Sex differences in HIV outcomes in the highly active antiretroviral therapy era: a systematic review
- PMID: 24401107
- PMCID: PMC4010172
- DOI: 10.1089/AID.2013.0208
Sex differences in HIV outcomes in the highly active antiretroviral therapy era: a systematic review
Abstract
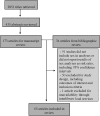
To assess sex disparities in AIDS clinical and laboratory outcomes in the highly active antiretroviral therapy (HAART) era we conducted a systematic review of the published literature on mortality, disease progression, and laboratory outcomes among persons living with HIV and starting HAART. We performed systematic PubMed and targeted bibliographic searches of observational studies published between January, 1998, and November, 2013, that included persons starting HAART and reported analyses of mortality, progression to AIDS, or virologic or immunologic treatment outcomes by sex. Risk ratios (relative risks, odd ratios, and hazard ratios) and 95% confidence intervals were obtained. Sixty-five articles were included in this review. Thirty-nine studies were from North America and Europe and 26 were from Latin America, Asia, and Africa. Forty-four studies (68%) showed no statistically significant difference in risk of mortality, progression to AIDS, or virologic or immunologic treatment outcomes by sex. Decreased risk of death among females compared to males was observed in 24 of the 25 articles that included mortality analyses [pooled risk ratio 0.72 (95% confidence interval=0.69-0.75)], and decreased risk of death or AIDS was observed in 9 of the 13 articles that examined the composite outcome [pooled risk ratio=0.91 (0.84-0.98)]. There was no significant effect of sex on the risk of progression to AIDS [pooled risk ratio=1.15 (0.99-1.31)]. In this systematic review, females starting HAART appeared to have improved survival compared to males. However, this benefit was not associated with decreased progression to either AIDS or to differences in virologic or immunologic treatment outcomes.
Figures




Similar articles
-
Optimal monitoring strategies for guiding when to switch first-line antiretroviral therapy regimens for treatment failure in adults and adolescents living with HIV in low-resource settings.Cochrane Database Syst Rev. 2010 Apr 14;(4):CD008494. doi: 10.1002/14651858.CD008494. Cochrane Database Syst Rev. 2010. PMID: 20393969
-
Treatment of severe or progressive Kaposi's sarcoma in HIV-infected adults.Cochrane Database Syst Rev. 2014;(9):CD003256. doi: 10.1002/14651858.CD003256.pub2. Cochrane Database Syst Rev. 2014. PMID: 25313415
-
Treatment of severe or progressive Kaposi's sarcoma in HIV-infected adults.Cochrane Database Syst Rev. 2014 Aug 13;8(8):CD003256. doi: 10.1002/14651858.CD003256.pub2. Cochrane Database Syst Rev. 2014. PMID: 25221796 Free PMC article.
-
Structured treatment interruptions (STI) in chronic unsuppressed HIV infection in adults.Cochrane Database Syst Rev. 2006 Jul 19;2006(3):CD006148. doi: 10.1002/14651858.CD006148. Cochrane Database Syst Rev. 2006. PMID: 16856117 Free PMC article.
-
Optimisation of antiretroviral therapy in HIV-infected children under 3 years of age.Cochrane Database Syst Rev. 2014 May 22;2014(5):CD004772. doi: 10.1002/14651858.CD004772.pub4. Cochrane Database Syst Rev. 2014. PMID: 24852077 Free PMC article.
Cited by
-
Sex and Race Disparities in Mortality and Years of Potential Life Lost Among People With HIV: A 21-Year Observational Cohort Study.Open Forum Infect Dis. 2022 Dec 19;10(1):ofac678. doi: 10.1093/ofid/ofac678. eCollection 2023 Jan. Open Forum Infect Dis. 2022. PMID: 36726547 Free PMC article.
-
Retention in Care and Virological Failure among Adult HIV-Positive Patients on First-Line Antiretroviral Treatment in Maputo, Mozambique.Viruses. 2023 Sep 22;15(10):1978. doi: 10.3390/v15101978. Viruses. 2023. PMID: 37896757 Free PMC article.
-
Possible protective role of 17β-estradiol against COVID-19.J Allergy Infect Dis. 2020;1(2):38-48. doi: 10.46439/allergy.1.010. Epub 2020 Aug 19. J Allergy Infect Dis. 2020. PMID: 33196058 Free PMC article.
-
Temporal changes in ART initiation in adults with high CD4 counts in Latin America: a cohort study.J Int AIDS Soc. 2019 Dec;22(12):e25413. doi: 10.1002/jia2.25413. J Int AIDS Soc. 2019. PMID: 31855320 Free PMC article.
-
Virological and immunological failure of HAART and associated risk factors among adults and adolescents in the Tigray region of Northern Ethiopia.PLoS One. 2018 May 1;13(5):e0196259. doi: 10.1371/journal.pone.0196259. eCollection 2018. PLoS One. 2018. PMID: 29715323 Free PMC article.
References
-
- Soon GG, Min M, Struble KA, et al. : Meta-analysis of gender differences in efficacy outcomes for HIV-positive subjects in randomized controlled clinical trials of antiretroviral therapy (2000–2008). AIDS Patient Care STDs 2012;26:444–453 - PubMed
-
- Ballesteros-Zebadua P, Villarreal C, Cocho G, Huerta L, and Estrada JL: Differences in HIV-1 viral loads between male and female antiretroviral-untreated Mexican patients. Arch Med Res 2013;44:296–301 - PubMed
-
- Sterling TR, Vlahov D, Astemborski J, Hoover DR, Margolick JB, and Quinn TC: Initial plasma HIV-1 RNA levels and progression to AIDS in women and men. N Engl J Med 2001;344:720–725 - PubMed
-
- Moore AL, Kirk O, Johnson AM, et al. : Virologic, immunologic, and clinical response to highly active antiretroviral therapy: The gender issue revisited. J Acquir Immune Defic Syndr 2003;32:452–461 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

