Optic nerve monitoring
- PMID: 24436741
- PMCID: PMC3721018
- DOI: 10.1055/s-0033-1343783
Optic nerve monitoring
Abstract
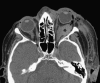
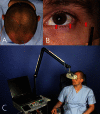
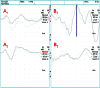
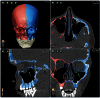
Orbital and anterior skull base surgery is generally performed close to the prechiasmatic visual pathway, and clear strategies for detecting and handling visual pathway damage are essential. To overcome the common problem of a missed clinical examination because of an uncooperative or unresponsive patient, flash visual evoked potentials and electroretinograms should be used. These electrophysiologic examination techniques can provide evidence of intact, pathologic, or absent conductivity of the visual pathway when clinical assessment is not feasible. Visual evoked potentials and electroretinograms are thus essential diagnostic procedures not only for primary diagnosis but also for intraoperative evaluation. A decision for or against treatment of a visual pathway injury has to be made as fast as possible due to the enormous importance of the time elapsed with such injuries; this can be achieved additionally using multislice spiral computed tomography. The first-line conservative treatment of choice for such injuries is megadose methylprednisolone therapy. Surgery is used to decompress the orbital compartment by exposure of the intracanalicular part of the optic nerve in the case of optic canal compression. Modern craniomaxillofacial surgery requires detailed consideration of the diagnosis and treatment of traumatic visual pathway damage with the ultimate goal of preserving visual acuity.
Keywords: flash visual evoked potentials (VEPs); megadose methylprednisolone; optic nerve decompression; optic nerve trauma; visual pathway damage.
Figures
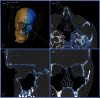
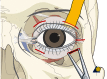

References
-
- Lang J. [Posterior ethmoid cells and their relation to the optic canal] HNO. 1988;6:49–53. - PubMed
-
- Osguthorpe J D, Sofferman R A. Optic nerve decompression. Otolaryngol Clin North Am. 1988;6:155–169. - PubMed
-
- Wolin M J, Lavin P J. Spontaneous visual recovery from traumatic optic neuropathy after blunt head injury. Am J Ophthalmol. 1990;6:430–435. - PubMed
-
- Elisevich K V, Ford R M, Anderson D P, Stratford J G, Richardson P M. Visual abnormalities with multiple trauma. Surg Neurol. 1984;6:565–575. - PubMed
-
- Habal M B, Maniscalco J E, Rhoton A L Jr. Microsurgical anatomy of the optic canal: correlates to optic nerve exposure. J Surg Res. 1977;6:527–533. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
