Effects of fluid resuscitation with 0.9% saline versus a balanced electrolyte solution on acute kidney injury in a rat model of sepsis*
- PMID: 24335444
- PMCID: PMC4143135
- DOI: 10.1097/CCM.0000000000000145
Effects of fluid resuscitation with 0.9% saline versus a balanced electrolyte solution on acute kidney injury in a rat model of sepsis*
Abstract
Objective: To compare the acute effects of 0.9% saline versus a balanced electrolyte solution on acute kidney injury in a rat model of sepsis.
Design: Controlled laboratory experiment.
Setting: University laboratory.
Subjects: Sixty adult, male Sprague-Dawley rats.
Interventions: We induced sepsis by cecal ligation and puncture and randomized animals to receive fluid resuscitation with either 0.9% saline or Plasma-Lyte solution for 4 hours after 18 hours of cecal ligation and puncture (10 mL/kg in the first hour and 5 mL/kg in the next 3 hr). Blood and urine specimens were obtained from baseline, 18 hours after cecal ligation and puncture, immediately after 4 hours fluid resuscitation, and 24 hours later. We measured blood gas, plasma electrolytes, creatinine, interleukin-6, cystatin C, and neutrophil gelatinase-associated lipocalin concentrations. We also analyzed urine for cystatin C and neutrophil gelatinase-associated lipocalin. We used Risk, Injury, Failure, Loss and End-stage criteria for creatinine to assess severity of acute kidney injury. We observed all animals for survival up to 1 day after resuscitation. Surviving animals were killed for kidney histology. Finally, we carried out an identical study in 12 healthy animals.
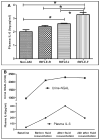
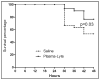
Measurements and main results: Compared with Plasma-Lyte, 0.9% saline resuscitation resulted in significantly greater blood chloride concentrations (p < 0.05) and significantly decreased pH and base excess. Acute kidney injury severity measured by RIFLE criteria was increased with 0.9% saline compared with Plasma-Lyte resuscitation (p < 0.05), and these results were consistent with kidney histology and biomarkers of acute kidney injury. Twenty-four-hour survival favored Plasma-Lyte resuscitation (76.6% vs 53.3%; p = 0.03). Finally, in healthy animals, we found no differences between fluids and no evidence of acute kidney injury.
Conclusion: Volume resuscitation with Plasma-Lyte resulted in less acidosis and less kidney injury and improved short-term survival when compared with 0.9% saline in this experimental animal model of sepsis.
Conflict of interest statement
The remaining authors have disclosed that they do not have any potential conflicts of interest.
Figures





Comment in
-
Building the case toward a definitive clinical trial: saline versus Plasma-Lyte*.Crit Care Med. 2014 Apr;42(4):1009-10. doi: 10.1097/CCM.0000000000000194. Crit Care Med. 2014. PMID: 24633112 No abstract available.
References
-
- Awad S, Allison SP, Lobo DN. The history of 0. 9% saline. Clin Nutr. 2008;27:179–188. - PubMed
-
- Scheingraber S, Rehm M, Sehmisch C, et al. Rapid saline infusion produces hyperchloremic acidosis in patients undergoing gynecologic surgery. Anesthesiology. 1999;90:1265–1270. - PubMed
-
- Hansen PB, Jensen BL, Skott O. Chloride regulates afferent arteriolar contraction in response to depolarization. Hypertension. 1998;32:1066–1070. - PubMed
-
- Imig JD, Passmore JC, Anderson GL, et al. Chloride alters renal blood flow autoregulation in deoxycorticosterone-treated rats. J Lab Clin Med. 1993;121:608–613. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

