Predictors and outcomes of resistant hypertension among patients with coronary artery disease and hypertension
- PMID: 24299915
- PMCID: PMC4118668
- DOI: 10.1097/HJH.0000000000000051
Predictors and outcomes of resistant hypertension among patients with coronary artery disease and hypertension
Abstract
Objective: Resistant hypertension (res-HTN) is a challenging problem, but little is known of res-HTN in patients with coronary artery disease (CAD). In this post-hoc INternational VErapamil SR-Trandolapril STudy (INVEST) analysis, we assessed prevalence, predictors, and impact on outcomes of res-HTN in CAD patients with hypertension.
Methods: Participants (n=17190) were divided into three groups according to achieved blood pressure (BP): controlled (BP <140/90 mmHg on three or fewer drugs); uncontrolled (BP ≥ 40/90 mmHg on two or fewer drugs); or resistant (BP ≥ 40/90 mmHg on three drugs or any patient on at least four drugs).
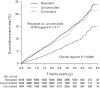
Results: The prevalence of res-HTN was 38%: significant predictors of res-HTN included heart failure [odds ratio (OR) 1.73], diabetes (OR 1.63), Black race (OR 1.50), and US residence (OR 1.50). Compared with controlled HTN, res-HTN had multivariate-adjusted association with higher risk of adverse outcomes {first occurrence of all-cause death, nonfatal myocardial infarction, or nonfatal stroke [hazard ratio 1.27, 95% confidence interval (CI) 1.13-1.43], and individual outcomes of all-cause death (hazard ratio 1.29, 95% CI 1.13-1.48), cardiovascular mortality (hazard ratio 1.47, 95% CI 1.21-1.78), and nonfatal stroke (hazard ratio 1.61, 95% CI 1.17-2.22), but not nonfatal myocardial infarction (hazard ratio 0.98, 95% CI 0.72-1.34)}. Adverse outcomes, except nonfatal stroke, did not differ in patients with res-HTN compared to uncontrolled HTN.
Conclusions: Res-HTN is common in patients with CAD and hypertension, associated with poor prognosis, and linked with a number of conditions. Emphasis should be placed on recognizing those at risk for res-HTN and future studies should examine whether more aggressive treatment of res-HTN improves outcomes.
Conflict of interest statement
Figures






Comment in
-
Resistant hypertension revisited: definition and true prevalence.J Hypertens. 2014 Jul;32(7):1546. doi: 10.1097/HJH.0000000000000219. J Hypertens. 2014. PMID: 24918497 No abstract available.
-
Reply to 'Resistant hypertension revisited: definition and true prevalence'.J Hypertens. 2014 Jul;32(7):1547. doi: 10.1097/HJH.0000000000000220. J Hypertens. 2014. PMID: 24984184 No abstract available.
References
-
- Calhoun DA, Jones D, Textor S, Goff DC, Murphy TP, Toto RD, et al. Resistant hypertension: diagnosis, evaluation, and treatment. A scientific statement from the American Heart Association Professional Education Committee of the Council for High Blood Pressure Research. Hypertension. 2008;51:1403–1419. - PubMed
-
- Cushman WC, Ford CE, Cutler JA, Margolis KL, Davis BR, Grimm RH, et al. Success and predictors of blood pressure control in diverse north american settings: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT) J Clin Hypertens (Greenwich) 2002;4:393–404. - PubMed
-
- Gupta AK, Nasothimiou EG, Chang CL, Sever PS, Dahlöf B, Poulter NR ASCOT Investigators. Baseline predictors of resistant hypertension in the Anglo-Scandinavian Cardiac Outcome Trial (ASCOT): a risk score to identify those at high-risk. J Hypertens. 2011;29:2004–2013. - PubMed
-
- Smith SM. Epidemiology, prognosis, and treatment of resistant hypertension. Pharmacotherapy. 2013;33:1071–1086. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

