Unidirectionally progressive left pneumonectomy & mediastinal lymph node dissection
- PMID: 24416507
- PMCID: PMC3886847
- DOI: 10.3978/j.issn.2072-1439.2013.11.36
Unidirectionally progressive left pneumonectomy & mediastinal lymph node dissection
Abstract
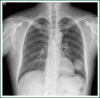
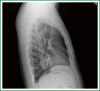
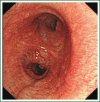
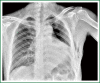
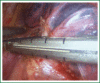
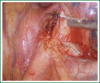
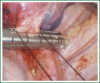
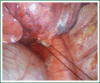
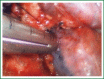
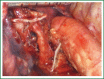
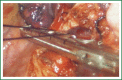
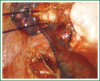
The patient has lower left lung tumor and adenocarcinoma at the openings of both upper and lower left lung. Preoperative bronchoscopic biopsy has confirmed the diagnosis. The surgical approach is unidirectionally progressive left pneumonectomy + mediastinal lymph node dissection. The layers of structure are treated one after another until the fissure from a single direction through the working port. Hence, the resecting order should be left superior pulmonary vein-left lower pulmonary vein-left main bronchus-left pulmonary artery. The vessels and bronchi are cut using an endoscopic linear stapler or the Hemolock clips. The resected lobe is placed into a large-size specimen bag and retrieved through the working port to prevent contamination of the chest incision by any tumor tissue. Mediastinal lymph node dissection is performed at the end. The surgery is performed under general anesthesia with double-lumen endotracheal intubation. The patient is placed in a 90-degree position lying on the unaffected side. Similar to traditional resection of left lung lobes, an approximately 1.5-cm observation port is created in the 7th intercostal space between the middle and anterior axillary lines, an approximately 4-cm working port in the 4th intercostal space between the anterior axillary line and the midclavicular line, and an approximately 1.5-cm auxiliary port in the 9th intercostal space between the posterior axillary line and the subscapular line. The operator stands in front of the patient, manipulating the endoscopic instruments while watching the monitor.
Keywords: Thoracoscopic operation; left pneumonectomy; unidirectionally progressive.
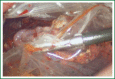
Figures


Similar articles
-
Unidirectionally progressive resection of lower right lung cancer under video-assisted thoracoscopy.J Thorac Dis. 2013 Aug;5 Suppl 3(Suppl 3):S310-4. doi: 10.3978/j.issn.2072-1439.2013.08.07. J Thorac Dis. 2013. PMID: 24040552 Free PMC article.
-
Thoracoscopic and laparoscopic oesophagectomy improves the quality of extended lymphadenectomy.Surg Endosc. 2006 Aug;20(8):1308-9. doi: 10.1007/s00464-006-2020-1. Epub 2006 Jul 31. Surg Endosc. 2006. PMID: 16897282
-
Multimedia article. Entirely thoracoscopic pneumonectomy using the prone position: a new technique.Surg Endosc. 2005 Sep;19(9):1282-3. doi: 10.1007/s00464-004-2114-6. Epub 2005 Jul 28. Surg Endosc. 2005. PMID: 16249969
-
Video-assisted thoracic surgery right upper lobe bronchial sleeve resection.J Vis Surg. 2016 Jan 18;2:18. doi: 10.3978/j.issn.2221-2965.2016.01.03. eCollection 2016. J Vis Surg. 2016. PMID: 29078446 Free PMC article.
-
Case of thoracoscopic right upper lobectomy for lung cancer with tracheal bronchus and a pulmonary vein variation.Asian J Endosc Surg. 2012 May;5(2):93-5. doi: 10.1111/j.1758-5910.2011.00115.x. Asian J Endosc Surg. 2012. PMID: 22776372 Review.
Cited by
-
Unidirectionally progressive resection of left upper pulmonary lobe under video-assisted thoracoscopy.J Thorac Dis. 2014 Dec;6(12):1843-7. doi: 10.3978/j.issn.2072-1439.2014.12.26. J Thorac Dis. 2014. PMID: 25589987 Free PMC article.
-
Unidirectionally progressive resection of lower left lung carcinoma under video-associated thoracoscopy.J Thorac Dis. 2015 Dec;7(12):2371-5. doi: 10.3978/j.issn.2072-1439.2015.12.49. J Thorac Dis. 2015. PMID: 26793362 Free PMC article.
-
Inhibition of BPHL inhibits proliferation in lung carcinoma cell lines.Transl Lung Cancer Res. 2023 May 31;12(5):1051-1061. doi: 10.21037/tlcr-23-225. Epub 2023 May 29. Transl Lung Cancer Res. 2023. PMID: 37323178 Free PMC article.
References
-
- He JX. Atlas of minimally invasive thoracic surgery. Guangzhou: Guangdong Science and Technology Publishing House, 2005:195-228.
-
- Pu JT, Dai TY, Tang XJ, et al. VATS Thoracic Small Incision and Conventional Surgery for Lung Cancer: Comparison of Therapy Effect and Impact on Blood Coagulation. Chinese Modern Doctor 2010;48:5-7
-
- Seder CW, Hanna K, Lucia V, et al. The safe transition from open to thoracoscopic lobectomy: a 5-year experience. Ann Thorac Surg 2009;88:216-25; discussion 225-6 - PubMed
-
- Kim K, Kim HK, Park JS, et al. Video-assisted thoracic surgery lobectomy: single institutional experience with 704 cases. Ann Thorac Surg 2010;89:S2118-22 - PubMed
-
- Liu XL, Che GW, Pu Q, et al. Single-direction VATS lobectomy. Chinese Journal of Thoracic and Cardiovascular Surgery 2008;24:156-8
Publication types
LinkOut - more resources
Full Text Sources
