17. Drug Deliv Transl Res. 2022. PMID: 33866528 Free PMC article.
-
Upregulation of PTPRC and Interferon Response Pathways in HIV-1 Seroconverters Prior to Infection.J Infect Dis. 2023 Mar 1;227(5):714-719. doi: 10.1093/infdis/jiac498. J Infect Dis. 2023. PMID: 36637125 Free PMC article.
-
LncIRF1 promotes chicken resistance to ALV-J infection.3 Biotech. 2023 Nov;13(11):367. doi: 10.1007/s13205-023-03773-y. Epub 2023 Oct 14. 3 Biotech. 2023. PMID: 37846216 Free PMC article.
-
Are violence, harmful alcohol/substance use and poor mental health associated with increased genital inflammation?: A longitudinal cohort study with HIV-negative female sex workers in Nairobi, Kenya.PLOS Glob Public Health. 2024 Aug 27;4(8):e0003592. doi: 10.1371/journal.pgph.0003592. eCollection 2024. PLOS Glob Public Health. 2024. PMID: 39190654 Free PMC article.
-
Improving Adherence to Post-Cervical Biopsy Sexual Abstinence in Kenyan Female Sex Workers.Am J Reprod Immunol. 2016 Jul;76(1):82-93. doi: 10.1111/aji.12520. Epub 2016 May 24. Am J Reprod Immunol. 2016. PMID: 27221472 Free PMC article. Clinical Trial.
References
-
- Zhang Z-Q, Wietgrefe SW, Li Q, Shore MD, Duan L, Reilly C, Lifson JD, Haase AT. Roles of substrate availability and infection of resting and activated CD4+ T cells in transmission and acute simian immunodeficiency virus infection. Proc Natl Acad Sci U S A. 2004;101:5640–5645. doi: 10.1073/pnas.0308425101. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

