Using the ACS-NSQIP to identify factors affecting hospital length of stay after elective posterior lumbar fusion
- PMID: 24384669
- PMCID: PMC3961012
- DOI: 10.1097/BRS.0000000000000184
Using the ACS-NSQIP to identify factors affecting hospital length of stay after elective posterior lumbar fusion
Abstract
Study design: Retrospective cohort study of the American College of Surgeons National Surgical Quality Improvement Program database from 2005 to 2010 that included 1861 patients who had undergone elective posterior lumbar fusion.
Objective: To characterize factors that were independently associated with increased hospital length of stay (LOS) in patients who had undergone elective posterior lumbar fusion.
Summary of background data: Posterior lumbar spine fusion is a common surgical procedure used to treat lumbar spine pathology. LOS is an important clinical variable and a major determinant of inpatient hospital costs. There is lack of studies in the literature using multivariate analysis to examine specifically the predictors of LOS after elective posterior lumbar fusion.
Methods: Patients who underwent elective posterior lumbar fusion from 2005 to 2010 were identified in the American College of Surgeons National Surgical Quality Improvement Program database. Preoperative and intraoperative variables were extracted for each case and a multivariate linear regression was performed to assess the contribution of each variable to LOS.
Results: A total of 1861 patients who had undergone elective posterior lumbar fusion were identified. The average age for patients in this cohort was 60.6 ± 13.9 years (mean ± standard deviation) with a body mass index of 30.3 ± 6.2 kg/m. Of the total patients, 44.7% of patients were male. LOS was in the range from 0 days to 51 days. Multivariate linear regression identified age (P < 0.001), morbid obesity (body mass index ≥ 40 kg/m, P < 0.001), American Society of Anesthesiologists class (P = 0.001), operative time (P < 0.001), multilevel procedure (P = 0.001), and intraoperative transfusion (P < 0.001) as significant predictors of extended LOS.
Conclusion: The identified preoperative and intraoperative variables associated with extended LOS after elective posterior lumbar fusion may be helpful to clinicians for patient counseling and postoperative planning.
Level of evidence: 3.
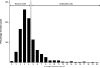
Figures
References
-
- Goz V, Weinreb JH, McCarthy I, et al. Perioperative Complications and Mortality After Spinal Fusions: Analysis of Trends and Risk Factors. Spine. 2013 - PubMed
-
- Epstein NE, Schwall G, Reillly T, et al. Surgeon choices, and the choice of surgeons, affect total hospital charges for single-level anterior cervical surgery. Spine. 2011;36:905–9. - PubMed
-
- Browne JA, Cook C, Pietrobon R, et al. Diabetes and early postoperative outcomes following lumbar fusion. Spine. 2007;32:2214–9. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical