A review of 11 years of Stenotrophomonas maltophilia blood isolates at a tertiary care institute in Canada
- PMID: 24294268
- PMCID: PMC3597391
- DOI: 10.1155/2012/762571
A review of 11 years of Stenotrophomonas maltophilia blood isolates at a tertiary care institute in Canada
Abstract
Background: Stenotrophomonas maltophilia has emerged as a significant nosocomial pathogen with increasing resistance to trimethoprim/sulphamethoxazole (TMP/SMX), the current drug of choice for treatment.
Objectives: To describe the microbiological and clinical characteristics of S maltophilia bloodstream infections (BSIs) over an 11-year period at a tertiary care centre in Canada.
Methods: All adult S maltophilia BSIs from 1999 to 2009 in a 750-bed tertiary care teaching hospital (University of Alberta Hospital, Edmonton, Alberta) were identified through the infection control nosocomial infection surveillance program. Demographic and clinical data were extracted from the infection control database and from patient charts. Microbiological data were confirmed through the laboratory information system.
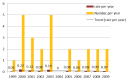
Results: Twenty-five episodes of S maltophilia BSI (0.9% of all BSIs) involving 24 patients were identified between 1999 and 2009. The patient age range was 18 to 83 years (average 45.7 years). The majority were men (14 of 24 [58.3%]). The mean length of hospital stay was 83.3 days (range eight to 310 days). The rate of S maltophilia BSIs per 1000 admissions ranged from 0.04 to 0.22 (average 0.09). Greater than one-half of the episodes (13 of 25 [52%]) were admitted to the intensive care unit before BSI onset. Laboratory data were available for 24 of the 25 isolates. Polymicrobial infections were present in 11 of 24 (45.8%) patients. Resistance to TMP/SMX occurred in 8.3% of all infections. Fifteen per cent of isolates were resistant to ticarcillin/clavulanate. Mortality attributed to bacteremia was 16.7%.
Conclusions: In the University of Alberta Hospital, the rate of S maltophilia BSI remains low and constant, and TMP/SMX remains the drug of choice for treatment.
Historique: Le Stenotrophomonas maltophilia a émergé comme un pathogène nosocomial important de plus en plus résistant au triméthoprim-sulphaméthoxazole (TMP-SMX), le traitement de choix actuel.
Objectifs: Décrire les caractéristiques microbiologiques et cliniques des infections du sang (IS) à S maltophilia sur une période de onze ans dans un centre de soins tertiaires du Canada.
Méthodologie: Les chercheurs ont retenu tous les adultes ayant contracté une IS à S maltophilia entre 1999 et 2009 dans un hôpital d’enseignement de soins tertiaires de 750 lits (University of Alberta Hospital, Edmonton, Alberta) par le programme de surveillance des infections nosocomiales du Contrôle des infections. Ils ont tiré les données démographiques et cliniques des bases de données du Contrôle des infections et des dossiers des patients. Ils ont confirmé les données microbiologiques par le système d’information en laboratoire.
Résultats: Les chercheurs ont constaté 25 épisodes d’IS à S maltophilia (0,9 % de toutes les IS), touchant 24 patients entre 1999 et 2009. Les patients avaient de 18 à 83 ans (moyenne de 45,7 ans), étaient majoritairement de sexe masculin (14 sur 24 [58,3 %]) et ils avaient été hospitalisés pendant une durée moyenne de 83,3 jours (plage de huit à 310 jours). Le taux d’IS à S maltophilia sur 1 000 hospitalisations oscillait entre 0,04 et 0,22 (moyenne 0,09). Plus de la moitié des épisodes (13 sur 25 [52 %]) s’étaient produits chez des patients hospitalisés à l’unité de soins intensifs avant l’apparition de l’IS. Les chercheurs possédaient les données de laboratoire de 24 des 25 isolats et ont relevé des infections polymicrobiennes chez 11 des 24 patients (45,8 %). Ils ont observé une résistance au TMP-SMX dans 8,3 % de toutes les infections. Quinze pour cent des isolats étaient résistants à la ticarcilline-clavulanate. La mortalité attribuée à la bactériémie s’élevait à 16,7 %.
Conclusions: À l’University of Alberta Hospital, le taux d’IS à S maltophilia demeure faible et constant, et le TMP-SMX demeure le médicament de choix pour traiter cette infection.
Keywords: Bloodstream infections; Catheter-related infections; Stenotrophomonas.
