Patterns of recurrence after liver transplantation for nonresectable liver metastases from colorectal cancer
- PMID: 24370906
- PMCID: PMC3942624
- DOI: 10.1245/s10434-013-3449-9
Patterns of recurrence after liver transplantation for nonresectable liver metastases from colorectal cancer
Abstract
Background: Surgical resection is the only curative modality for colorectal liver metastases (CLM), and the pattern of recurrences after resection affects survival. In a prospective study of liver transplantation (Lt) for nonresectable CLM we have shown a 5-year overall survival rate of 60 %, but 19 of 21 experienced recurrence. This study reports the pattern of recurrences after Lt for CLM and the effect on survival.
Methods: Characterization of metastatic lesions in a prospective study for Lt for nonresectable CLM was performed (n = 21). The study included reexamination of chest computed tomographic scans taken before Lt.
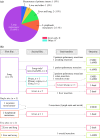
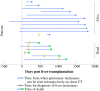
Results: At the time of first recurrence, 16 were a single site, and three were multiple sites. Thirteen of the single sites were pulmonary recurrences. The pulmonary recurrences appeared early and were slow growing, and several were accessible to surgical treatment. When chest computed tomographic scans were reexamined, seven patients had pulmonary nodules at the time of Lt without an effect on survival. There was no first single-site hepatic recurrence. Six of the seven patients who developed metastases to the transplanted liver died from metastatic disease.
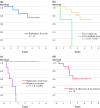
Conclusions: The pulmonary recurrences after Lt for CLM were of an indolent character, even those that were present at the time of Lt. This contrasts with the finding of metastases to the transplanted liver, which was prognostically adverse. The lack of single hepatic first-site recurrences and hepatic metastases only as part of disseminated disease is different from the pattern of recurrence after liver resection. This suggests two distinct mechanisms for hepatic recurrences after resection for CLM.
Figures
Similar articles
-
Is Liver Transplantation an Option in Colorectal Cancer Patients with Nonresectable Liver Metastases and Progression on All Lines of Standard Chemotherapy?Ann Surg Oncol. 2015 Jul;22(7):2195-200. doi: 10.1245/s10434-014-4137-0. Epub 2014 Oct 9. Ann Surg Oncol. 2015. PMID: 25297902
-
Predictive factors for time to recurrence, treatment and post-recurrence survival in patients with initially resected colorectal liver metastases.World J Surg Oncol. 2015 Dec 3;13:328. doi: 10.1186/s12957-015-0738-8. World J Surg Oncol. 2015. PMID: 26631156 Free PMC article.
-
Intrahepatic Recurrence Patterns Predict Survival After Resection of Colorectal Liver Metastases.Ann Surg Oncol. 2019 Jan;26(1):275-281. doi: 10.1245/s10434-018-6945-0. Epub 2018 Oct 25. Ann Surg Oncol. 2019. PMID: 30362064
-
[Diagnosis and treatment of colorectal liver metastases - workflow].Zentralbl Chir. 2008 Jun;133(3):267-84. doi: 10.1055/s-2008-1076796. Zentralbl Chir. 2008. PMID: 18563694 Review. German.
-
Aggressive repeat liver resection for hepatic metastases of colorectal carcinoma.Surg Today. 1992;22(3):260-4. doi: 10.1007/BF00308832. Surg Today. 1992. PMID: 1392331 Review.
Cited by
-
Salvage liver transplantation after resection of colorectal cancer liver metastasis with favorable outcomes: a case report and review of the literature.BMC Gastroenterol. 2021 Apr 27;21(1):191. doi: 10.1186/s12876-021-01778-6. BMC Gastroenterol. 2021. PMID: 33906639 Free PMC article. Review.
-
Liver transplantation for hepatobiliary malignancies: a new era of "Transplant Oncology" has begun.Surg Today. 2017 Apr;47(4):403-415. doi: 10.1007/s00595-016-1337-1. Epub 2016 Apr 29. Surg Today. 2017. PMID: 27130463 Review.
-
Colorectal cancer with potentially resectable hepatic metastases: optimizing treatment.Curr Oncol Rep. 2014 Oct;16(10):407. doi: 10.1007/s11912-014-0407-z. Curr Oncol Rep. 2014. PMID: 25129331 Review.
-
Liver transplantation for non-resectable colorectal metastases-an evolving paradigm in transplant oncology.Hepatobiliary Surg Nutr. 2023 Jun 1;12(3):424-427. doi: 10.21037/hbsn-23-200. Epub 2023 May 22. Hepatobiliary Surg Nutr. 2023. PMID: 37351144 Free PMC article. No abstract available.
-
Liver transplantation as a new treatment option for perihilar cholangiocarcinoma and colorectal liver metastases: a review.Int J Clin Oncol. 2025 Jul 5. doi: 10.1007/s10147-025-02820-3. Online ahead of print. Int J Clin Oncol. 2025. PMID: 40616773 Review.
References
-
- de Jong MC, Pulitano C, Ribero D, et al. Rates and patterns of recurrence following curative intent surgery for colorectal liver metastasis: an international multi-institutional analysis of 1,669 patients. Ann Surg. 2009;250:440–448. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

