Dermatomyositis associated with malignancy: A report of 3 cases
- PMID: 24350018
- PMCID: PMC3853903
- DOI: 10.4103/2229-5178.120664
Dermatomyositis associated with malignancy: A report of 3 cases
Abstract
The association between dermatomyositis (DMS) and various types of malignancies has been reported in several studies, with an estimated frequency of 20-25%. DMS may precede, accompany or follow the diagnosis of malignancy. In the present report, we have discussed three cases of dermatomyositis associated with malignancy. In the first case, DMS preceded the diagnosis of gastric adenocarcinoma while in the second and third cases, it followed the diagnosis of ductal carcinoma of the breast and transitional cell carcinoma of the bladder respectively. In all three patients, cutaneous and musculoskeletal features of DMS showed very good response to the treatment, irrespective of the course of malignancy.
Keywords: Dermatomyositis; ductal carcinoma of breast; gastric adenocarcinoma; transitional cell carcinoma of bladder.
Conflict of interest statement
Figures
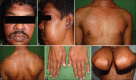


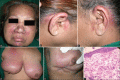


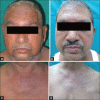
Similar articles
-
Paraneoplastic Dermatomyositis in a Patient with Metastatic Gastric Carcinoma.Acta Dermatovenerol Croat. 2020 Aug;28(2):120-122. Acta Dermatovenerol Croat. 2020. PMID: 32876041
-
Dermatomyositis in association with transitional cell carcinoma of the bladder.Clin Oncol (R Coll Radiol). 2001;13(1):50-1. doi: 10.1053/clon.2001.9214. Clin Oncol (R Coll Radiol). 2001. PMID: 11292137
-
Breast cancer and second primary ovarian cancer in dermatomyositis.Gynecol Oncol. 1991 Dec;43(3):286-90. doi: 10.1016/0090-8258(91)90037-6. Gynecol Oncol. 1991. PMID: 1752501
-
The value of malignancy evaluation in patients with dermatomyositis.J Am Acad Dermatol. 1982 Feb;6(2):253-9. doi: 10.1016/s0190-9622(82)70018-0. J Am Acad Dermatol. 1982. PMID: 7037882 Review.
-
Amyopathic Dermatomyositis: A Concise Review of Clinical Manifestations and Associated Malignancies.Am J Clin Dermatol. 2016 Oct;17(5):509-518. doi: 10.1007/s40257-016-0199-z. Am J Clin Dermatol. 2016. PMID: 27256496 Review.
References
-
- Ghate J, Katsambas A, Augerinou G, Jorizzo JL. Review article: A therapeutic update on dermatomyositis/polymyositis. Int J Dermatol. 2000;39:81–7. - PubMed
-
- Airio A, Pukkala E, Isomaki H. Elevated cancer incidence in patients with dermatomyositis: A population based study. J Rheumatol. 1995;22:1300–3. - PubMed
-
- Chen YJ, Wu CY, Shen JL. Predicting factors of malignancy in dermatomyositis and polymyositis: A case-control study. Br J Dermatol. 2001;144:825–31. - PubMed
-
- Leow YH, Goh CL. Malignancy in adult dermatomyositis. Int J Dermatol. 1997;36:904–7. - PubMed
-
- Sterz G. Polymyositis. Berliner Klinische Wochenschrift (Clinical Berlin Weekly) 1916;53:489.
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