Figures
Similar articles
-
Epidemiological Trends and Resistance Associated with Stenotrophomonas maltophilia Bacteremia: A 10-Year Retrospective Cohort Study in a Tertiary-Care Hospital in Hungary.Diseases. 2019 May 31;7(2):41. doi: 10.3390/diseases7020041. Diseases. 2019. PMID: 31159258 Free PMC article.
-
The Burden of Bloodstream Infections due to Stenotrophomonas Maltophilia in the United States: A Large, Retrospective Database Study.Open Forum Infect Dis. 2020 Apr 22;7(5):ofaa141. doi: 10.1093/ofid/ofaa141. eCollection 2020 May. Open Forum Infect Dis. 2020. PMID: 32462047 Free PMC article.
-
Stenotrophomonas maltophilia bloodstream infection in patients with hematologic malignancies: a retrospective study and in vitro activities of antimicrobial combinations.BMC Infect Dis. 2015 Feb 18;15:69. doi: 10.1186/s12879-015-0801-7. BMC Infect Dis. 2015. PMID: 25887489 Free PMC article.
-
Stenotrophomonas (Xanthomonas) maltophilia: a multidrug-resistant nosocomial pathogen.Pharmacotherapy. 1997 Mar-Apr;17(2):293-301. Pharmacotherapy. 1997. PMID: 9085321 Review.
-
Update on infections caused by Stenotrophomonas maltophilia with particular attention to resistance mechanisms and therapeutic options.Front Microbiol. 2015 Sep 2;6:893. doi: 10.3389/fmicb.2015.00893. eCollection 2015. Front Microbiol. 2015. PMID: 26388847 Free PMC article. Review.
Cited by
-
Infections Caused by Stenotrophomonas maltophilia in Recipients of Hematopoietic Stem Cell Transplantation.Front Oncol. 2014 Aug 25;4:232. doi: 10.3389/fonc.2014.00232. eCollection 2014. Front Oncol. 2014. PMID: 25202682 Free PMC article. Review.
-
Stenotrophomonas maltophilia bacteremia and pneumonia at a tertiary-care oncology center: a review of 16 years.Support Care Cancer. 2018 Jun;26(6):1953-1960. doi: 10.1007/s00520-017-4032-x. Epub 2018 Jan 7. Support Care Cancer. 2018. PMID: 29307014
-
Molecular Epidemiology of Stenotrophomonas maltophilia Strains Isolated from Bacteremia in Hospitalized Children.Oman Med J. 2023 May 31;38(3):e505. doi: 10.5001/omj.2023.76. eCollection 2023 May. Oman Med J. 2023. PMID: 37346891 Free PMC article.
-
Characterization of Novel Broad-Host-Range Bacteriophage DLP3 Specific to Stenotrophomonas maltophilia as a Potential Therapeutic Agent.Front Microbiol. 2020 Jun 24;11:1358. doi: 10.3389/fmicb.2020.01358. eCollection 2020. Front Microbiol. 2020. PMID: 32670234 Free PMC article.
-
Clinical characteristics and prognostic factors of patients with Stenotrophomonas maltophilia infections.J Lab Physicians. 2017 Apr-Jun;9(2):132-135. doi: 10.4103/0974-2727.199639. J Lab Physicians. 2017. PMID: 28367030 Free PMC article.
References
-
- Spencer RC. The emergence of epidemic, multiple-antibiotic-resistant Stenotrophomonas maltophilia and Burkholderia cepacia. J Hosp Infect. 1995;30:453–64. - PubMed
-
- Barchitta M, Cipresso R, Giaquinta L, et al. Acquisition and spread of Acinetobacter baumannii and Stenotrophomonas maltophilia in intensive care patients. Int J Hyg Environ Health. 2009;212:330–7. - PubMed
-
- Nyc O, Matejkova J. Stenotrophomonas maltophilia: Significant contemporary hospital pathogen – review. Folia Microbiol. 2010;55:286–94. - PubMed
-
- Centers for Disease Prevention and Control National Hospital Surveillance Network website < www.cdc.gov/nhsn/> (Accessed November 30, 2010).
-
- Looney WJ, Narita M, Muhlemann K. Stenotrophomonas maltophilia: An emerging opportunist human pathogen. Lancet Infect Dis. 2009;9:312–23. - PubMed
LinkOut - more resources
Full Text Sources