Self-rated health and long-term prognosis of depression
- PMID: 24445104
- PMCID: PMC3896539
- DOI: 10.1370/afm.1562
Self-rated health and long-term prognosis of depression
Abstract
Purpose: Indicators of prognosis should be considered to fully inform clinical decision making in the treatment of depression. This study examines whether self-rated health predicts long-term depression outcomes in primary care.
Methods: Our analysis was based on the first 5 years of a prospective 10-year cohort study underway since January 2005 conducted in 30 randomly selected Australian primary care practices. Participants were 789 adult patients with a history of depressive symptoms. Main outcome measures include risks, risk differences, and risk ratios of major depressive syndrome (MDS) on the Patient Health Questionnaire.
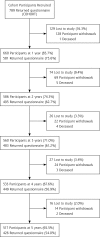
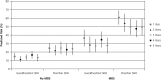
Results: Retention rates during the 5 years were 660 (84%), 586 (74%), 560 (71%), 533 (68%), and 517 (66%). At baseline, MDS was present in 27% (95% CI, 23%-30%). Cross-sectional analysis of baseline data showed participants reporting poor or fair self-rated health had greater odds of chronic illness, MDS, and lower socioeconomic status than those reporting good to excellent self-rated health. For participants rating their health as poor to fair compared with those rating it good to excellent, risk ratios of MDS were 2.10 (95% CI, 1.60-2.76), 2.38 (95% CI, 1.77-3.20), 2.22 (95% CI, 1.70-2.89), 1.73 (95% CI, 1.30-2.28), and 2.15 (95% CI, 1.59-2.90) at 1, 2, 3, 4, and 5 years, after accounting for missing data using multiple imputation. After adjusting for age, sex, multimorbidity, and depression status and severity, self-rated health remained a predictor of MDS up to 5 years.
Conclusions: Self-rated health offers family physicians an efficient and simple way to identify patients at risk of poor long-term depression outcomes and to inform therapeutic decision making.
Keywords: depression; longitudinal study; primary care; prognosis; self-rated health.
Figures
References
-
- World Health Organization (WHO) The Global Burden of Disease: 2004 Update. Geneva, Switzerland: World Health Organization; 2008
-
- Bloom DE, Cafiero ET, Jané-Llopis E, et al. The Global Economic Burden of Non-communicable Diseases. Geneva, Switzerland: World Economic Forum; 2011
-
- Australian Bureau of Statistics National Survey of Mental Health and Wellbeing: Summary of Results, 2007. Canberra, Australia; 2007
-
- Herrman H, Patrick DL, Diehr P, et al. Longitudinal investigation of depression outcomes in primary care in six countries: the LIDO study. Functional status, health service use and treatment of people with depressive symptoms. Psychol Med. 2002;32(5):889–902 - PubMed
-
- Cassano P, Fava M. Depression and public health: an overview. J Psychosom Res. 2002;53(4):849–857 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
