Campylobacteriosis in urban versus rural areas: a case-case study integrated with molecular typing to validate risk factors and to attribute sources of infection
- PMID: 24386265
- PMCID: PMC3873381
- DOI: 10.1371/journal.pone.0083731
Campylobacteriosis in urban versus rural areas: a case-case study integrated with molecular typing to validate risk factors and to attribute sources of infection
Abstract
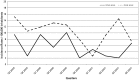
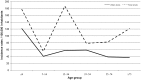
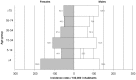
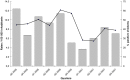
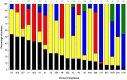
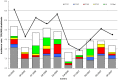
Campylobacter infection is a leading cause of bacterial gastroenteritis worldwide, and most clinical cases appear as isolated, sporadic infections for which the source is rarely apparent. From July 2005 to December 2007 we conducted a prospective case-case study of sporadic, domestically-acquired Campylobacter enteritis in rural versus urban areas and a prevalence study of Campylobacter in animal and environmental sources in the Eastern Townships, Quebec. Isolates were typed using Multilocus Sequence Typing (MLST) to reinforce the case-case findings and to assign a source probability estimate for each human isolate. The risk of human campylobacteriosis was 1.89-fold higher in rural than urban areas. Unconditional multivariate logistic regression analysis identified two independent risk factors associated with human Campylobacter infections acquired in rural area: occupational exposure to animals (OR = 10.6, 95% CI: 1.2-91, p = 0.032), and household water coming from a private well (OR = 8.3, 95% CI: 3.4-20.4, p<0.0001). A total of 851 C. jejuni isolates (178 human, 257 chicken, 87 bovine, 266 water, 63 wild bird) were typed using MLST. Among human isolates, the incidence rates of clonal complexes (CC) CC-21, CC-45, and CC-61 were higher in rural than urban areas. MLST-based source attribution analysis indicated that 64.5% of human C. jejuni isolates were attributable to chicken, followed by cattle (25.8%), water (7.4%), and wild birds (2.3%). Chicken was the attributable source for the majority of cases, independent of residential area, sex and age. The increased incidence in rural compared to urban areas was associated with occupational exposure to animals, particularly cattle among those aged 15-34 years, and with consumption of private well water. Both bovine and water exposure appeared to contribute to the seasonal variation in campylobacteriosis. These results provide a basis for developing public education and preventive programs targeting the risk factors identified.
Conflict of interest statement
Figures

Similar articles
-
Attribution of Campylobacter infections in northeast Scotland to specific sources by use of multilocus sequence typing.J Infect Dis. 2009 Apr 15;199(8):1205-8. doi: 10.1086/597417. J Infect Dis. 2009. PMID: 19265482 Free PMC article.
-
Human Campylobacteriosis in Luxembourg, 2010-2013: A Case-Control Study Combined with Multilocus Sequence Typing for Source Attribution and Risk Factor Analysis.Sci Rep. 2016 Feb 10;6:20939. doi: 10.1038/srep20939. Sci Rep. 2016. PMID: 26860258 Free PMC article.
-
Risk factors for campylobacteriosis of chicken, ruminant, and environmental origin: a combined case-control and source attribution analysis.PLoS One. 2012;7(8):e42599. doi: 10.1371/journal.pone.0042599. Epub 2012 Aug 3. PLoS One. 2012. PMID: 22880049 Free PMC article.
-
A systematic review of source attribution of human campylobacteriosis using multilocus sequence typing.Euro Surveill. 2019 Oct;24(43):1800696. doi: 10.2807/1560-7917.ES.2019.24.43.1800696. Euro Surveill. 2019. PMID: 31662159 Free PMC article.
-
Campylobacteriosis Outbreak Linked to Municipal Water, Nebraska, USA, 20211.Emerg Infect Dis. 2024 Oct;30(10):1998-2005. doi: 10.3201/eid3010.231509. Emerg Infect Dis. 2024. PMID: 39320141 Free PMC article. Review.
Cited by
-
Non food-related risk factors of campylobacteriosis in Canada: a matched case-control study.BMC Public Health. 2016 Sep 27;16(1):1016. doi: 10.1186/s12889-016-3679-4. BMC Public Health. 2016. PMID: 27677338 Free PMC article.
-
Genomic diversity, virulence and source of Campylobacter jejuni contamination in Irish poultry slaughterhouses by whole genome sequencing.J Appl Microbiol. 2022 Nov;133(5):3150-3160. doi: 10.1111/jam.15753. Epub 2022 Aug 22. J Appl Microbiol. 2022. PMID: 35993276 Free PMC article.
-
Dogs and Cats: Reservoirs for Highly Diverse Campylobacter jejuni and a Potential Source of Human Exposure.Animals (Basel). 2020 May 12;10(5):838. doi: 10.3390/ani10050838. Animals (Basel). 2020. PMID: 32408633 Free PMC article.
-
Survival in water of Campylobacter jejuni strains isolated from the slaughterhouse.Springerplus. 2015 Dec 22;4(1):799. doi: 10.1186/s40064-015-1595-1. eCollection 2015. Springerplus. 2015. PMID: 26702388 Free PMC article.
-
Phenotypic and Transcriptomic Responses of Campylobacter jejuni Suspended in an Artificial Freshwater Medium.Front Microbiol. 2017 Sep 20;8:1781. doi: 10.3389/fmicb.2017.01781. eCollection 2017. Front Microbiol. 2017. PMID: 28979243 Free PMC article.
References
-
- Michaud S, Menard S, Gaudreau C, Arbeit RD (2001) Comparison of SmaI-defined genotypes of Campylobacter jejuni examined by KpnI: a population-based study. J Med Microbiol 50: 1075–1081. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

