TRPV1 channel-mediated bilateral allodynia induced by unilateral masseter muscle inflammation in rats
- PMID: 24377488
- PMCID: PMC3880456
- DOI: 10.1186/1744-8069-9-68
TRPV1 channel-mediated bilateral allodynia induced by unilateral masseter muscle inflammation in rats
Abstract
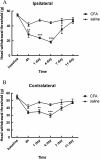
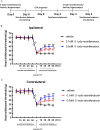
Pain in masticatory muscles is among the most prominent symptoms of temperomandibular disorders (TMDs) that have diverse and complex etiology. A common complaint of TMD is that unilateral pain of craniofacial muscle can cause a widespread of bilateral pain sensation, although the underlying mechanism remains unknown. To investigate whether unilateral inflammation of masseter muscle can cause a bilateral allodynia, we generated masseter muscle inflammation induced by unilateral injection of complete Freund's adjuvant (CFA) in rats, and measured the bilateral head withdrawal threshold at different time points using a von Frey anesthesiometer. After behavioral assessment, both right and left trigeminal ganglia (TRG) were dissected and examined for histopathology and transient receptor potential vanilloid 1 (TRPV1) mRNA expression using quantitative real-time PCR analysis. A significant increase in TRPV1 mRNA expression occurred in TRG ipsilateral to CFA injected masseter muscle, whereas no significant alteration in TRPV1 occurred in the contralateral TRG. Interestingly, central injection of TRPV1 antagonist 5-iodoresiniferatoxin into the hippocampus significantly attenuated the head withdrawal response of both CFA injected and non-CFA injected contralateral masseter muscle. Our findings show that unilateral inflammation of masseter muscle is capable of inducing bilateral allodynia in rats. Upregulation of TRPV1 at the TRG level is due to nociception caused by inflammation, whereas contralateral nocifensive behavior in masticatory muscle nociception is likely mediated by central TRPV1, pointing to the involvement of altered information processing in higher centers.
Figures

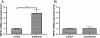

Similar articles
-
The role of P2X3 receptors in bilateral masseter muscle allodynia in rats.Croat Med J. 2016 Dec 31;57(6):530-539. doi: 10.3325/cmj.2016.57.530. Croat Med J. 2016. PMID: 28051277 Free PMC article.
-
Transcriptome analysis of trigeminal ganglia following masseter muscle inflammation in rats.Mol Pain. 2016 Oct 4;12:1744806916668526. doi: 10.1177/1744806916668526. Print 2016. Mol Pain. 2016. PMID: 27702909 Free PMC article.
-
Effect of Testosterone on TRPV1 Expression in a Model of Orofacial Myositis Pain in the Rat.J Mol Neurosci. 2018 Jan;64(1):93-101. doi: 10.1007/s12031-017-1009-7. Epub 2017 Dec 5. J Mol Neurosci. 2018. PMID: 29209900
-
Role of TRPV1 and ASIC3 channels in experimental occlusal interference-induced hyperalgesia in rat masseter muscle.Eur J Pain. 2016 Apr;20(4):552-63. doi: 10.1002/ejp.758. Epub 2015 Jul 22. Eur J Pain. 2016. PMID: 26201614
-
Neural Pathways of Craniofacial Muscle Pain: Implications for Novel Treatments.J Dent Res. 2020 Aug;99(9):1004-1012. doi: 10.1177/0022034520919384. Epub 2020 May 6. J Dent Res. 2020. PMID: 32374638 Free PMC article. Review.
Cited by
-
Lack of evidence for ectopic sprouting of genetically labeled Aβ touch afferents in inflammatory and neuropathic trigeminal pain.Mol Pain. 2015 Apr 10;11:18. doi: 10.1186/s12990-015-0017-2. Mol Pain. 2015. PMID: 25880319 Free PMC article.
-
[Hippocampus is involved in 17β-estradiol exacerbating experimental occlusal inter- ference-induced chronic masseter hyperalgesia in ovariectomized rats].Beijing Da Xue Xue Bao Yi Xue Ban. 2022 Feb 18;54(1):40-47. doi: 10.19723/j.issn.1671-167X.2022.01.007. Beijing Da Xue Xue Bao Yi Xue Ban. 2022. PMID: 35165466 Free PMC article. Chinese.
-
Assessment of mechanical allodynia in healthy teeth adjacent and contralateral to endodontically diseased teeth: a clinical study.Restor Dent Endod. 2024 Jul 29;49(3):e31. doi: 10.5395/rde.2024.49.e31. eCollection 2024 Aug. Restor Dent Endod. 2024. PMID: 39247644 Free PMC article.
-
Role of medullary astroglial glutamine synthesis in tooth pulp hypersensitivity associated with frequent masseter muscle contraction.Mol Pain. 2018 Jan-Dec;14:1744806918763270. doi: 10.1177/1744806918763270. Epub 2018 Feb 15. Mol Pain. 2018. PMID: 29448913 Free PMC article.
-
Bilateral increases in ERK activation at the spinomedullary junction region by acute masseter muscle injury during temporomandibular joint inflammation in the rats.Exp Brain Res. 2017 Mar;235(3):913-921. doi: 10.1007/s00221-016-4852-9. Epub 2016 Dec 8. Exp Brain Res. 2017. PMID: 27933357
References
-
- Brazeau GA, Gremillion HA, Widmer CG, Mahan PE, Benson MB, Mauderli AP, Riley JL 3rd, Smith CL. The role of pharmacy in the management of patients with temporomandibular disorders and orofacial pain. J Am Pharm Assoc (Wash) 1998;9:354–361. quiz 362–353. - PubMed
-
- Machado LP, Nery Cde G, Leles CR, Nery MB, Okeson JP. The prevalence of clinical diagnostic groups in patients with temporomandibular disorders. Cranio. 2009;9:194–199. - PubMed
-
- Svensson P, Graven-Nielsen T. Craniofacial muscle pain: review of mechanisms and clinical manifestations. J Orofac Pain. 2001;9:117–145. - PubMed
-
- Stohler CS. Muscle-related temporomandibular disorders. J Orofac Pain. 1999;9:273–284. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

