Cisternostomy: Replacing the age old decompressive hemicraniectomy?
- PMID: 24403955
- PMCID: PMC3877499
- DOI: 10.4103/1793-5482.121684
Cisternostomy: Replacing the age old decompressive hemicraniectomy?
Abstract
Backround: Practical scenario in trauma neurosurgery comes with multiple challenges and limitations. It accounts for the maximum mortality in neurosurgery and yet the developing countries are still ill-equipped even for an emergency set-up for primary management of traumatic brain injuries. The evolution of modern neurosurgical techniques in traumatic brain injury has been ongoing for the last two centuries. However, it has always been a challenge to obtain a satisfactory clinical outcome, especially those following severe traumatic brain injuries. Other than the well-established procedures such as decompressive hemicraniectomy and those for acute and or chronic subdural hematomas and depressed skull fractures, contusions etcetera newer avenues for development of surgical techniques where indicated have been minimal. We are advocating a replacement for decompressive hemicranictomy, which would have the same indications as decompressive hemicraniectomy. The results of this procedure has been compared with the results of decompressive hemicraniectomy done in our institution and elsewhere and has been proven beyond doubts to be superior to decompressive hemicraniectomy. This procedure is elegant and can replace decompressive hemicraniectomy because of low morbidity and mortality. However, there is a steep learning curve and the microscope has to be used.
Materials and methods: Based on the clinical experience and observation of acute neurosurgical service in tertiary medical centers in a developing country, the procedure of cisternostomy in the management of trauma neurosurgery have been elucidated in the current study. The study proposes to apply the principles of microvascular surgery and skull base surgery in selected cases of severe traumatic brain injuries, thus replacing decompressive hemicraniectomy as the primary modality of treatment for indicated cases.
Conclusion: Extensive opening of cisterns making use of skull base techniques to approach them in a swollen brain is a better option to decompressive hemicraniectomy for the same indications.
Keywords: Brain swelling; cisterns; decompressive hemicraniectomy; intra brain pressure; intra cisternal pressure.
Conflict of interest statement
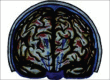
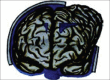
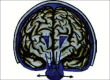
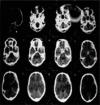
Figures



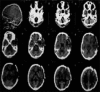
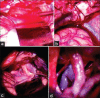
Similar articles
-
Post-operative expansion of hemorrhagic contusions after unilateral decompressive hemicraniectomy in severe traumatic brain injury.J Neurotrauma. 2008 May;25(5):503-12. doi: 10.1089/neu.2007.0442. J Neurotrauma. 2008. PMID: 18346002
-
Cisternostomy for Traumatic Brain Injury: Pathophysiologic Mechanisms and Surgical Technical Notes.World Neurosurg. 2016 May;89:51-7. doi: 10.1016/j.wneu.2016.01.072. Epub 2016 Feb 4. World Neurosurg. 2016. PMID: 26851743
-
Decompressive craniectomy in acute brain injury.Handb Clin Neurol. 2017;140:299-318. doi: 10.1016/B978-0-444-63600-3.00016-7. Handb Clin Neurol. 2017. PMID: 28187804 Review.
-
Cisternostomy: A Timely Intervention in Moderate to Severe Traumatic Brain Injuries: Rationale, Indications, and Prospects.World Neurosurg. 2019 Nov;131:385-390. doi: 10.1016/j.wneu.2019.07.082. World Neurosurg. 2019. PMID: 31658580
-
Refractory Intracranial Hypertension: The Role of Decompressive Craniectomy.Anesth Analg. 2017 Dec;125(6):1999-2008. doi: 10.1213/ANE.0000000000002399. Anesth Analg. 2017. PMID: 28806209 Review.
Cited by
-
The Conundrum of Ventricular Dilatations Following Decompressive Craniectomy: Is Ventriculoperitoneal Shunt, The Only Panacea?J Neurosci Rural Pract. 2018 Apr-Jun;9(2):232-239. doi: 10.4103/jnrp.jnrp_395_17. J Neurosci Rural Pract. 2018. PMID: 29725175 Free PMC article.
-
The basal cisternostomy for management of severe traumatic brain injury: A retrospective study.Chin J Traumatol. 2025 Mar;28(2):118-123. doi: 10.1016/j.cjtee.2024.09.007. Epub 2024 Nov 20. Chin J Traumatol. 2025. PMID: 39632242 Free PMC article.
-
Is basal cisternostomy in traumatic brain injury a need of hour or white elephant - A randomized trial to answer.Surg Neurol Int. 2023 Dec 1;14:412. doi: 10.25259/SNI_825_2023. eCollection 2023. Surg Neurol Int. 2023. PMID: 38213437 Free PMC article.
-
[Focus neurosurgical intensive care medicine : Summary of selected intensive medical care studies].Anaesthesiologie. 2023 Jul;72(7):518-525. doi: 10.1007/s00101-023-01287-z. Epub 2023 May 17. Anaesthesiologie. 2023. PMID: 37195500 German. No abstract available.
-
Basal Cisternostomy for Severe TBI: Surgical Technique and Cadaveric Dissection.Front Surg. 2022 May 6;9:915818. doi: 10.3389/fsurg.2022.915818. eCollection 2022. Front Surg. 2022. PMID: 35599786 Free PMC article.
References
-
- Corrigan JD, Selassie AW, Orman JA. The epidemiology of traumatic brain injury. J Head Trauma Rehabil. 2010;25:72–80. - PubMed
-
- Murray CJ, Lopez AD. Evidence-based health policy – Lessons from the Global Burden of Disease Study. Science. 1996;274:740–3. - PubMed
-
- Li LM, Timofeev I, Czosnyka M, Hutchinson PJ. Review article: The surgical approach to the management of increased intracranial pressure after traumatic brain injury. Anesth Analg. 2010;111:736–48. - PubMed
-
- Sindou M. Favourable influence of opening the lamina terminalis and Lilliequist's membrane on the outcome of ruptured intracranial aneurysms. A study of 197 consecutive cases. Acta Neurochir (Wien) 1994;127:15–6. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

