Replacing clinic-based tests with home-use tests may increase HIV prevalence among Seattle men who have sex with men: evidence from a mathematical model
- PMID: 24335742
- PMCID: PMC3955208
- DOI: 10.1097/OLQ.0000000000000046
Replacing clinic-based tests with home-use tests may increase HIV prevalence among Seattle men who have sex with men: evidence from a mathematical model
Abstract
Background: Home-use tests have potential to increase HIV testing but may increase the rate of false-negative tests and decrease linkage to HIV care. We sought to estimate the impact of replacing clinic-based testing with home-use tests on HIV prevalence among men who have sex with men (MSM) in Seattle, Washington.
Methods: We adapted a deterministic, continuous-time model of HIV transmission dynamics parameterized using a 2003 random digit dial study of Seattle MSM. Test performance was based on the OraQuick In-Home HIV Test (OraSure Technologies, Inc, Bethlehem, PA) for home-use tests and, on an average, of antigen-antibody combination assays and nucleic acid amplification tests for clinic-based testing.
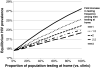
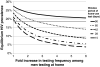
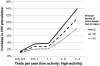
Results: Based on observed levels of clinic-based testing, our baseline model predicted an equilibrium HIV prevalence of 18.6%. If all men replaced clinic-based testing with home-use tests, prevalence increased to 27.5% if home-use testing did not impact testing frequency and to 22.4% if home-use testing increased testing frequency 3-fold. Regardless of how much home-use testing increased testing frequency, any replacement of clinic-based testing with home-use testing increased prevalence. These increases in HIV prevalence were mostly caused by the relatively long window period of the currently approved test. If the window period of a home-use test were 2 months instead of 3 months, prevalence would decrease if all MSM replaced clinic-based testing with home-use tests and tested more than 2.6 times more frequently.
Conclusions: Our model suggests that if home-use HIV tests replace supplement clinic-based testing, HIV prevalence may increase among Seattle MSM, even if home-use tests result in increased testing.
Conflict of interest statement
Conflicts of interest: The authors have no conflicts of interest to declare.
Figures

Comment in
-
Response to the modeling analysis by Katz et al. on the impact of replacing clinic-based HIV tests with home testing among men who have sex with men in Seattle.Sex Transm Dis. 2014 May;41(5):319. doi: 10.1097/OLQ.0000000000000127. Sex Transm Dis. 2014. PMID: 24722386 No abstract available.
-
Response to the modeling analysis by Katz et al. on the impact of replacing clinic-based HIV tests with home testing among men who have sex with men in Seattle: authors' reply.Sex Transm Dis. 2014 May;41(5):320. doi: 10.1097/OLQ.0000000000000131. Sex Transm Dis. 2014. PMID: 24722387 Free PMC article. No abstract available.
-
Translation of "at-home" HIV testing: response to Katz et al. and Hurt and Powers.Sex Transm Dis. 2014 Jul;41(7):454. doi: 10.1097/OLQ.0000000000000140. Sex Transm Dis. 2014. PMID: 24922106 No abstract available.
Similar articles
-
Response to the modeling analysis by Katz et al. on the impact of replacing clinic-based HIV tests with home testing among men who have sex with men in Seattle: authors' reply.Sex Transm Dis. 2014 May;41(5):320. doi: 10.1097/OLQ.0000000000000131. Sex Transm Dis. 2014. PMID: 24722387 Free PMC article. No abstract available.
-
Response to the modeling analysis by Katz et al. on the impact of replacing clinic-based HIV tests with home testing among men who have sex with men in Seattle.Sex Transm Dis. 2014 May;41(5):319. doi: 10.1097/OLQ.0000000000000127. Sex Transm Dis. 2014. PMID: 24722386 No abstract available.
-
HIV serosorting as a harm reduction strategy: evidence from Seattle, Washington.AIDS. 2009 Nov 27;23(18):2497-506. doi: 10.1097/QAD.0b013e328330ed8a. AIDS. 2009. PMID: 19834319 Free PMC article.
-
Translation of "at-home" HIV testing: response to Katz et al. and Hurt and Powers.Sex Transm Dis. 2014 Jul;41(7):454. doi: 10.1097/OLQ.0000000000000140. Sex Transm Dis. 2014. PMID: 24922106 No abstract available.
-
HIV Self-Testing: a Review of Current Implementation and Fidelity.Curr HIV/AIDS Rep. 2016 Apr;13(2):107-15. doi: 10.1007/s11904-016-0307-y. Curr HIV/AIDS Rep. 2016. PMID: 26879653 Review.
Cited by
-
A Pilot, Randomized Controlled Trial of HIV Self-Testing and Real-Time Post-Test Counseling/Referral on Screening and Preventative Care Among Men Who Have Sex with Men.AIDS Patient Care STDS. 2018 Sep;32(9):360-367. doi: 10.1089/apc.2018.0049. AIDS Patient Care STDS. 2018. PMID: 30179528 Free PMC article. Clinical Trial.
-
Factors associated with acceptability of HIV self-testing (HIVST) among university students in a Peri-Urban area of the Democratic Republic of Congo (DRC).Pan Afr Med J. 2018 Dec 27;31:248. doi: 10.11604/pamj.2018.31.248.13855. eCollection 2018. Pan Afr Med J. 2018. PMID: 31452830 Free PMC article.
-
Economic and epidemiological impact of early antiretroviral therapy initiation in India.J Int AIDS Soc. 2015 Oct 1;18(1):20217. doi: 10.7448/IAS.18.1.20217. eCollection 2015. J Int AIDS Soc. 2015. PMID: 26434780 Free PMC article.
-
Effect of Internet-Distributed HIV Self-tests on HIV Diagnosis and Behavioral Outcomes in Men Who Have Sex With Men: A Randomized Clinical Trial.JAMA Intern Med. 2020 Jan 1;180(1):117-125. doi: 10.1001/jamainternmed.2019.5222. JAMA Intern Med. 2020. PMID: 31738378 Free PMC article. Clinical Trial.
-
Evidence and implication of interventions across various socioecological levels to address HIV testing uptake among men who have sex with men in the United States: A systematic review.SAGE Open Med. 2022 Jun 29;10:20503121221107126. doi: 10.1177/20503121221107126. eCollection 2022. SAGE Open Med. 2022. PMID: 35795867 Free PMC article. Review.
References
-
- Spielberg F, Levine RO, Weaver M. Self-testing for HIV: A new option for HIV prevention? Lancet Infect Dis. 2004;4:640–646. - PubMed
-
- Safety and effectiveness of the proposed OraQuick® In-Home HIV Test; U.S. Food and Drug Administration Blood Products Advisory Committee: 102nd Meeting; Gaithersburg, MD. 2012.
-
- Proposed studies to support the approval of over-the-counter (OTC) home use HIV test kits; U.S. Food and Drug Administration Blood Products Advisory Committee: 86th Meeting; Gaithersburg, MD. 2006.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

