Transrectal ultrasound-guided aspiration in the management of prostatic abscess: A single-center experience
- PMID: 24347857
- PMCID: PMC3843335
- DOI: 10.4103/0971-3026.120262
Transrectal ultrasound-guided aspiration in the management of prostatic abscess: A single-center experience
Abstract
Objectives: The safety and efficacy of transrectal ultrasound (TRUS) guided aspiration of prostatic abscess (PA) is known. The objective of this study is to describe a treatment algorithm for management of PA with TRUS-guided aspiration, emphasizing on indications and factors predicting the treatment outcome.
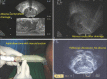
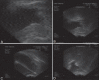
Materials and methods: After the institutional review board approval was obtained, a retrospective study was done of all patients suspected with PA on digital rectal examination (DRE) and confirmed on TRUS. An 18-gauge two-part needle was used for aspiration. The real-time TRUS-guided aspiration of PA was done in the longitudinal axis. The aspiration of pus and the sequential collapse of cavity was seen "real time." A suprapubic catheter was placed, if the patient had urinary retention, persistent dysuria, and/or severe lower urinary tract symptoms (LUTS). Success was defined as complete resolution of the abscess and/or symptoms.
Results: Forty-eight patients were studied with PA, with a mean age of 54.6 ± 14.6 (range 26-79) years. The DRE diagnosed PA in 22 (45.83%) patients, while abdominal sonography diagnosed PA in 13 (27.08%) patients. TRUS revealed a hypoechoic area with internal echoes in all 48 (100%) patients. The diagnosis was confirmed in all 48 cases with aspiration. The mean size of the lesion was 3.2 ± 1.2 (range 1.5-8) cm. Mean volume aspirated was 10.2 ml (range 2.5-30 ml). Complete resolution after first aspiration was observed in 20 (41.66%) patients. An average of 4.1 (range 1-7) aspirations was required for complete resolution which was seen in 41 patients (85.42%). Seven (14.58%) patients required transurethral resection (deroofing) of the abscess cavity. We formulated a treatment algorithm based on the above findings.
Conclusion: The proposed algorithm based on our experience suggests that patients with PA larger than 2 cm with severe LUTS and/or leukocytosis benefit from TRUS-guided aspiration. In addition, these patients are benefitted from urinary drainage (either perurethral or suprapubic). The algorithm also suggests that if two attempts of TRUS aspiration fail, these patients benefit from transurethral drainage.
Keywords: LUTS; TRUS; prostate imaging; prostatic abscess.
Conflict of interest statement
Figures


References
-
- Kodman D, Ling D, Lee JKT. Percutaneous drainage of prostatic abscesses. J Urol. 1986;135:1259–60. - PubMed
-
- Zighelboim J, Goldfarb RA, Mody D. Prostatic abscess due to Histoplasma capsulatum in patient with the acquired immunodeficiency syndrome. J Urol. 1992;147:166–8. - PubMed
-
- Ludwig M, Schroeder-Printzen I, Schiefer HC, Weidner W. Diagnosis and therapeutic management of 18 patients with prostatic abscess. Urology. 1999;53:340–5. - PubMed
-
- Mariani AJ, Jacobs LD, Hariharan A. Emphesemoatous Prostatic abscess Diagnosis and Treatment. J Urol. 1983;129:385–6. - PubMed
-
- Pai MG, Bhat HS. Prostatic abscess. J Urol. 1972;108:599–600. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

